Obesity has become a global health burden, prompting the search for less invasive and safer treatment options for people who are not candidates for major surgery. Endoscopic Sleeve Gastroplasty (ESG) is an endoscopic procedure in which stitches are placed inside the stomach to form folds that reduce its size without having to cut or remove part of the stomach.
According to a systematic review and data from a 5-year follow-up center, the average overall weight loss in patients was about 15-16% after one year, with good stability of results after five years, and a moderate complication rate. ESG surgery is a promising option for those with a moderate or high BMI who want to lose weight with less risk and faster recovery.
What is endoscopic sleeve gastroplasty (ESG)?
Endoscopic Sleeve Gastroplasty (ESG) is a non-surgical procedure that aims to reduce the size of the stomach using an endoscope. A flexible endoscope is inserted through the mouth with a special suturing device, through which serial stitches are made inside the stomach wall to shape it into a smaller tube similar to a sleeve, but without cutting or removing any part of it.
This structural change reduces the amount of food the stomach can accommodate, helping the patient feel full more quickly and eat less. Unlike traditional surgeries, ESG does not require incisions or tissue removal, making it a less invasive and quicker recovery option for patients who do not qualify for surgery or want a safer alternative.
Why is it considered a non-surgical procedure?
Endoscopic Sleeve Gastroplasty (ESG) is classified as a non-surgical procedure because it does not require any incisions in the abdominal wall and does not involve removing or cutting parts of the stomach or intestines. A flexible scope is inserted through the mouth and into the stomach, through which internal sutures that reduce the capacity of the stomach are placed. This technique avoids the risks associated with traditional surgery, such as infection, surgical bleeding, or complications from healing incisions.
In addition, the ESG procedure does not cause permanent changes to the anatomy of the digestive tract, allowing the stitches to be removed or the procedure to be repeated when needed. These characteristics make the procedure less invasive and safer for patients who have contraindications to surgery or prefer a treatment option with a shorter recovery time and faster return to daily activities.
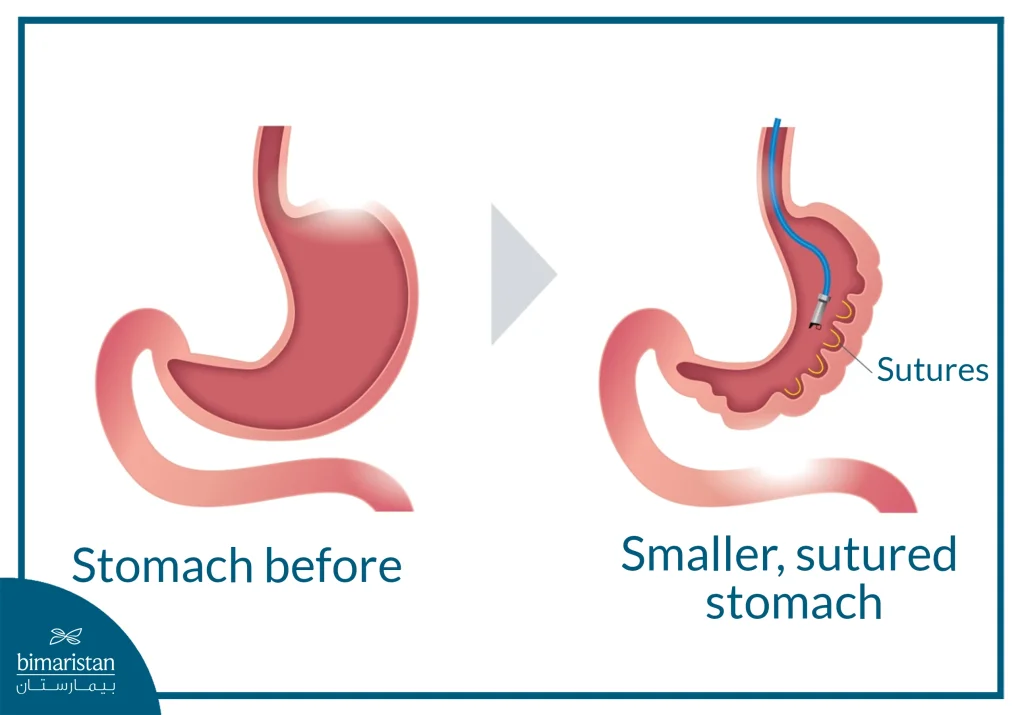
How is endoscopic sleeve gastroplasty (ESG) performed?
Endoscopic sleeve gastroplasty is a non-surgical procedure performed entirely through an endoscope inserted through the mouth into the stomach, without the need for external incisions or removal of parts of the gastrointestinal tract. The procedure is usually performed under general anesthesia or deep sedation and takes about an hour to an hour and a half.
Preparation and anesthesia
Before the procedure begins, the patient undergoes a thorough clinical evaluation, including medical history, laboratory tests, and imaging if necessary. General anesthesia or deep sedation is administered to ensure that the patient is comfortable and pain-free during the procedure.
Inserting the telescope
A flexible endoscope is inserted through the mouth, down the esophagus and into the stomach. The endoscope is equipped with a high-definition camera and an automated suturing tool that enables the doctor to see and work inside the stomach.
Placing internal stitches
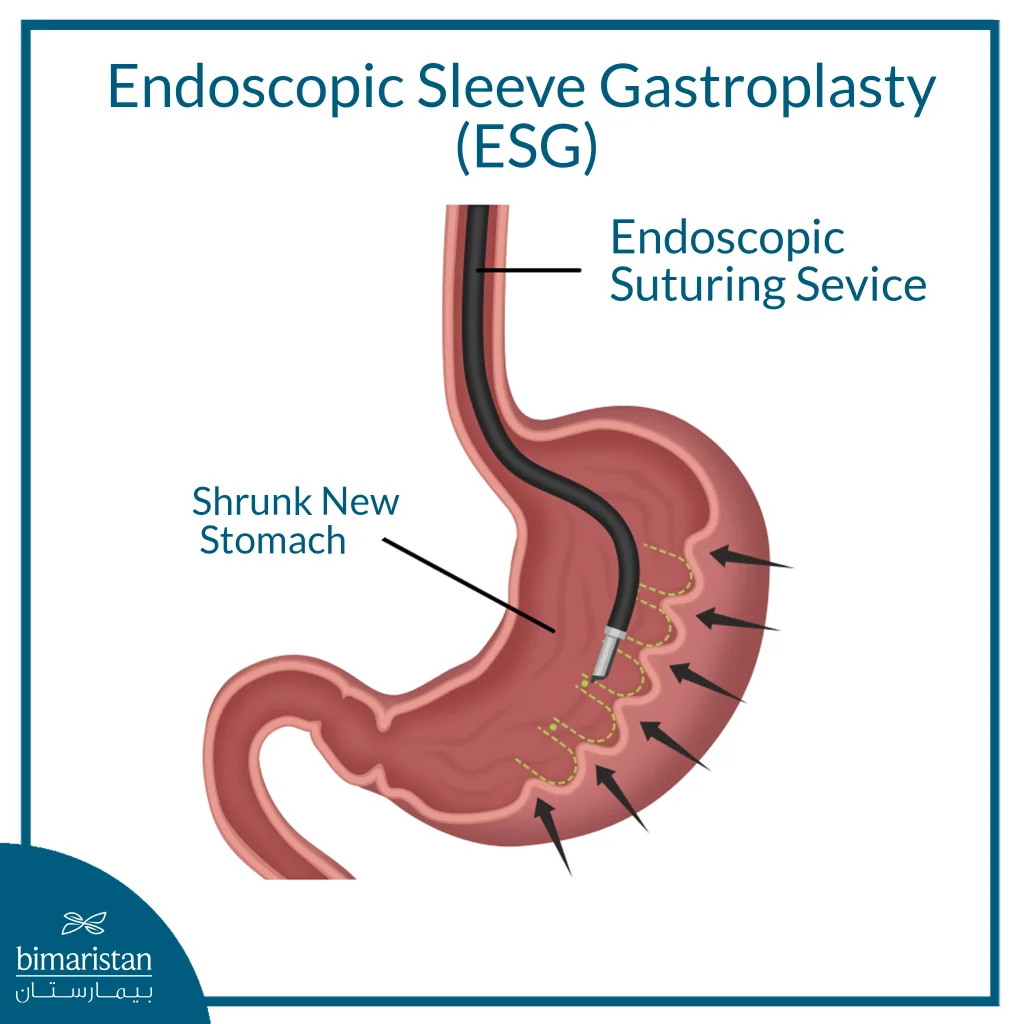
Using an Endoscopic Suturing System, your doctor makes a series of longitudinal stitches in the stomach wall, usually in sequence from near the mouth of the stomach downward. These stitches tighten the stomach wall to shape it into a smaller tube.
Stomach reduction
After suturing, the stomach capacity is reduced by up to 70-80% compared to the normal size, which reduces the amount of food that can be eaten and increases the feeling of early satiety.
Finalizing the procedure and recovery
After making sure the stitches are secure and there is no bleeding, the scope is withdrawn, and the patient is taken to the recovery room. The patient can often leave the hospital the same day or the next day with dietary and lifestyle instructions.
Features and benefits compared to traditional surgery
Endoscopic sleeve gastroplasty (ESG) offers a number of significant advantages when compared to traditional abdominal surgery for the treatment of obesity:
- Faster recovery: Often discharged from the hospital within 24 hours.
- Retractability: The ability to remove stitches or repeat the procedure when needed.
- Higher safety: Lower rate of surgical complications such as infection and bleeding.
- Improved quality of life: Significant weight loss while minimizing the risk of major operations.
- Less invasive procedure: It is done through the mouth using an endoscope without the need for incisions.
- No permanent changes in the anatomy of the digestive system: no cutting or resection of the stomach or intestines.
Low risk and recovery time
The main advantage of the ESG procedure is that it avoids the common complications associated with traditional surgery, such as leaking surgical lines or infection at the incision site. Due to the absence of abdominal incisions, post-operative pain is limited, and patients usually do not require an extended hospital stay. Patients are often able to return to their daily activities within a few days, which is an important difference compared to sleeve gastrectomy or bypass, where recovery takes weeks longer.
Reverseability and Repeatability
Unlike traditional surgeries that make permanent changes to the stomach or intestines, the ESG procedure uses retractable stitches. In some cases, these stitches can be removed, or the procedure can be repeated if necessary, giving additional treatment flexibility to patients and doctors. This feature makes the procedure a suitable option for people who are reluctant to undergo irreversible surgical intervention.
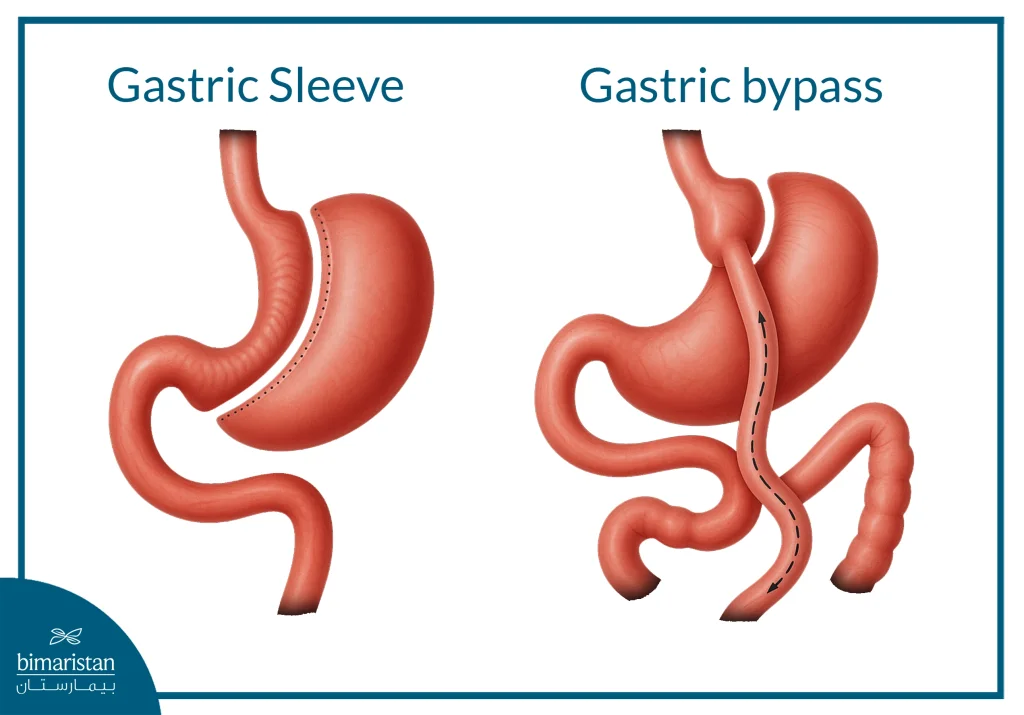
Comparing ESG with other operations (sleeve gastrectomy, bypass, balloon, belt)
ESG is a middle step between non-surgical treatments, such as a gastric balloon, and major surgical procedures, such as sleeve gastrectomy and gastric bypass. Weight loss after ESG is typically greater than a balloon or gastric band, but less than a surgical sleeve or gastric bypass. ESG is characterized by lower surgical risks and a faster recovery time, making it a suitable option for patients with a medium to high BMI who do not want a permanent surgical intervention. ESG is a complementary option in the obesity treatment spectrum, combining relative effectiveness with high safety compared to other procedures.
Possible complications and issues after endoscopic sleeve gastroplasty (ESG)
Although endoscopic sleeve gastroplasty (ESG) is a safe procedure compared to traditional surgery, like any medical intervention, it can be associated with some complications and side effects. These issues are often temporary and mild, and rarely rise to the level of serious complications. Possible complications include
- Nausea and vomiting: These are the most common symptoms after the procedure, especially in the early days. These symptoms usually respond to drug treatment and gradually improve within a week.
- Intragastric bleeding: A rare complication that occurs at the site of the stitches and is often managed with medication or endoscopic re-intervention without the need for surgery.
- Infection: Infections after ESG are very rare, as there are no external incisions, but if they do occur, they may require antibiotics or close monitoring.
- Abdominal pain or gastric discomfort: The patient may experience abdominal pain or cramping as a result of the internal stitches and the reduction in the size of the stomach. These pains are often temporary and can be treated with simple painkillers.
- Stitches fail or lose their effectiveness over time: Some sutures may loosen over the long term, leading to an increase in stomach size again and the need for a repeat procedure or conversion to surgery.
- Gastroesophageal reflux disease (GERD): Reflux symptoms such as heartburn or acid reflux may increase in some patients after the procedure, but they are usually mild and can be controlled with acid-suppressing medications.
- Rare and serious complications, Such as perforation of the stomach or injury to neighboring organs, are exceptional cases with a very low rate compared to major surgeries.
Long-term results and candidates for the process
Long-term results
Endoscopic sleeve gastroplasty (ESG) has proven to be remarkably effective for medium- and long-term weight loss. Clinical data suggest that patients may achieve a weight loss of 15-20% of total weight within the first year after the procedure, with good results lasting up to five years when adhering to a healthy lifestyle. In addition, many patients have shown improvement in obesity-related diseases such as type 2 diabetes, hypertension, and sleep apnea. Although weight loss with ESG may be less than that seen after sleeve gastrectomy or bypass, it is balanced by a lower complication rate and faster recovery.
Candidates for the operation
ESG is a suitable option for a specific category of patients, especially:
- Those who have a body mass index (BMI) between 30 and 40 and have been unsuccessful in losing weight with diet or medication
- Patients with obesity-related complications who are not candidates for major surgery due to anesthesia risks or comorbidities
- People who prefer a less invasive and reversible procedure compared to permanent surgery
- Patients who want to lose significant weight while preserving stomach anatomy without resection or clipping
Tips after Endoscopic sleeve gastroplasty (ESG)
Long-term success after endoscopic sleeve gastroplasty is not only dependent on the procedure itself, but requires a serious commitment to lifestyle changes:
- A gradual diet: The patient starts with clear liquids, then progresses to soft foods, and finally to solid foods within weeks, as instructed by the medical team.
- Adhere to a balanced diet program: Preferably under the supervision of a nutritionist to ensure the body gets the necessary vitamins and minerals.
- Regular physical activity: Perform aerobic and resistance training to support weight loss and maintain muscle mass.
- Regular medical follow-up: See your doctor regularly to monitor results and early detection of any complications or nutritional issues.
- Psychological and behavioral support: Taking advantage of counseling or behavior modification programs can help establish long-lasting, healthy habits.
- Nutritional supplements, if needed: Vitamins and minerals may be recommended, especially if food intake is limited.
- Chew food slowly and in small portions: to avoid nausea and vomiting, and to take advantage of the reduction in stomach size.
Advantages of Endoscopic Sleeve Gastroplasty (ESG) in Turkey
- Low cost: Endoscopic sleeve gastroplasty in Turkey is typically up to 50-70% less expensive compared to the US or Europe, while maintaining the same quality of medical care. This difference makes Turkey an attractive option for patients looking for effective and affordable solutions.
- Internationally accredited hospitals: Turkey has a large number of JCI (Joint Commission International) accredited hospitals and medical centers, ensuring that they adhere to international standards of quality and safety.
- Doctors’ expertise and precise specialties: Many doctors in Turkey have received advanced training in Europe and America, and have extensive practical experience in bariatric surgery and modern endoscopic procedures such as ESG, which enhances the efficiency and success of the procedure.
- Short waiting time: The ability to schedule a procedure quickly, without the long waiting lists common in some European countries, provides convenience and speed in obtaining treatment.
- Advanced medical infrastructure: Hospitals are equipped with state-of-the-art operating rooms, advanced intensive care units, and advanced laparoscopic equipment that supports the laparoscopic sleeve gastrectomy procedure with the highest safety standards.
- Comprehensive services for international patients: These services include translation, medical coordination, transportation to and from the airport, and integrated treatment packages that combine surgery, accommodation, and post-operative care.
- Government support for medical tourism: Turkey offers a favorable regulatory environment, with streamlined procedures and ongoing development to attract international patients.
Endoscopic sleeve gastroplasty (ESG) has been shown to be an effective and practical option for weight loss in patients who have not achieved adequate results with diet or medication. The procedure is less invasive, with a faster recovery period and a lower complication rate compared to traditional surgery. Long-term results show good efficacy in weight loss and amelioration of obesity-related diseases when medical follow-up and a healthy lifestyle are adhered to. ESG has the added advantage of being reversible or repeatable when needed, making it a flexible option for many patients. The choice of this procedure should be part of a thorough evaluation by the medical team to determine if it is appropriate based on BMI and overall health status.
Sources:
- Ng, S. K.-K., & Teoh, A. Y.-B. (2025). Endoscopic sleeve gastroplasty – Current status and future perspectives. Digestive Endoscopy, 37(6), 601-610.
- Matteo, M. V., Gualtieri, L., Bove, V., Palumbo, G., Pontecorvi, V., De Siena, M., Barbaro, F., Spada, C., & Boškoski, I. (2024). Endoscopic sleeve gastroplasty for metabolic dysfunction-associated steatotic liver disease. Expert Review of Gastroenterology & Hepatology, 18(8), 397-405.
- Abu Dayyeh, B. K., Bazerbachi, F., Vargas, E. J., Sharaiha, R. Z., Thompson, C. C., Thaemert, B. C., Teixeira, A. F., Chapman, C. G, Kumbhari, V., Ujiki, M. B., Ahrens, J., Day, C., MERIT Study Group, Galvao Neto, M., Zundel, N., & Wilson, E. B. (2022). Endoscopic sleeve gastroplasty for treatment of class 1 and 2 obesity (MERIT): a prospective, multicentre, randomized trial. The Lancet, 400(10350), 441-451.
- Ang, J.-W., & Chen, C.-Y. (2020). Current status of endoscopic sleeve gastroplasty: An opinion review. World Journal of Gastroenterology, 26(11), 1107-1112.