Tuberculosis is a chronic infectious disease that mainly affects the lungs, and in some cases may extend to other organs in the body if not treated properly. Although drug therapy is the mainstay of TB treatment, there are certain cases in which this treatment alone is not sufficient, especially when complications occur or the response to drugs declines.
In such circumstances, the role of surgery in tuberculosis treatment emerges as a supportive treatment option that aims to deal with serious complications, improve the patient’s condition, and support the effectiveness of drug therapy within a comprehensive treatment plan.
What is tuberculosis?
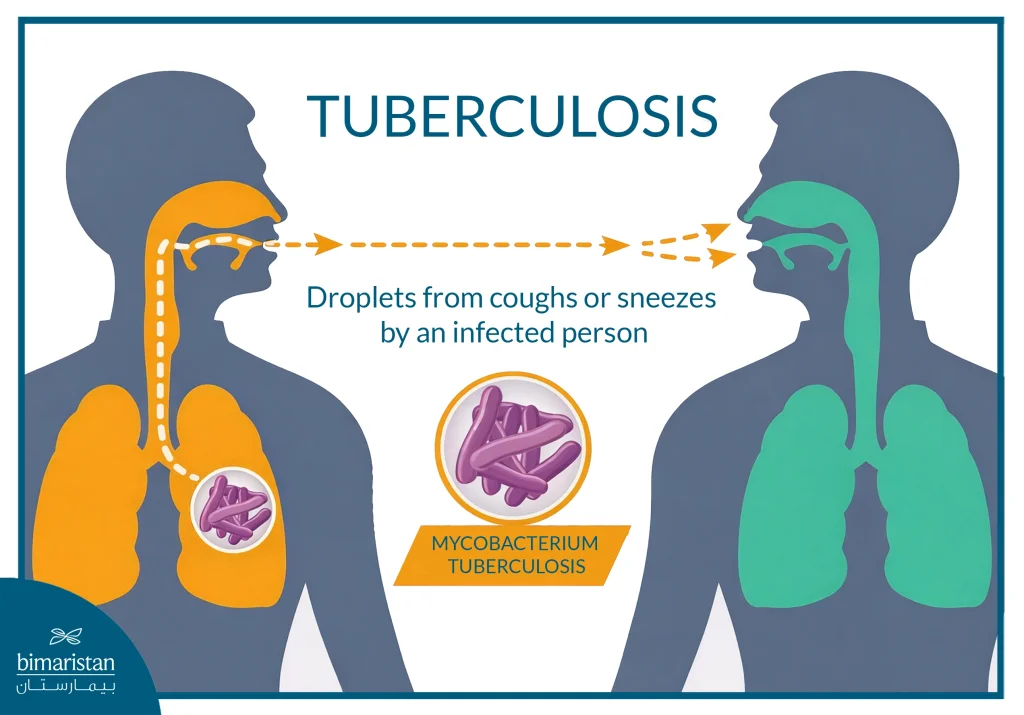
Tuberculosis, or TB, is an infectious disease caused by the Mycobacterium tuberculosis bacteria that most commonly affects the lungs, but can also affect other organs such as the brain, spine, kidneys, or bones. TB is transmitted through the air when a person with active TB coughs, sneezes, or talks, as fine droplets containing the bacteria are spread and inhaled by others.
The likelihood of infection increases in crowded places or when the immune system is weak, and not all people exposed to the bacteria develop symptoms, as the infection may remain latent for long periods without symptoms, but the disease may later become active when immunity decreases, leading to the appearance of active tuberculosis that requires medical treatment.
How is tuberculosis usually treated?
The treatment of tuberculosis is mainly based on the use of special antibiotics taken for a long time, usually for several months, and includes both latent tuberculosis and active tuberculosis.
In cases of latent tuberculosis, treatment is given to prevent the infection from turning into an active disease, especially in people with weak immunity, while active tuberculosis requires taking a combination of several medications for up to six or nine months depending on the case, and full commitment to taking medications until the end of the treatment period is essential to eliminate the bacteria and prevent the emergence of drug-resistant strains, as stopping treatment early may lead to treatment failure and complicate the case.
When is drug treatment for TB not enough?
In most cases, drug treatment is effective in controlling tuberculosis, but this treatment may fail in some patients, especially in cases of drug-resistant tuberculosis or when the presence of bacteria in sputum persists despite full adherence to treatment.
Drug therapy may not be sufficient when advanced pulmonary complications occur, such as localized destruction of lung tissue, the formation of chronic cavities and abscesses, or persistent bronchiectasis. Severe pulmonary hemorrhage is one of the most serious complications of TB, and may require surgical intervention in some cases, especially when conservative or interventional therapies fail.
In such circumstances, surgical intervention becomes an important supportive option in addition to drug therapy, especially when the infection is localized and the affected part can be removed, improving the chances of recovery and reducing the risk of persistent or recurrent infection.
The role of surgery in tuberculosis treatment
Although drug therapy remains the mainstay of TB management, the role of surgery in tuberculosis treatment is emerging as an important supportive option in some complex cases. Surgery is not used as a substitute for drugs, but rather aims to enhance their effectiveness by removing localized disease foci that impede full response to treatment.
The essence of the role of surgery in tuberculosis treatment is to reduce the bacterial burden and improve the conditions that allow drug therapy to work more efficiently. Studies show that when patients are carefully selected, resection of the affected part of the lung, in conjunction with continued drug therapy, can achieve cure rates as high as 90%, resulting in disease control and improved quality of life.
Preparing for surgery in patients with tuberculosis
Good pre-surgical preparation is an essential step to ensure the success of surgical intervention and minimize risks in TB patients. This begins with a thorough assessment of the patient’s general health status, focusing on lung function to ensure that the body can withstand surgery and loss of lung tissue if resection is required. It also ensures that the infection is localized and can be managed surgically, and that drug therapy has been used appropriately before the decision to operate is made.
Doctors pay special attention to the patient’s nutritional status, as optimizing nutrition is an important factor in supporting post-operative recovery. In addition, the surgical intervention is planned as part of an integrated medical team to ensure infection control and continuation of post-operative drug therapy, increasing the chances of success and minimizing the occurrence of complications.
Types of surgeries used to treat tuberculosis
The types of surgical procedures used in the treatment of tuberculosis are determined based on the extent of the infection and the extent of damage to the lung tissue, taking into account the patient’s general condition and respiratory functions. These interventions aim to remove disease foci or treat localized complications, making drug therapy more effective and contributing to reducing disease activity and complications.
Partial lung resection
Partial lung resection is used when tuberculosis is localized and confined to a small area without extensive spread to the rest of the lung tissue. This procedure is one of the applications of the role of surgery in tuberculosis treatment, as it aims to remove an infected focus that is a persistent source of infection or prevents full recovery despite adherence to drug therapy. In appropriate cases, this type of resection can be performed either by traditional open surgery or by using video-assisted minimally invasive thoracic surgery (VATS) techniques, which allow the resection to be accomplished through small incisions with less pain and faster recovery, without affecting the therapeutic goal of the surgery.
Pulmonary lobectomy
Pulmonary lobectomy is one of the most common procedures in the treatment of locally advanced pulmonary tuberculosis, especially when there is extensive destruction of one of the lobes or chronic pulmonary cavities that do not respond to drug therapy, aiming to remove the source of chronic infection and minimize the risk of persistent symptoms or disease recurrence. In selected cases, pulmonary lobectomy can be performed using minimally invasive surgical techniques such as VATS, when the anatomical condition allows it, while maintaining the effectiveness of the surgery and minimizing the surgical burden on the patient.
Complete lung resection
Whole lung resection is a major surgical option and is only used in severe cases of extensive and irreversible lung damage. This decision is made after careful evaluation of the remaining lung function and the overall health status of the patient, given its significant impact on respiratory capacity. This procedure is one of the most complex forms of the role of surgery in tuberculosis treatment, but it may be necessary in selected cases when all other treatment options have failed.
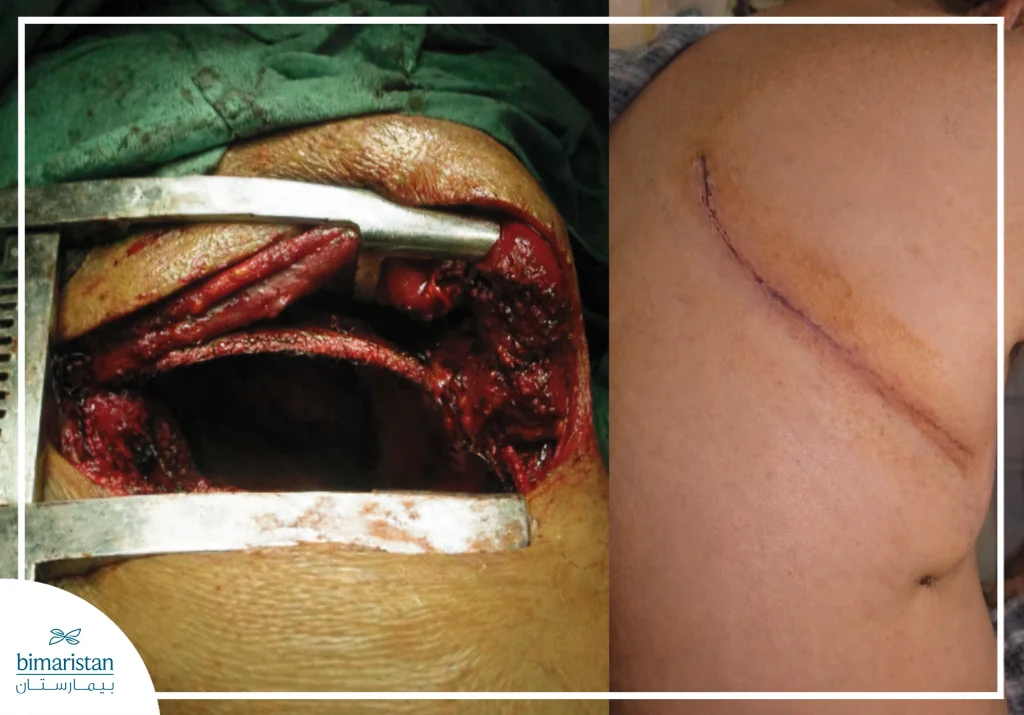
Surgery to treat complications of pulmonary tuberculosis
The role of surgery in tuberculosis treatment is not limited to removing parts of the lungs; it also includes procedures to treat complications resulting from the disease, such as chronic chest infections, fistulas, or persistent purulent collections. These interventions aim to improve the patient’s condition and reduce the risk of chronic infection, and are often performed in combination with long-term drug therapy to achieve the best results.
Post-surgery and the role of pharmacotherapy
The treatment plan does not end when the surgical intervention is performed. Continuing drug treatment after the operation is an essential part of the success of the role of surgery in tuberculosis treatment, as even after removing the infected tissues or treating localized complications, the TB bacteria may remain in the body, requiring follow-up antibiotic treatment according to recommended medical protocols to prevent recurrence of the disease or the development of drug resistance.
Studies show that the integration of surgery and drug therapy significantly improves treatment outcomes, especially when the postoperative treatment period is fully adhered to. The post-operative phase also includes regular medical follow-up to assess recovery, monitor lung function, and detect potential complications early. This integration strengthens the role of surgery in tuberculosis treatment as part of a comprehensive treatment plan aimed at achieving better recovery and minimizing the risk of relapse in the long term.
Potential risks of tuberculosis surgery
Although the role of surgery in tuberculosis treatment may be crucial in selected cases, this treatment option requires a clear understanding of the potential risks, as lung surgery is a major intervention that needs careful evaluation before making a decision. The main risks associated with surgery include the following:
- Risks associated with general anesthesia, especially in patients with poor general health
- Bleeding or infections after surgery, as with any major surgery
- Temporary respiratory issues or reduced respiratory capacity, especially when a large portion of the lung is removed
- Increased risk of complications in patients with malnutrition or chronic comorbidities
For these reasons, the decision to operate is made after careful weighing of the expected benefit of surgery in treating TB against the potential risks, ensuring that the right patients are selected and that careful medical follow-up is provided before and after surgery to minimize these risks as much as possible.
In conclusion, surgery is a complementary treatment option in the treatment of TB and is resorted to in cases where drug therapy alone is not sufficient to control the disease or when complications arise that require surgical intervention. The integration of surgery with drug therapy and regular medical follow-up contributes to improving treatment outcomes and reducing the risk of relapse, especially when patients are carefully selected. With advances in surgical techniques and medical care, surgery has become safer and more effective when incorporated into an integrated treatment plan.
Sources:
- Shiraishi, Y. (2017). Surgical treatment of pulmonary tuberculosis. Microbiology Spectrum, 5(1), TNMI7-0043-2017.
- Surgery for pulmonary tuberculosis. (n.d.). SlideShare.

