Spinal fracture is one of the injuries that directly affects the stability and movement of the body, and its incidence is increasing globally due to the high rates of accidents and falls in different groups. Studies indicate that the incidence of spinal fractures ranges between 5% and 10% of all bone injuries, while the percentage rises to about 20% in the elderly as a result of osteoporosis.
Statistics also show that women after the age of 50 are almost twice as likely to be injured as men. The severity of these fractures varies from simple injuries that can be recovered with conservative treatment to complex cases that may affect nerves or movement. With the development of modern medical care, the chances of recovery are better than ever, thanks to advanced diagnostic and treatment techniques that provide accurate results and minimize the recovery period.
What is a spinal fracture?
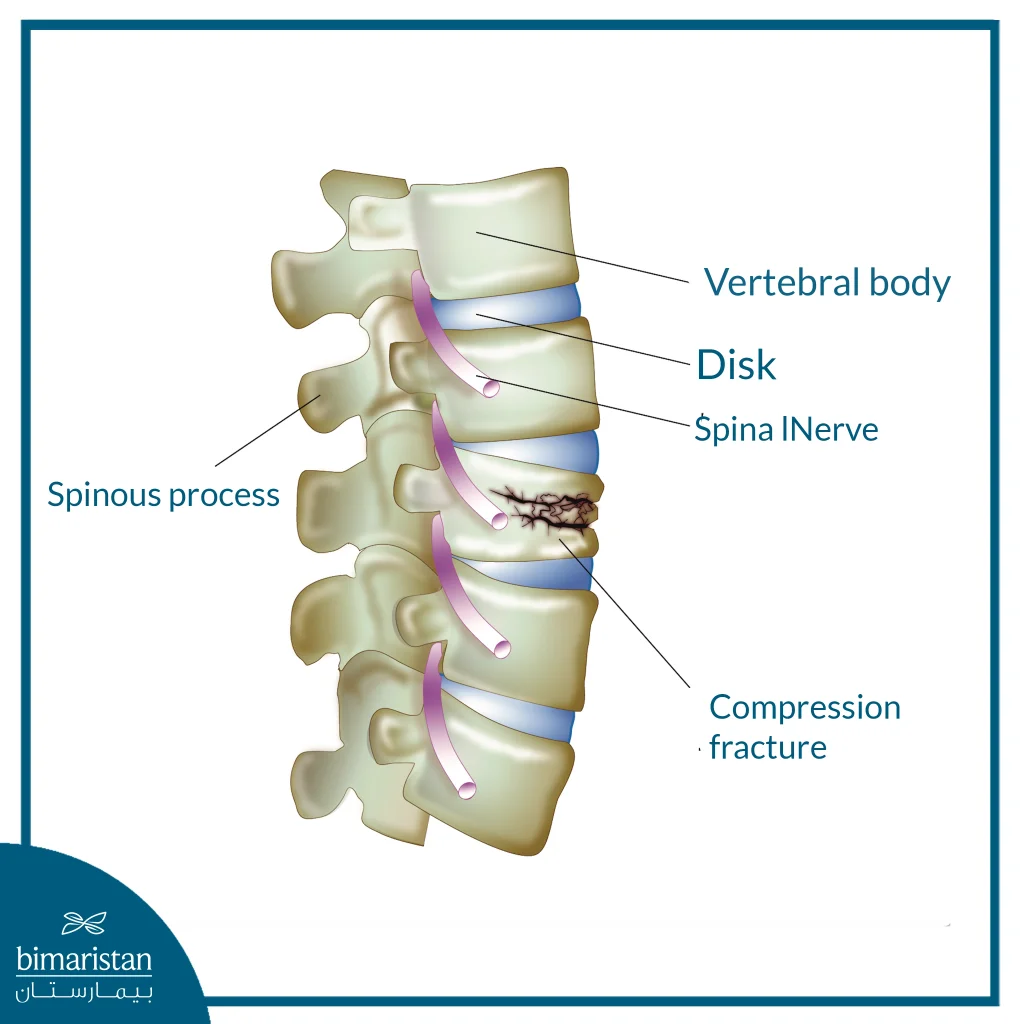
A vertebral fracture is an injury to one or more of the vertebrae of the spine when they are subjected to a force that exceeds the bones’ ability to withstand it. It can be caused by car accidents, falls from height, blunt force trauma, or as a result of weakened bones due to osteoporosis or chronic disease. A compression fracture is often seen in the elderly, where the vertebra collapses and becomes wedge-shaped due to constant pressure.
The severity of a spinal fracture varies according to its location and nature; it may be simple, causing no obvious symptoms or disability, or complex, leading to pressure on the spinal cord or nerves, causing loss of sensation or impaired movement in some cases, the diagnosis depends on clinical examination and imaging such as X-rays, CT or MRI to determine the extent of the damage and make the appropriate treatment decision.
Types of Spinal Fractures
Spinal fractures vary in nature and severity depending on the cause of the injury and the location of the fracture. They can be simple and do not threaten the nerves, or complex, affecting the spinal cord and limiting movement or sensation in some organs, the most important of these types:
- Compression spinal fracture: Occurs when a vertebra collapses due to extreme pressure, often in the thoracic or lumbar region, and is most commonly seen in older people with osteoporosis.
- Explosive spinal fracture: Caused by blunt force trauma that causes a complete collapse of the vertebra, and parts of the bone can spread into the spinal canal, causing pressure on the nerves.
- Slipped or dislocated spinal fracture: It involves the sliding of one vertebra on another with a partial fracture of the bone, and usually leads to spinal instability and requires surgical intervention.
- Direct traumatic spinal fracture: Caused by a sudden accident or forceful injury, such as a sports accident or fall from a height, and may involve injury to the spinal cord or nerves.
Causes of Spinal Fracture
Spinal fractures occur as a result of vertebrae being subjected to forces beyond their ability to withstand or poor structure, and include both mechanical and biological causes, the most important of which are:
- Traffic accidents and trauma: A car hits a passenger or a person falls during an accident, causing extreme pressure on the vertebrae and leading to a fracture or deformity of the spine.
- Chronic diseases: Certain diseases, such as thyroid or parathyroid disorders, affect calcium balance and weaken bones, increasing the likelihood of fractures.
- Osteoporosis: Poor bone density makes vertebrae more prone to fractures even with minor accidents or sudden movements, a common cause in the elderly.
- Falling from a height: Falling from a height generates a lot of force on the vertebrae, especially in the thoracic or lumbar part of the spine.
- Bone tumors or spinal tumors: These cause the vertebrae to erode or weaken their structure, making it easier for a fracture to occur even without significant trauma.
- Bone cancer or bone metastases Can weaken the vertebrae, increasing the likelihood of fractures even without a severe injury.
- Diabetes mellitus: They often have impaired bone healing and fracture healing, making spinal monitoring essential.
Symptoms of a spinal fracture
The symptoms of a spinal fracture vary depending on the type, location, and severity of the fracture, and appear suddenly after trauma or gradually with osteoporotic fractures. Some fractures are simple and do not cause major issues, while complex fractures can affect mobility, nerves, and vital body functions:
- Severe pain in the back or neck: This is the most common symptom, and it increases with movement or pressure on the affected vertebrae, and the pain may extend to the chest or pelvis.
- Loss of sensation or control of organs: In severe cases, a fracture can lead to partial paralysis or loss of control of urine or feces.
- Difficulty moving or sitting: The patient feels unable to bend, walk, or lift objects, which limits daily activities.
- Swelling or bruising in the affected area: Can be seen at the fracture site as a result of internal bleeding or trauma to the surrounding tissues.
- Numbness or weakness in the limbs: This is caused by the pressure of the fracture on the nerves and may appear in the hands or legs, depending on the location of the injury.
- Muscle spasms or weakness: Motor nerves are affected, resulting in loss of coordination or difficulty controlling muscles.
- A change in the general posture of the body, Such as anterior curvature or hunchback, occurs in chronic cases of compression fracture.
Spinal Fracture Diagnosis
Diagnosis of a spinal fracture begins with a clinical examination to determine the extent of the fracture’s impact on movement and nerves, and relies on a range of imaging methods to accurately determine the type, location, and severity of the fracture. Early diagnosis is important to determine the most appropriate treatment and minimize potential complications:
Clinical examination and neurological assessment
The clinical examination includes assessing the patient’s pain, mobility, muscle strength, and sensitivity in the limbs. The doctor will check for any loss of sensation or muscle weakness, as well as the normal curvature of the spine. Neurological evaluation includes testing reflexes and the ability to control urine and feces if needed. This step helps determine if there is pressure on the spinal cord or nerves.
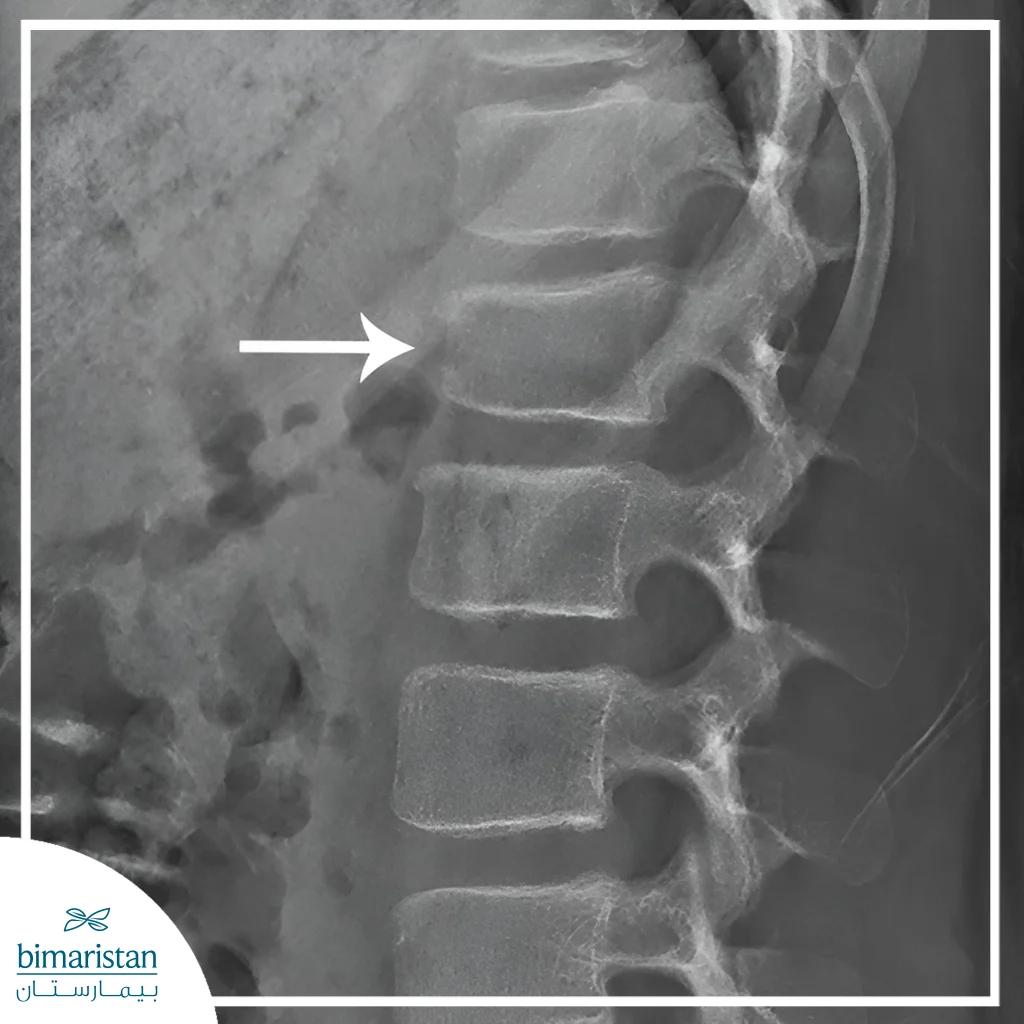
X-rays
X-rays are the first step in imaging to determine the location and type of fracture. Damaged vertebrae are clearly visible and help detect compression or slipped fractures. Multi-angle images can be used to assess the overall stability of the spine before determining the need for any surgical intervention.
Computed tomography
Computed tomography provides detailed images of the injured vertebra, including the surrounding bone and subtle abnormalities. This type of imaging helps to see if the vertebra is fragmented or if there are fragments that may be pressing on the spinal cord, and is essential in planning surgery if the fracture is complex.
Magnetic resonance
MRI allows us to see a precise view of the spinal cord and nerves surrounding the affected vertebra, as well as the soft tissues and cartilage. This test is used to assess nerve compression, internal bleeding, or any ruptured intervertebral discs, as MRI helps in making the most appropriate decision regarding surgery or conservative treatment.
Spinal Fracture Treatment Methods
Spinal fracture treatment depends on the type of fracture, its severity, location, and the condition of the nerves and spinal cord. The goal of treatment is to stabilize the vertebrae, relieve pain, protect the nerves, prevent damage from worsening, and improve mobility. The choice of treatment is based on the severity and stability of the fracture and the extent of nerve damage. Non-surgical treatment is usually used for simple or compression fractures that do not threaten the nerves, while complex, slipped, or burst fractures require surgical intervention to correct the deformity and stabilize the spine, and physical therapy is applied after all methods to strengthen muscles and restore movement, among the most important methods:
Non-surgical treatment
It is used in simple or compression fractures that do not affect the spinal cord and nerves and the spine is relatively stable, where the treatment includes rest for specific periods to relieve pressure on the vertebrae and allow natural healing, the use of belts or splints to stabilize the spine and prevent excessive movement or increased curvature, and the treatment plan includes painkillers and anti-inflammatories to reduce pain and swelling during the recovery phase. After the acute pain is gone, physiotherapy exercises are applied to strengthen the back muscles and muscular support of the spine and improve flexibility and mobility, which helps prevent fracture recurrence and improve overall posture.
Non-surgical spinal stabilization
It is applied in some partially stable or compression fractures that can be stabilized without direct surgical intervention, but require additional support to avoid slippage or increased curvature of the spine. Treatment includes the use of special external stabilization devices to support the spine during daily movement, and follow-up healing through periodic scans to assess the stability of the vertebrae and monitor any changes in posture or pressure on the spinal cord, as this type of treatment helps to allow natural healing of the vertebrae while minimizing complications without the need for complex surgery.

Surgical treatment
It is applied in complex, slipped, or burst fractures, or when there is pressure on the spinal cord or nerves, loss of sensation or muscle weakness, or obvious deformity of the spine. The goal of surgical treatment is to stabilize the spine, protect the nerves, correct the deformity, and prevent the worsening of the curvature or hunch resulting from the fracture:
- Complete anesthesia, preparation, and sterilization of the surgical area
- Opening the incision to access the affected vertebrae while protecting the surrounding nerves and tissues
- Vertebral stabilization using metal screws and plates to stabilize the spine and prevent excessive movement
- Gradually correcting the deformity to normalize the spine
- Neurological examination to make sure there is no pressure on the spinal cord and that the vertebrae are stabilized
- Close the incision with sutures, cover the area with bandages, and then transfer the patient to recovery
- Post-operative follow-up includes muscle strengthening exercises, monitoring of healing, and the use of supportive braces if needed
Medical Advantages of Spinal Fracture Treatment in Turkey
Turkey is considered one of the leading countries in spinal fracture treatment due to the long experience of doctors, the use of the latest surgical techniques, and the provision of integrated health care, which makes treatment effective and reliable:
- The expertise of specialized doctors: Turkey has specialized spine surgeons with many years of experience in treating complex, slipped, and burst fractures, increasing success rates, and minimizing potential complications.
- Modern technologies and medical equipment: Turkish hospitals use advanced imaging equipment such as MRI and CT scans, as well as high-quality spinal stabilization tools to ensure accuracy and safety during surgery.
- Integrated treatment and rehabilitation: The medical centers offer comprehensive programs that include surgical treatment, immobilization, physical therapy, and post-operative rehabilitation plans to ensure restoration of mobility and spinal stability.
- Affordability and additional services: Compared to European and American countries, Turkey offers affordable prices that include treatment, accommodation, and follow-up, as well as access to additional services such as transportation and translation.
- Easy access and support for international patients: Support services are available for international patients, including pre-booking, translation, and assistance with medical procedures, making the treatment experience smoother and more comfortable.
A spinal fracture is a serious injury that requires accurate diagnosis and proper treatment to avoid complications and protect the nerves. The choice of treatment depends on the type of fracture, severity, and location, and may include non-surgical treatment for simple fractures or non-surgical spinal stabilization, while complex cases require surgical treatment to stabilize the spine and correct deformity. Post-treatment rehabilitation is necessary to enhance muscle strength, improve mobility, and restore normal body posture.
Spinal fracture treatment in Turkey offers many advantages, including the expertise of specialized doctors, modern technologies, comprehensive rehabilitation programs, affordable costs, and support for international patients. Patients can visit Bimaristan Medical Center for specialized consultations and quality services. Medical development in Turkey has made surgical and non-surgical spine treatment a safe and reliable experience, increasing the chances of full recovery and restoration of normal life for patients.
Sources:
- Kutsal, F. Y., & Ergani, G. O. E. (2021). Vertebral compression fractures: Still an unpredictable aspect of osteoporosis. Turkish Journal of Medical Sciences, 51(2), 393-399.
- Robinson, D. L., Tse, K. M., Franklyn, M., Zhang, J., Fernandez, J. W., Ackland, D. C., & Lee, P. V. S. (2021). Specimen-specific fracture risk curves of lumbar vertebrae under dynamic axial compression. Journal of the Mechanical Behavior of Biomedical Materials, 118, 104457.
- Roland, H. Fracture of cervical vertebrae. Medical Journal of Australia, 2(24), 732.