The treatment of early esophageal tumors has advanced significantly with the rise of modern endoscopic techniques. Esophageal ESD (Endoscopic Submucosal Dissection) stands out as one of the most effective approaches, enabling precise removal of superficial tumors and abnormal lesions without the need for open surgery. This technique offers both immediate tumor management and the advantage of obtaining a detailed histological diagnosis, enhancing clinical outcomes and minimizing the risks typically associated with conventional surgical methods.
What is the esophagus?
The esophagus is a muscular tube that connects the pharynx to the stomach, and works to transport food and liquids after swallowing towards the stomach through contractile movements called the gastric movement. The esophagus is about 25 centimeters long and contains a sensitive mucosal lining that is constantly exposed to the effects of food, microbes, and stomach acid. The esophagus can be affected by several conditions, including chronic infections, ulcers, strictures resulting from old wounds, benign tumors, and early esophageal tumors or precancerous changes such as Barrett’s esophagus.
These conditions can affect esophageal function and increase the risk of complications if left untreated. Advanced treatment techniques such as Esophageal Endoscopic Submucosal Dissection (EESD) have been developed to remove superficial lesions or early tumors with high precision, while preserving normal esophageal function and minimizing the need for conventional surgical intervention. These techniques combine treatment and histologic diagnosis in a single step, improving treatment outcomes and minimizing risks to the patient.
What is Esophageal Endoscopic Submucosal Dissection (EESD)?
Esophageal Endoscopic Submucosal Dissection (EESD) is an endoscopic procedure used to treat and completely remove early superficial tumors in the esophagus. This procedure allows lesions to be removed without the need for partial or total esophagectomy, preserving normal esophageal function and minimizing the complications associated with conventional surgery.
The procedure utilizes a flexible endoscope with a camera and precise surgical instruments. The doctor injects a special solution under the tumor to lift it from the deeper layers, and then carefully removes the tumor using specialized power tools. This approach enables the assessment of the type and extent of the tumor through a complete histological sample, thereby combining treatment and diagnosis in a single step. Endoscopic esophageal submucosal dissection is usually performed in specialized medical centers. It is an effective treatment option for patients with superficial esophageal tumors, especially early tumors that have not penetrated the deeper layers.
When is Esophageal Endoscopic Submucosal Dissection (EESD) indicated?
Esophageal Endoscopic Submucosal Dissection is an important treatment option for the treatment of early superficial tumors in the esophagus. This procedure is utilized to treat specific lesions without the need for major surgical intervention. The choice of procedure is based on the type and size of the lesion, the depth of its spread, and the risk of it transforming into esophageal cancer. The main indications for using this procedure include:
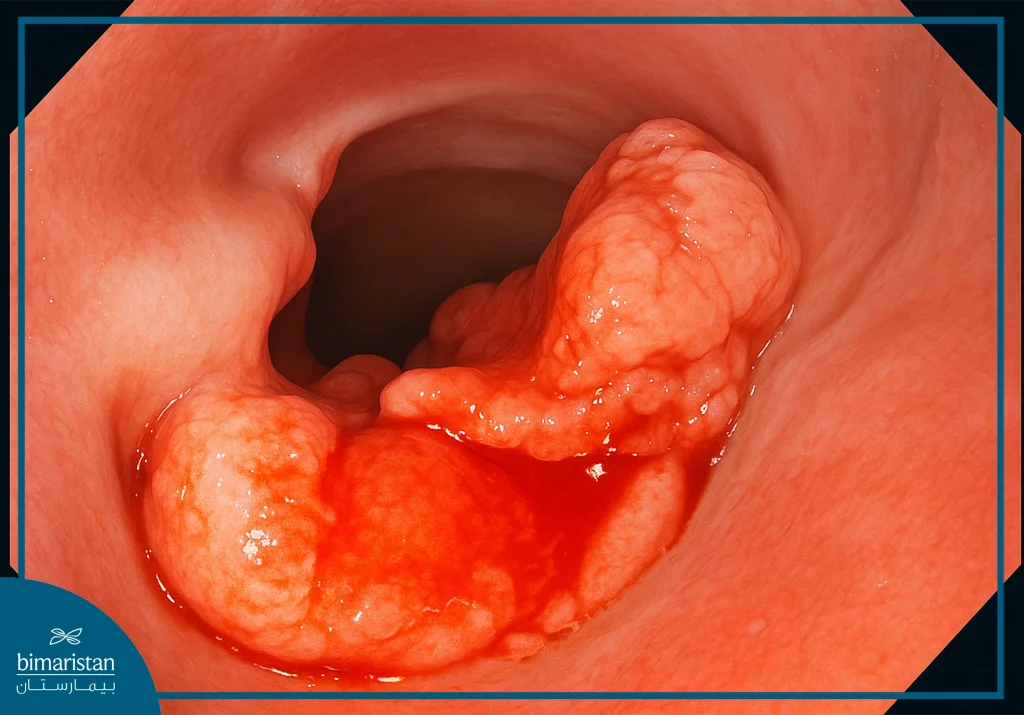
- Early superficial tumors of the esophagus: Tumors that have not penetrated the deeper layers of the esophagus are removed to ensure complete removal and reduce the risk of relapse.
- Barrett’s esophagus and precancerous lesions: Cellular changes in the lining of the esophagus in patients with Barrett’s esophagus are an essential precursor to dissection, especially when early tumor cells are present.
- Polyps or limited lymph nodes: In some cases, large benign lesions or small lymph nodes within a limited mucosal range are removed using this procedure instead of surgery.
- Lesions that are difficult to reach with conventional methods: Some tumors may be large or in difficult locations, such as the lower esophagus near the stomach, making submucosal dissection the best option.
- Other esophageal diseases: Esophageal tumors associated with chronic infections, non-healing ulcers, or strictures from old wounds are sometimes removed to avoid long-term complications.
Esophageal endoscopic submucosal dissection provides effective results with high success rates and minimizes the need for conventional surgery, although a specialized medical team must evaluate each case to determine the appropriateness of the procedure based on the characteristics of the lesion and potential risks.
Steps of Esophageal Endoscopic Submucosal Dissection
Esophageal Endoscopic Submucosal Dissection is an advanced endoscopic procedure used to remove early superficial tumors or abnormal lesions in the lining of the esophagus. The success of the procedure depends on careful preparation before the procedure, adherence to specific technical steps during the dissection, and ensuring that histological samples are taken to confirm the diagnosis.
Preparation before the procedure
- Assessment of the patient’s general condition: This includes a comprehensive clinical examination, evaluation of cardiopulmonary function, and basic laboratory tests to minimize the risks associated with anesthesia and surgery.
- Imaging and dissection planning: Upper gastrointestinal endoscopy, sometimes combined with ultrasound imaging, is used to accurately determine the size and location of the lesion and the depth of penetration into the different layers of the esophagus.
- Gastrointestinal preparation and patient fasting: Fasting is usually required for an average of 7 hours before the procedure to empty the stomach and reduce the risk of vomiting or aspiration during anesthesia.
- Determine the type of anesthesia: Often done under general anesthesia or deep local anesthesia, depending on the size of the lesion and the patient’s condition, with careful monitoring of vital functions.
Stages of Esophageal Endoscopic Submucosal Dissection
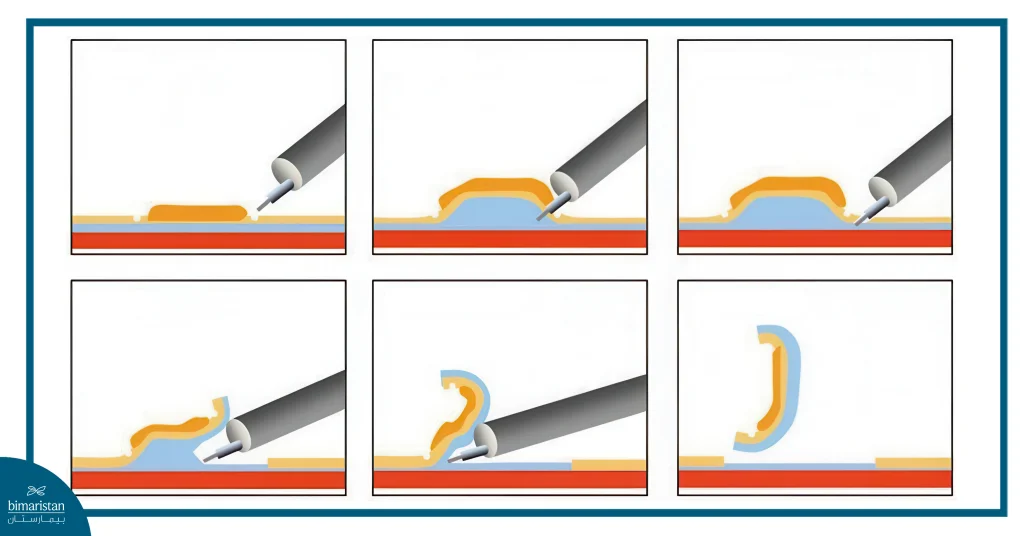
- Accurately delineate the boundaries of the lesion: This is done using special dyes or color fluoroscopy to clarify the tumor boundaries and distinguish between healthy and diseased tissue.
- Injecting a solution under the lesion: The solution lifts the lining of the esophagus from the deeper layers, reducing the risk of perforation during dissection and making it easier to remove the tumor.
- Careful dissection of the mucosa: Utilizing precise electrical instruments, the lesion is meticulously separated from the underlying layers, ensuring it is removed in one piece whenever possible for accurate diagnosis.
- Bleeding control: During the procedure, blood vessels are carefully monitored, and any bleeding is promptly treated using specialized endoscopic tools like electrocautery or small clips.
- Examine the site after dissection: Ensure that all affected esophageal tissue has been removed, and examine the area for any residue, and any small strictures or tears can be treated immediately.
Tissue sampling during the procedure
All excised tissue is sent to a laboratory for histological evaluation. This evaluation assesses various factors, including the depth of penetration, the boundaries of the tumor, and the presence of pre-cancerous or cancerous cells. Combining treatment and diagnosis in a single step leads to improved outcomes and reduces the need for further interventions.
Possible complications after esophageal endoscopic submucosal dissection
Although esophageal endoscopic submucosal dissection is a precise and safe procedure, some complications may arise after the procedure and require careful follow-up by the medical team:
- . Bleeding: Bleeding may occur during or after the procedure and is the most common. The area is continuously monitored and can be controlled immediately, minimizing the need for additional surgical intervention.
- Esophageal perforation: Occurs when the esophageal wall is accidentally breached during removal of the lesion. The perforation is often discovered during the operation and is treated immediately with clips or stents, rarely requiring additional surgical intervention.
- Strictures of the esophagus: Strictures may form after the removal of large or long-distance tumors, making it difficult to swallow. They are usually treated with balloon dilation or special endoscopic instruments to restore normal esophageal function.
- Gastroesophageal reflux disease (GERD): May occur especially if the operation involves the lower part of the esophagus close to the stomach. It is often temporary and treated with anti-acid medications and lifestyle modifications, and rarely requires additional intervention if it is severe or chronic.
- Infection or inflammation: Although rare, localized infections can occur after the procedure and are typically treated with antibiotics and close patient monitoring.
- Temporary symptoms after the operation: Such as pain or mild difficulty swallowing, which gradually improve over a few days with proper medical care.
Recovery and follow-up after esophageal endoscopic submucosal dissection
After an esophageal endoscopic submucosal dissection, the recovery phase begins, which requires careful follow-up to ensure that the esophagus heals properly, minimizes complications, and achieves the best treatment results. Recovery depends on post-operative medical care, regular esophageal check-ups, and a proper dietary lifestyle.
Post-op care
After the procedure, the patient is usually kept under observation for a few hours or overnight, depending on the size of the lesion and the patient’s condition. Vital signs are monitored, and any signs of bleeding or possible perforation are checked, while pain is managed with appropriate analgesics. Patients are advised to rest and avoid any heavy physical exertion in the first few days after the procedure, and are given clear instructions regarding the warning signs to contact the medical team immediately.
Esophageal screening and regular follow-up
Regular follow-up is an essential part of ensuring the success of the operation and minimizing the risk of relapse. Periodic esophagoscopy is usually performed several weeks after resection to ensure that the area is fully healed and for early detection of any altered tissue or strictures. The doctor determines the follow-up schedule based on the size and type of the initial lesion and the results of the histologic examination.
Nutrition and lifestyle after surgery
In the first few days after surgery, patients are advised to follow a bland diet to minimize irritation to the esophagus, such as soft foods and liquids. Solid foods can be introduced gradually depending on the patient’s tolerance. It is also advised to avoid smoking and alcohol, elevate the head during sleep to reduce the risk of reflux, and adhere to antacids if prescribed by the doctor to minimize esophageal irritation and speed up recovery.
Features of treatment in Turkey for esophageal endoscopic submucosal dissection
Turkey is one of the leading providers of Esophageal Endoscopic Submucosal Dissection (EESD), offering specialized medical centers with high expertise in therapeutic endoscopy. Highlights include:
- Advanced medical expertise: Turkey boasts specialized medical teams in therapeutic endoscopy and gastrointestinal surgery, with extensive experience in performing esophageal ESD procedures, which enhances success rates and minimizes complications.
- Using the latest technology and equipment: Turkish centers rely on modern endoscopes and electrical tools, as well as lesion lifting solutions and bleeding control techniques, to ensure the accuracy of the procedure and patient safety.
- Comprehensive post-operative follow-up: Centers provide careful follow-up programs that include regular endoscopy, evaluation of tissue samples, and nutrition and lifestyle advice to ensure that the esophagus heals properly and minimizes the risk of relapse.
- Competitive treatment costs and high quality: Turkey offers high-quality treatments at competitive prices compared to other countries, with complete medical services including counseling, accommodation, and post-operative care.
- Multidisciplinary care: A team of gastroenterologists, anesthesiologists, radiologists, and specialty nurses works together to ensure comprehensive care before, during, and after the procedure.
- Medical travel is easy: Turkey offers a strong medical tourism infrastructure, including accommodation, transportation, and logistics, making treatment more accessible to international patients.
- Post-operative support: The centers focus on providing ongoing follow-up and counseling after the procedure, including nutritional and psychological support, and instructions to prevent potential complications such as GERD or strictures.
Esophageal Endoscopic Submucosal Dissection (ESD) is a cutting-edge and highly effective technique for treating early superficial tumors and Barrett’s esophagus lesions. This minimally invasive procedure enables complete and precise removal of abnormal tissue while preserving esophageal function and reducing the need for conventional surgery. By integrating therapeutic intervention with intraoperative histological assessment, esophageal ESD ensures accurate tumor staging and enhances overall treatment outcomes. It also lowers the risk of complications compared to conventional surgical methods and supports faster recovery, with ongoing medical supervision including routine endoscopy and management of potential issues such as bleeding, strictures, or gastroesophageal reflux disease (GERD).
Turkey has emerged as a leading destination for patients seeking esophageal ESD, offering state-of-the-art medical centers equipped with the latest technologies and supported by multidisciplinary teams that provide continuous care before, during, and after the procedure. These centers also deliver comprehensive follow-up programs, nutritional and psychological support, and full medical travel services, including accommodation. With a strong commitment to quality care and competitive pricing, Turkey presents an ideal environment for safe and precise esophageal ESD treatment, boosting recovery prospects, minimizing risks, and improving post-procedure quality of life.
Sources:
- Okubo, Y., & Ishihara, R. (2023). Endoscopic submucosal dissection for esophageal cancer: current and future. Life, 13(4), 892.
- Zhao, S. H., & Wang, J. (2018). Is endoscopic submucosal dissection of early esophageal cancer ready for prime time? Clinical Gastroenterology and Hepatology, 16(5), 684-686.