Esophageal perforation refers to a rupture or tear in the esophagus, the muscular tube connecting the mouth to the stomach. When this condition occurs, esophageal contents may escape into the chest cavity, particularly the mediastinum, potentially causing a severe and life-threatening infection known as mediastinitis.
The majority of esophageal perforation cases result from iatrogenic injuries during medical procedures, most notably endoscopy. Although the adoption of flexible instruments has lowered the incidence, it remains the leading cause. Additional causes include elevated intraesophageal pressure from forceful vomiting (Boerhaave’s syndrome), ingestion of sharp objects or corrosive substances, malignancies, and external trauma.
What is the esophagus?
The esophagus is a hollow muscular tube that connects the pharynx to the stomach and is about 25 centimeters long in adults. Its main role is to transport food and drink in a coordinated manner from the mouth to the stomach, thanks to a muscular movement known as peristalsis, which pushes the contents downward. The esophagus passes through the neck and chest to the abdomen. It is surrounded by many vital organs, such as the trachea, lungs, and heart, making any injury to the esophagus extremely dangerous.
The esophageal wall is made up of several layers: An inner mucosal layer, a submucosal layer, a muscular layer responsible for contractions, and a thin outer layer. Although the esophagus does not digest food like the stomach and intestines, its integrity is essential to ensure the normal passage of food without leakage or reflux. Any defect in its structure or perforation can lead to serious complications, given its proximity to major blood vessels and respiratory organs.
What is esophageal perforation?
Esophageal perforation is a rupture or hole in the esophageal wall, the muscular tube responsible for transporting food and liquids from the mouth to the stomach. When perforation occurs, esophageal contents such as food, saliva, and gastric secretions can leak into the chest cavity (mediastinum), leading to severe contamination and inflammation of surrounding tissues, a condition known as mediastinitis. Although rare, esophageal perforation is extremely serious and can rapidly progress to a life-threatening infection without prompt medical intervention. It is considered a medical-surgical emergency requiring precise diagnosis and immediate treatment.
Most cases of esophageal perforation stem from iatrogenic injuries during diagnostic or therapeutic procedures, particularly endoscopy involving rigid instruments, though flexible scopes may also pose a risk. Less frequent causes include spontaneous rupture due to sudden pressure spikes during intense vomiting (Boerhaave’s syndrome), ingestion of foreign objects or corrosive agents, esophageal tumors, blunt or penetrating trauma to the chest, and ulceration from chronic gastroesophageal reflux. Given the critical nature of this condition, any delay in diagnosis or treatment significantly raises the risk of complications such as systemic infection, abscess formation, and respiratory or circulatory collapse.
Causes of esophageal perforation
Esophageal perforation is caused by several factors, most of which are related to medical procedures, but other causes can lead to the rupture of the esophageal wall under certain circumstances. Here are the most common causes of esophageal perforation:
- Medical injuries (iatrogenic perforation): The most common cause of esophageal perforation, resulting from diagnostic or therapeutic procedures such as endoscopy, balloon dilation, or surgery near the esophagus.
- Spontaneous perforation (Boerhaave syndrome): This occurs when the pressure inside the esophagus suddenly rises due to severe vomiting or exertion, and is the most serious form of perforation.
- Swallowing foreign objects or caustic substances: Sharp bones, disc batteries, or corrosive chemicals (such as detergents) may cause a tear or weakening of the esophageal wall.
- External injuries or direct trauma: Stabbings, traffic accidents, and penetrating injuries to the chest and neck.
- Chronic esophageal diseases: Tumors, ulcers associated with gastroesophageal reflux disease (GERD), reflux esophagitis, or eosinophilic esophagitis may weaken the wall and increase the likelihood of perforation.
- Other rare causes: Esophageal perforation caused by balloon dilation of strictures, or as a complication of drug-induced esophagitis.
Symptoms of esophageal perforation
Symptoms of esophageal perforation can vary based on the location of the perforation. However, they generally share the characteristic of developing quickly and indicating a medical emergency. Here are the most common symptoms associated with a perforation:
- Sudden, severe pain: Usually appears in the chest or upper abdomen, but may spread to the shoulder or back.
- Dysphagia & Odynophagia: Difficulty and pain while swallowing, an early sign that accompanies an esophageal rupture and gradually increases.
- Shortness of breath and respiratory symptoms: Rapid breathing or chest tightness and Hamman’s sign, a popping sound synchronized with the heartbeat, may be heard when there is air in the mediastinum.
- Generalized systemic symptoms: These symptoms include fever, rapid heartbeat, low blood pressure, and tremors due to leakage of esophageal contents and early inflammation or infection.
- Local signs depending on the location of the perforation:
- In the neck: pain, stiffness, hoarseness, and subcutaneous emphysema.
- In the chest: pain behind the sternum, pleural effusion, roughness or crackling under the skin.
- In the abdomen: epigastric pain, nausea and vomiting, or signs of peritonitis.
Diagnosis of esophageal perforation
Confirmation of esophageal perforation primarily relies on imaging tests that reveal indirect signs of leakage or the presence of air outside the esophagus. Enhanced imaging techniques help identify the precise location of the tear and its associated features. Here are the main diagnostic methods used:
Initial clinical examination
Clinical assessments look for respiratory and circulatory signs such as shortness of breath, fever, tachycardia, low blood pressure, pain or stiffness in the neck or chest, and possibly subcutaneous emphysema with cervical rupture.
Chest X-ray
It is the first imaging step and may show air in the mediastinum, pleural effusion, mediastinal shadow dilatation, subcutaneous air, or free air under the diaphragm in cases of abdominal perforation.
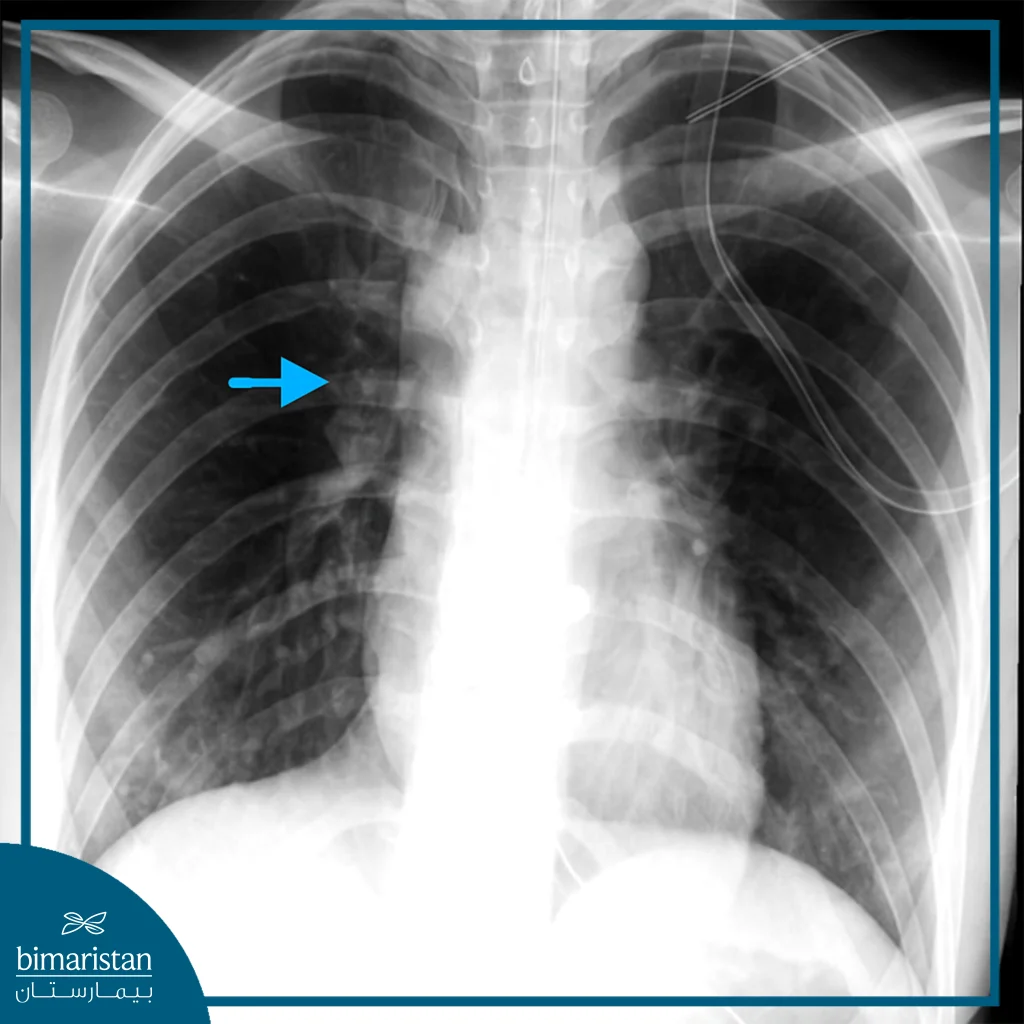
Contrast Esophagography
The preferred test for confirming the diagnosis, as it reveals any leakage of contrast material from the esophagus. This test is crucial for assessing the location and extent of the rupture. It is advisable to use an aqueous dye to reduce the risk of mediastinitis. If the result is negative but there is still a strong suspicion of a rupture, barium can be used to enhance the sensitivity of the test.
Computerized tomography (CT scan)
Used for evaluation when the diagnosis is unclear or complications are suspected, it can detect fluid accumulations or air around the esophagus, pleural effusions, or abscesses, and makes it easier to pinpoint the exact location of the perforation.
Endoscopy
If radiological examinations cannot determine the cause and the clinical presentation is strong, we can use endoscopy to aid in the diagnosis; however, its use should be cautious, as the air used during the examination may worsen the perforation.
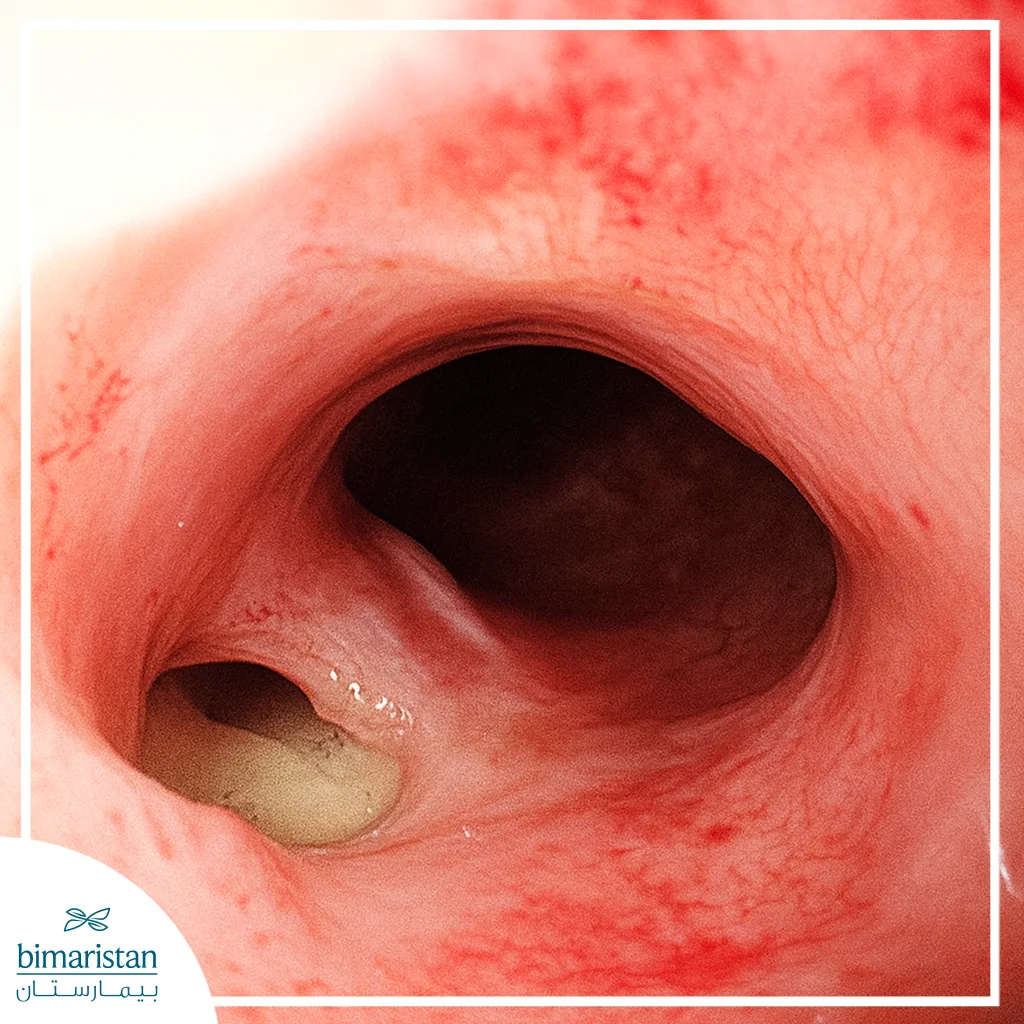
Methods for treating esophageal perforation
The choice of perforation treatment method depends on the size and location of the perforation, the time of diagnosis, and the patient’s clinical condition. Conventional surgical intervention is favored in cases of large perforation or delayed diagnosis with signs of inflammation or septicemia. Endoscopic treatment is often applied for small to medium tears that can be contained with stents or clips. Conservative treatment is an option in stable cases with limited perforation, provided there is no extensive infection or systemic shock.
Conventional surgical treatment
- Preoperative preparation and evaluation: Begins with stabilization of circulation, administration of broad-spectrum antibiotics, and placement of a nasogastric tube to empty the stomach.
- Appropriate surgical access: Determined based on the location of the perforation (neck, chest, or abdomen).
- Identify the location of the perforation: Carefully open the mediastinum or chest cavity to assess the extent of the damage.
- Primary repair: Sew the tear with separate sutures and cover the suture with a supportive tissue such as pleura or intercostal muscle.
- Washing and draining: A thorough wash of the mediastinum or chest with multiple drainage tubes.
- Resection: Performed if repair is not possible or if there is a severe tumor or fibrosis.
- Reconstruction: Pulling out the stomach or colon as a replacement for the esophagus when needed.
- Post-operative care: Close monitoring in intensive care with nutritional support and imaging follow-up.
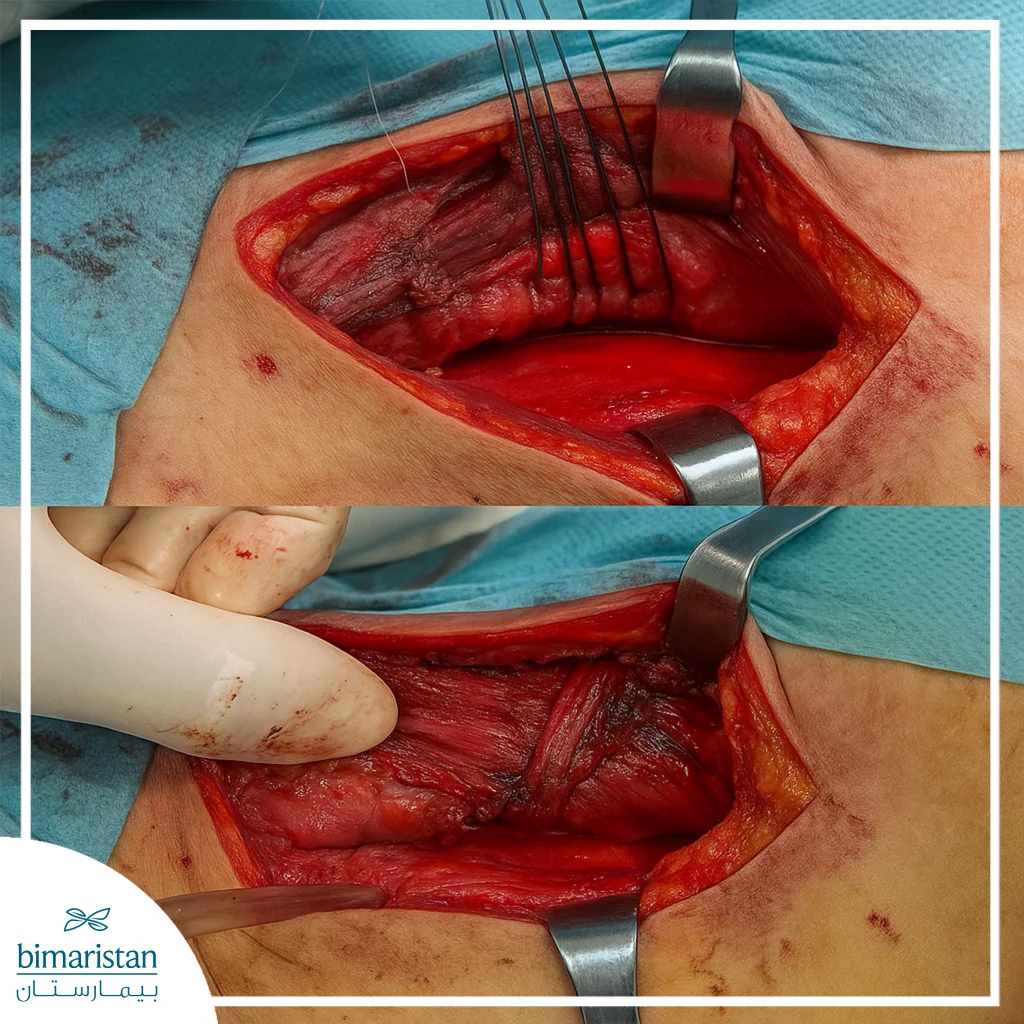
Endoscopic treatment
- Initial endoscopic evaluation: Determine the exact location and size of the perforation.
- Clips closure: Effective for small to medium tears.
- Stent placement: Used for larger perforations to cover the rupture and allow for healing.
- Endovascular vacuum therapy (EVT): Inserting a sponge attached to a vacuum device to remove fluid and promote healing.
- Device removal and follow-up: After the healing period, the stent or sponge is removed, and the esophageal wall is re-evaluated.
Conservative (non-surgical) treatment
In cases of esophageal perforation where the tear is small, localized, and the patient remains clinically stable without signs of systemic infection or significant inflammation, conservative management is the preferred approach. This approach involves strict abstinence from oral intake (NPO) and the administration of total parenteral nutrition (TPN) to maintain nutritional support. Broad-spectrum antibiotics are delivered intravenously, and a nasogastric tube is placed to empty the stomach and reduce intra-esophageal pressure. If fluid accumulation is present, drainage tubes may be inserted to prevent abscess formation. The patient is closely monitored in a hospital setting with regular imaging studies, and surgical intervention is considered if clinical deterioration or failure of conservative therapy is observed.
Complications of esophageal perforation surgery
Although surgery is a lifesaver in most cases of esophageal perforation, this intervention carries the potential for complications that may affect the course of recovery. These complications vary depending on the timing of the diagnosis, the experience of the surgical team, and the general condition of the patient.
- Leakage after repair: Failure to suture the perforation site or poor tissue fusion may lead to recurrent leakage of esophageal contents into the chest or mediastinum.
- Infection and mediastinitis: One of the most serious complications, as the inflammation may develop into a chest abscess or bacteremia.
- Narrowing of the esophagus: Tissue scarring after repair or resection may lead to chronic narrowing and difficulty swallowing.
- Pulmonary complications: These include pleural effusion, pneumonia, or the formation of an esophageal-bronchial fistula as a result of the spread of the infection.
- Bleeding: Bleeding may occur during or after the procedure due to the fragility of the tissue or because of a nearby blood vessel injury.
- Multiple organ failure: In severe or late cases, widespread inflammation can lead to renal failure, systemic shock, or multi-organ failure.
Expectations and follow-up after esophageal perforation treatment
When surgical or endoscopic repair is performed within the first 24 hours, survival rates are significantly higher, reaching reasonable rates in more than three-quarters of cases, while delay causes a severe deterioration in outcomes, with mortality rates reaching more than half after one day and approaching 90 percent after 48 hours. Perforation is a serious condition, even in the best circumstances, with an overall mortality rate of approximately 35% at advanced centers.
After treatment is completed, careful follow-up of the patient is an essential element to minimize complications and improve the chances of full recovery. The follow-up plan includes continuous clinical monitoring for signs of infection or leakage, and periodic imaging tests such as CT scans or contrast swallow to ensure the integrity of the esophagus. Parenteral or gastrostomy tube feeding is relied upon until the affected area is proven to be healed, and then oral food is gradually reintroduced. Monitoring for late complications such as stenosis or abscesses is recommended to ensure long-term patient stability.
Advantages of esophageal perforation treatment in Turkey
Turkey has become one of the top medical destinations for the treatment of complex conditions such as esophageal perforation, thanks to the development of its health infrastructure and the integration of its treatment services:
- Advanced surgical expertise: University hospitals and specialized centers have highly experienced surgeons in thoracic and gastrointestinal surgery, which increases success rates and reduces complications.
- Modern endoscopic techniques: Hospitals offer advanced endoscopic devices that allow for high-precision closure of perforations, reducing the need for extensive surgery.
- Specialized intensive care units: Patients are closely monitored post-operatively in departments equipped with state-of-the-art monitoring and respiratory and cardiac support.
- Competitive treatment costs: Turkey offers advanced medical services with quality comparable to that of European countries, but at lower costs, making it a favourite choice for international patients.
- International accreditation of medical centers: Many Turkish hospitals are accredited by international health organizations, ensuring that they adhere to the highest standards of quality and safety.
Managing esophageal perforation goes far beyond a routine therapeutic procedure; it is a critical test of the medical team’s preparedness and ability to act decisively under pressure. Treatment involves more than simply closing the perforation or repairing damaged tissue; it requires safeguarding the patient from potentially fatal infections, stabilizing vital organ function, and ensuring adequate nutrition until the esophagus regains its normal physiological role. These combined efforts underscore the importance of early diagnosis and rapid intervention as key factors in improving patient outcomes.
Recovery from esophageal perforation does not conclude with a successful surgery or endoscopic repair. It extends into a vigilant follow-up phase focused on identifying early or delayed complications, while providing comprehensive psychological and physical support to help the patient resume normal life. Acknowledging the gravity of this condition and the necessity of multidisciplinary collaboration highlights that esophageal perforation is not merely a surgical emergency; it is a complex clinical challenge that demands expertise, swift action, and seamless coordination across medical specialties to maximize survival and ensure full recovery.
Sources:
- Kassem, M. M., & Wallen, J. M. (2025). Esophageal Perforation and Tears. In StatPearls . Treasure Island (FL): StatPearls Publishing.
- A.D.A.M., Inc. (2024, October 30). Esophageal perforation. In MedlinePlus Medical Encyclopedia. U.S. National Library of Medicine.