Lung cancer remains one of the most widespread and health‑impacting cancers worldwide, and it is frequently diagnosed at advanced stages, making treatment especially challenging. For many years, standard care has centered on surgery, chemotherapy, and radiation, each offering varying levels of success. Immunotherapy for lung cancer has emerged as a transformative approach, aiming to strengthen the immune system so it can target cancer cells in a way that differs from conventional treatments.
What is immunotherapy for lung cancer?
Lung cancer immunotherapy is a type of cancer treatment that uses the body’s natural immune system to fight the disease, also known as biologic therapy. Normally, the immune system protects the body from harmful agents through mechanisms that regulate its activity and prevent it from attacking healthy cells. However, lung cancer cells are particularly challenging because they originate from normal cells, which can sometimes allow them to evade immune recognition. Immunotherapy aims to enhance or restore the immune system’s ability to recognize and attack these cells, helping limit and control the growth and spread of cancer.
Types of immunotherapy used in lung cancer
There are many types of immunotherapies in use or under study for lung cancer, some of which are an integral part of current treatment plans, while others are still in clinical trials.
1. Immune checkpoint inhibitors
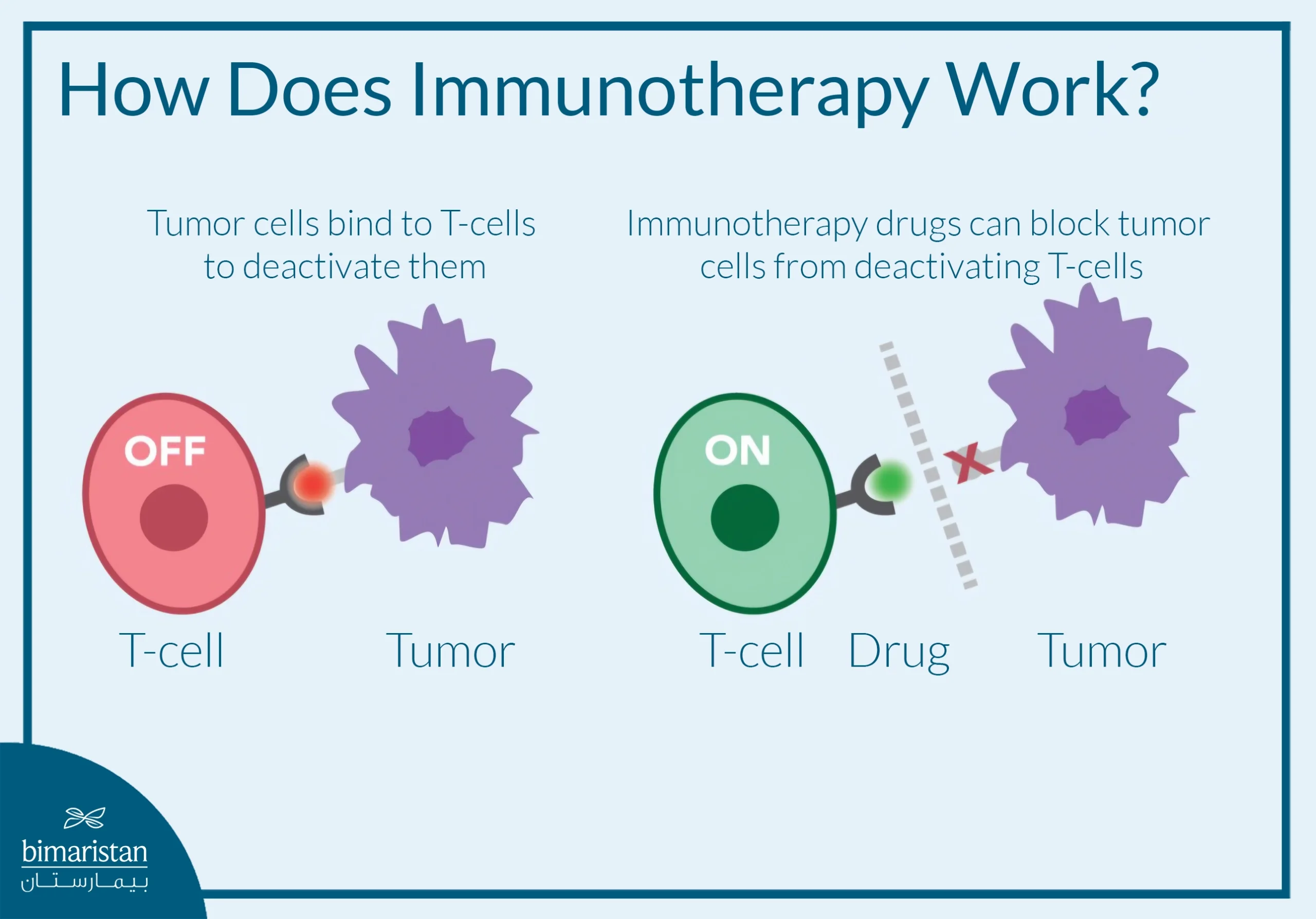
Immune checkpoint inhibitors are the most advanced and widely used type of immunotherapy in lung cancer. These drugs work by disrupting mechanisms that cancer cells use to suppress the immune response. Immune cells contain molecules that regulate the initiation or termination of the immune response, and cancer cells use these molecules to evade immune attack.
Checkpoint inhibitors block this suppression, allowing the immune system to recognize and attack cancer cells. These drugs mainly target pathways such as PD-1, PD-L1, and CTLA-4, and are usually given by intravenous infusion. Also, they may be used alone or in combination with chemotherapy or other immunotherapies.
2. Therapeutic cancer vaccines
Unlike well-known preventive vaccines, therapeutic vaccines aim to treat existing cancer by stimulating the immune system to better kill cancer cells. These vaccines target proteins found in cancer cells that are absent or rarely expressed in normal cells. In some cases, vaccines are tailored to the characteristics of the patient’s own cancer. These vaccines are still being studied in clinical trials, and no lung cancer vaccine has been approved yet.
3. Modified T-cell therapy
This treatment involves extracting T cells from the patient’s body, modifying them in a laboratory to improve their ability to attack cancer cells, and then reintroducing them into the body. The extraction process typically requires a specialized procedure to separate blood components. This type of treatment is still under investigation in clinical trials and is not yet approved for lung cancer.
4. Dual-targeting T-cell therapy
This type of immunotherapy aims to bring T cells closer to cancer cells to enhance the immune attack. This is done through drugs that simultaneously bind to both immune cells and tumor cells that carry certain antigens. This treatment is currently used in some cases of advanced small cell lung cancer.
When is immunotherapy used for lung cancer, and which patients are suitable for it?
Immunotherapy has become an available treatment option for an increasing number of patients with lung cancer, especially in advanced stages of the disease. Many patients receive it as a first‑line treatment, and in some cases, immunotherapy is combined with chemotherapy, or two different immunotherapy agents may be given together. Determining whether immunotherapy is appropriate depends on several factors, including the type of lung cancer, the presence of specific mutations or biomarkers, previous treatments the patient has received, and the patient’s overall health status. Some patients with mild autoimmune diseases may also receive immunotherapy after adjusting their treatment, provided this is done under close medical supervision to determine the most suitable option for each case.
Does immunotherapy differ according to the type of lung cancer?
The use of immunotherapy varies depending on the type of lung cancer. It is more commonly and consistently used in non‑small cell lung cancer, where it has become an essential part of the treatment plan across many stages. In small cell lung cancer, immunotherapy can also be used, but its role is limited to specific situations and stages of the disease. Determining the role of immunotherapy depends on the characteristics of the cancer, as well as the physician’s assessment of the patient’s overall health and the most appropriate treatment strategy, which makes the therapeutic approach differ from one case to another.
Side effects of Immunotherapy for lung cancer
Immunotherapy for lung cancer may trigger an inflammatory response in different parts of the body, and the side effects vary depending on the affected organ and the type of medication used. Most patients experience mild side effects that are manageable and often improve over time, although some effects may be more severe and require close medical monitoring.
Common side effects
Common side effects of immunotherapy include:
- loss of appetite
- General fatigue and exhaustion
- Rash or itchy skin
- Joint and muscle pain
- Coughing or difficulty breathing
- Flu-like symptoms such as fever and chills
- Gastrointestinal disorders such as diarrhea or constipation

Less common side effects
Some less common immune‑related side effects may occur as a result of excessive activation of the immune system, and these include:
- Inflammation of the lungs or heart
- Inflammation of the liver or kidneys
- Inflammation of the intestines
- Endocrine disorders such as thyroid dysfunction
When should I see a doctor?
It is recommended to contact the doctor or medical team if any new or unusual symptoms appear during or after immunotherapy, especially if the symptoms persist or worsen. Some side effects may appear within the first weeks or months of treatment, while others may occasionally develop after treatment has ended. Early communication with the medical team helps assess symptoms and provide appropriate guidance, and in some cases, temporary adjustment of treatment may be required until symptoms improve.
Medical follow-up during immunotherapy for lung cancer
Medical follow‑up is an essential part of the treatment plan for immunotherapy for lung cancer, as it helps evaluate the body’s response to treatment and detect any potential side effects early. During the course of immunotherapy for lung cancer, the patient undergoes regular monitoring by the medical team, which may include clinical examinations and periodic laboratory tests depending on the case and the type of immunotherapy used. Continuous follow‑up also allows the physician to adjust the treatment plan when needed, whether by continuing immunotherapy, pausing it temporarily, or combining it with other treatments, ensuring the best balance between treatment effectiveness and patient safety.
Immunotherapy for lung cancer has brought a significant shift in how the disease is managed by relying on strengthening the immune system and helping it recognize and attack cancer cells. Although this treatment is not suitable for all patients, it has become a key therapeutic option in many situations, especially when patients are carefully selected and closely monitored. Accurate medical evaluation and continuous follow‑up contribute to achieving the greatest possible benefit from treatment while minimizing side effects. In this context, Bimaristan Medical Center is committed to providing comprehensive care based on the latest therapeutic options with meticulous follow‑up for every patient.
Sources:
- American Lung Association. (n.d.). Immunotherapy for lung cancer.
- LUNGevity Foundation. (n.d.). Immunotherapy.

