شهد علاج سرطان المستقيم تطورًا كبيرًا خلال السنوات الأخيرة، مع ظهور تقنيات حديثة تهدف إلى زيادة فرص الشفاء وتقليل المضاعفات، مع الحفاظ على جودة حياة المريض. لم يعد العلاج مقتصرًا على الجراحة التقليدية فقط، بل أصبح يشمل مجموعة من الأساليب المتقدمة، مثل الجراحة بالمنظار، الجراحة الروبوتية، استئصال المستقيم عبر الشرج (TaTME)، والعلاج الإشعاعي والكيميائي الحديث.
تساعد هذه الطرق الحديثة على استئصال الورم بدقة عالية، تقليل الألم، تقصير فترة التعافي، والحفاظ على وظائف المستقيم الطبيعية قدر الإمكان. في تركيا، تتوفر هذه التقنيات في مراكز متخصصة، بإشراف جراحين ذوي خبرة كبيرة، مما يجعلها وجهة مفضلة للمرضى الباحثين عن علاج متقدم وآمن.
ما هو سرطان المستقيم؟
سرطان المستقيم هو نوع من السرطان ينشأ في الخلايا المبطنة للمستقيم، وهو الجزء الأخير من الأمعاء الغليظة الذي يربط القولون بفتحة الشرج. يبدأ المرض عادةً على شكل سلائل (Polyps) تتحول مع الوقت إلى أورام سرطانية إذا لم تُكتشف وتُعالج مبكرًا.
يختلف سرطان المستقيم عن سرطان القولون من حيث الموقع وطريقة العلاج، إذ يتطلب في كثير من الحالات تقنيات جراحية دقيقة بسبب قربه من العضلة العاصرة والأعصاب المسؤولة عن التحكم في عملية الإخراج. لذلك، يعتمد علاج سرطان المستقيم على مرحلة المرض وموقع الورم، وقد يشمل الجراحة، والعلاج الإشعاعي، والعلاج الكيميائي، أو مزيجًا منها.
الفرق بين سرطان المستقيم وسرطان القولون
رغم تصنيف سرطان القولون والمستقيم ضمن أورام القولون والمستقيم، إلا أن هناك فروقاً مهمة تؤثر على التشخيص وخيارات العلاج:
| جانب المقارنة | سرطان القولون | سرطان المستقيم |
|---|---|---|
| الموقع | الأجزاء العليا من الأمعاء الغليظة | الجزء الأخير من الأمعاء الغليظة بالقرب من فتحة الشرج |
| القرب من العضلة العاصرة | بعيد نسبياً | قريب جداً، مما يجعل الجراحة أكثر تحدياً |
| طرق العلاج | غالبًا جراحة فقط | جراحة دقيقة وعلاج إشعاعي وكيميائي حسب المرحلة |
| صعوبة الجراحة | أقل | أعلى بسبب ضيق الحوض والحاجة للحفاظ على العضلة العاصرة |
| الحفاظ على وظيفة الإخراج | أسهل | يحتاج تقنيات حديثة للحفاظ على العضلة العاصرة، مثل TaTME أو الروبوت |
هذه المقارنة تساعد المرضى على فهم السبب وراء اختلاف خيارات العلاج وأهمية التقنيات الحديثة لعلاج سرطان المستقيم بشكل آمن وفعال.
الفئات الأكثر عرضة للإصابة بسرطان المستقيم
- الأشخاص فوق سن 50 عامًا
- من لديهم زوائد لحمية في القولون أو المستقيم
- من لديهم تاريخ عائلي لسرطان القولون أو المستقيم
- المصابون بأمراض الأمعاء الالتهابية المزمنة (مثل التهاب القولون التقرحي)
- الأشخاص الذين يتبعون نظامًا غذائيًا غنيًا باللحوم المصنعة وقليل الألياف
- قلة النشاط البدني والسمنة
- المدخنون
مراحل سرطان المستقيم
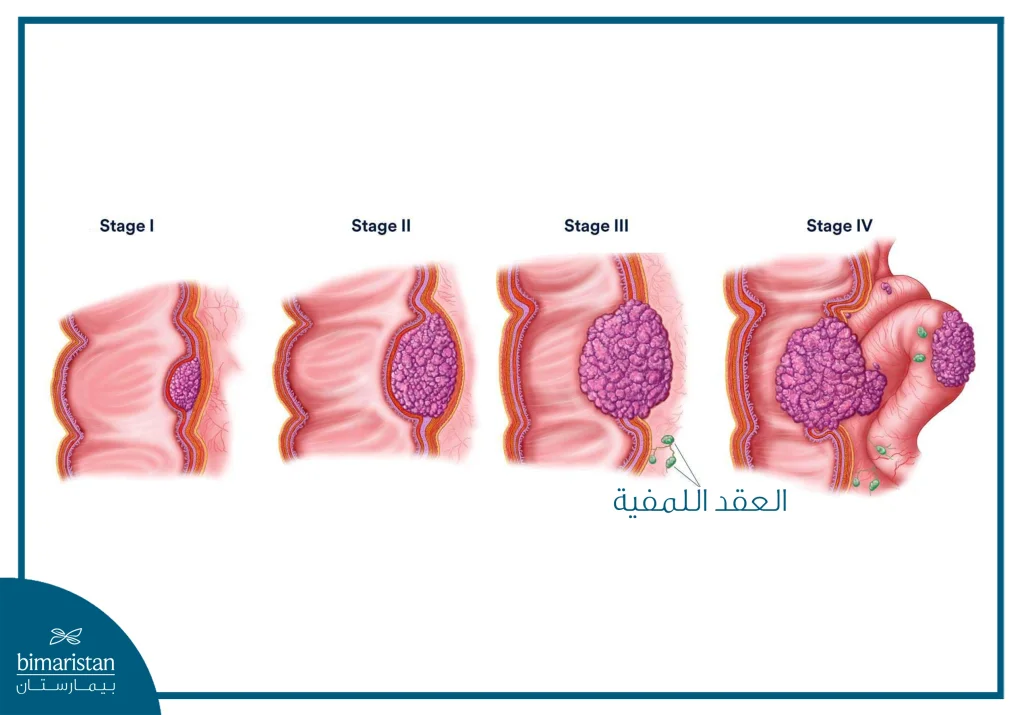
الموقع يوضح أن مرحلة السرطان تُحدَّد وفقًا لنظام TNM الذي يأخذ بالاعتبار حجم الورم، انتشار السرطان في العقد الليمفاوية، وانتشاره إلى أجزاء بعيدة من الجسم. المراحل الرئيسية هي:
- المرحلة 0 (Carcinoma in situ): تكون الخلايا غير الطبيعية موجودة فقط في الطبقة الداخلية لجدار المستقيم ولا تمتد للخارج. تُسمى أحيانًا سرطان موضعي (لابدة).
- المرحلة I: السرطان امتدّ من الطبقة الداخلية إلى الأنسجة المجاورة (مثل الطبقة تحت المخاط أو عضلات جدار المستقيم) لكن لم ينتشر إلى العقد الليمفاوية أو الأعضاء البعيدة.
- المرحلة II تشمل ثلاث مجموعات فرعية:
- IIA: السرطان امتدّ عبر العضلة إلى الطبقة الخارجية من جدار المستقيم (serosa).
- IIB: السرطان امتدّ عبر الطبقة الخارجية ولكن لم يصل لأعضاء قريبة.
- IIC: السرطان امتدّ إلى أعضاء قريبة من المستقيم.
- المرحلة III تشمل ثلاث مجموعات فرعية:
- السرطان امتدّ إلى واحد أو أكثر من العقد الليمفاوية القريبة، وقد يكون امتدّ في جدار المستقيم بعمق أكبر.
- ينقسم إلى IIIA وIIIB وIIIC حسب عدد العقد الليمفاوية ومدى انتشار الورم.
- المرحلة IV سرطان منتشِر: السرطان انتشر إلى أجزاء بعيدة من الجسم مثل الكبد أو الرئتين أو العقد الليمفاوية البعيدة. تنقسم أيضًا إلى IV A, IV B, IV C بحسب عدد المواقع التي انتشر إليها السرطان.
- السرطان العائد: قد يعود السرطان بعد العلاج في نفس مكانه أو في جزء آخر من الجسم، وهذه الحالة تحتاج تقييمًا علاجياً جديدًا.
أعراض سرطان المستقيم
تختلف أعراض سرطان المستقيم حسب مرحلة المرض وموقع الورم، وقد تكون خفيفة أو غير واضحة في المراحل المبكرة، مما يجعل الكشف المبكر أمراً بالغ الأهمية.
الأعراض المبكرة
- نزيف من الشرج أو وجود دم في البراز
- تغيّر في نمط التبرز (إسهال أو إمساك مستمر)
- الإحساس بعدم إفراغ المستقيم بالكامل
- براز رفيع أو متغير الشكل
الأعراض المتقدمة
- ألم أو ضغط في منطقة الحوض أو المستقيم
- فقر الدم الناتج عن النزيف المزمن
- إرهاق عام وضعف مستمر
- فقدان الوزن غير المبرر

تشخيص سرطان المستقيم
يعد التشخيص المبكر لسرطان المستقيم أمرًا بالغ الأهمية لزيادة فرص العلاج الناجح والحفاظ على جودة حياة المريض. يعتمد التشخيص على مجموعة من الفحوصات السريرية والصور الطبية الدقيقة لتحديد مرحلة الورم وموقعه. ويكون التشخيص وفق ما يلي:
- الفحوصات السريرية:
- الفحص الشرجي الرقمي: يسمح للطبيب بالكشف عن أي أورام أو زوائد غير طبيعية في المستقيم.
- التاريخ المرضي والفحص السريري العام: لتقييم الأعراض والمخاطر المرتبطة بسرطان المستقيم.
- الفحص الشعاعي:
- التصوير بالرنين المغناطيسي (MRI): لتحديد مدى انتشار الورم في جدار المستقيم والأنسجة المحيطة.
- الأشعة المقطعية (CT Scan): لتقييم انتقال السرطان إلى أعضاء أخرى مثل الكبد أو الرئة.
- الموجات فوق الصوتية عبر المستقيم : لتقدير عمق انتشار الورم في جدار المستقيم والعقد اللمفاوية القريبة.
- الفحوصات المخبرية:
- خزعة: أخذ عينة من الورم لتحليلها مجهريًا وتأكيد التشخيص.
- اختبارات الدم: مثل فحص مؤشرات الورم (Tumor Markers) لدعم تقييم المرض.
- تحديد مرحلة المرض: تصنيف السرطان حسب المرحلة يساعد الطبيب في اختيار العلاج الأنسب، سواء كانت الجراحة التقليدية، الجراحة الحديثة بالمنظار أو الروبوت، أو الجمع مع العلاج الإشعاعي والكيميائي.
علاج سرطان المستقيم حسب المرحلة
يعتمد علاج سرطان المستقيم بشكل أساسي على مرحلة المرض، ومدى انتشار الورم، وموقعه داخل المستقيم، مع الهدف الأساسي المتمثل في إزالة السرطان بالكامل مع الحفاظ على وظيفة الإخراج وجودة حياة المريض قدر الإمكان.
علاج سرطان المستقيم (Stage 0)
في هذه المرحلة يكون السرطان محصورًا في الطبقة الداخلية من بطانة المستقيم فقط. غالبًا ما يتم العلاج عبر جراحة طفيفة التوغل. كما يمكن إزالة الورم بالكامل دون الحاجة إلى علاج إضافي مثل العلاج الكيميائي أو الإشعاعي، إن نسب الشفاء في هذه المرحلة مرتفعة جدًا.
علاج سرطان المستقيم (Stage I)
في علاج سرطان المستقيم في المرحلة الأولى (Stage I) يكون الورم قد اخترق جدار المستقيم لكنه لا يزال موضعيًا ولم ينتشر إلى الأنسجة المحيطة أو العقد اللمفاوية. في هذه المرحلة تُعد الجراحة هي العلاج الأساسي، ويحرص الجراحون قدر الإمكان على تجنب الجراحة البطنية الواسعة، خاصة عندما يكون الورم منخفضًا، وذلك بالاعتماد على التقنيات الجراحية الحديثة طفيفة التوغل.
في كثير من الحالات، يمكن إزالة الأورام الصغيرة والمبكرة في الجزء السفلي من المستقيم من خلال الاستئصال الموضعي عبر الشرج، وهي تقنية تسمح باستئصال الورم مباشرة عبر فتحة الشرج دون الحاجة إلى شقوق بطنية. أما الأورام الأكبر حجمًا أو الأعلى موقعًا داخل المستقيم، فيمكن علاجها باستخدام الجراحة التنظيرية عبر الشرج، حيث تُستخدم أدوات خاصة ومنظار لتوفير رؤية أدق وتمكين استئصال الورم بشكل آمن.
في حال تعذر إزالة الورم عبر الشرج، قد يكون من الضروري اللجوء إلى جراحات أكثر توسعًا تعتمد على موقع الورم داخل المستقيم. ففي الأورام الموجودة في الجزء العلوي من المستقيم، يُستخدم الاستئصال الأمامي، حيث يتم إزالة الجزء المصاب من المستقيم ثم إعادة توصيل القولون بالجزء المتبقي. أما الأورام في منتصف أو أسفل المستقيم، فيُجرى الاستئصال الأمامي المنخفض، مع توصيل القولون مباشرة بالشرج للحفاظ على وظيفة الإخراج قدر الإمكان.
وفي الحالات التي يكون فيها الورم منخفضًا جدًا وقريبًا من العضلة العاصرة، قد يلزم إجراء الاستئصال البطني العجاني (APR)، والذي يتطلب إزالة المستقيم والشرج مع الحاجة إلى كيس دائم. في جميع هذه الخيارات، يتم تقييم كل حالة بشكل فردي، مع إعطاء أولوية قصوى للحفاظ على العضلة العاصرة وتجنب الكيس الدائم متى كان ذلك ممكنًا، دون التأثير على فعالية العلاج أو فرص الشفاء.
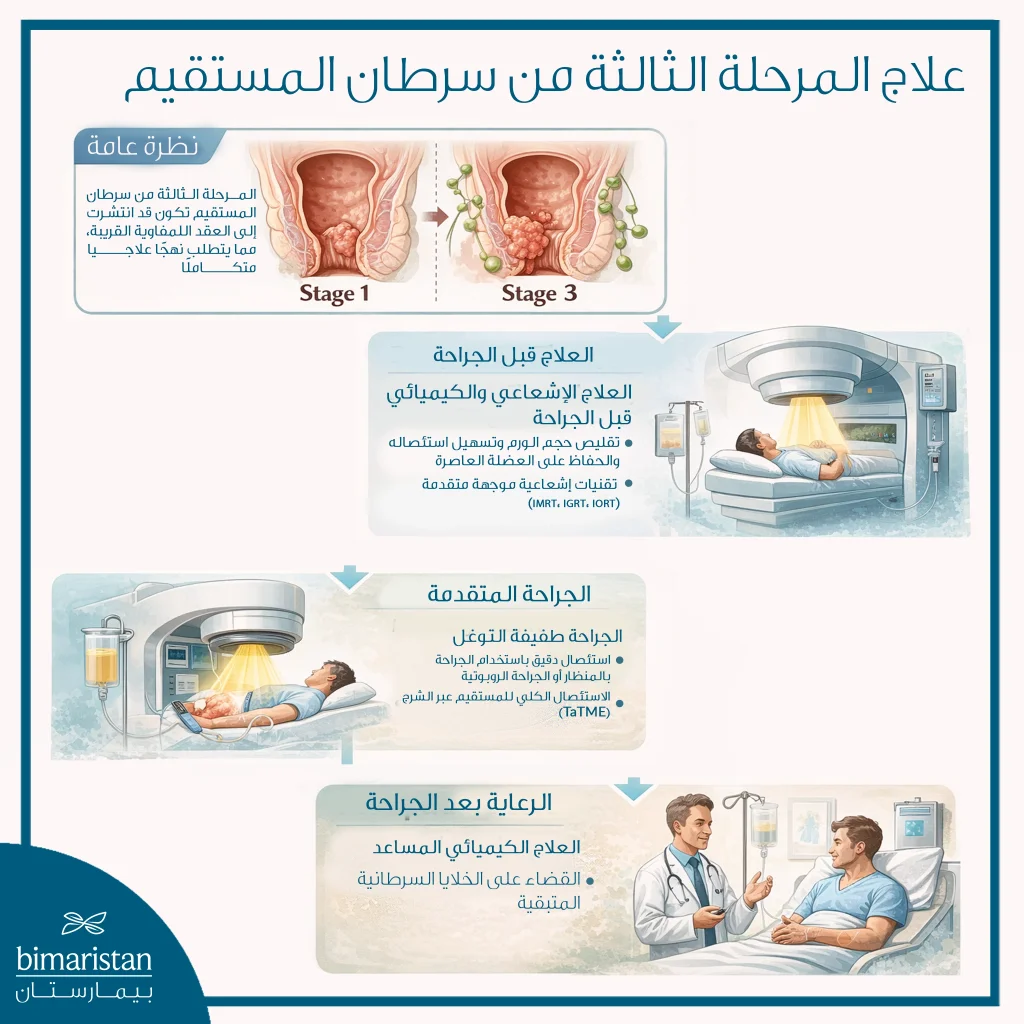
علاج سرطان المستقيم (Stage II & III)
يُعتمد في علاج سرطان المستقيم في المرحلتين الثانية والثالثة على العلاج المدمج بوصفه النهج الأكثر فعالية لتحقيق السيطرة على المرض وتقليل خطر عودته. ففي المرحلة الثانية يكون الورم قد تجاوز جدار المستقيم دون إصابة العقد اللمفاوية، بينما تتميز المرحلة الثالثة بانتشار الخلايا السرطانية إلى العقد اللمفاوية القريبة، ما يستدعي خطة علاجية متكاملة.
غالبًا ما يبدأ العلاج بالعلاج الإشعاعي المترافق مع العلاج الكيميائي قبل الجراحة بهدف تقليص حجم الورم وتسهيل استئصاله، إضافة إلى زيادة فرص الحفاظ على العضلة العاصرة وتقليل الحاجة إلى الكيس الدائم. يُعطى العلاج الإشعاعي إما على شكل جرعات صغيرة يومية تمتد لمدة خمسة إلى ستة أسابيع، أو على شكل جرعات مكثفة خلال فترة قصيرة لا تتجاوز خمسة أيام، ويتم اختيار الخطة الأنسب بناءً على موقع الورم وقربه من الشرج وحالة المريض العامة.
وتشمل تقنيات الإشعاع الحديثة الإشعاع الخارجي الموجّه بدقة مثل IMRT وIGRT، والعلاج الإشعاعي الموضعي، إضافة إلى العلاج الإشعاعي أثناء الجراحة (IORT) في الحالات المعقدة أو عند عودة الورم. بعد الانتهاء من العلاج التحضيري، يتم إجراء جراحة حديثة دقيقة باستخدام إحدى التقنيات المتقدمة مثل الجراحة بالمنظار، الجراحة الروبوتية، أو التقنيات الجراحية عبر الشرج، وفقًا لموضع الورم وتشريحه. ويُعد الاستئصال الكلي للمستقيم عبر الشرج (TaTME) من أبرز هذه التقنيات الحديثة، حيث يُستخدم بشكل أساسي في المرحلتين الثانية والثالثة، خاصة في الأورام المنخفضة والقريبة من العضلة العاصرة.
تُجرى هذه الجراحة عبر الشرج دون الحاجة إلى شقوق بطنية واسعة، ما يوفر رؤية دقيقة للورم ويسمح باستئصال كامل للغشاء المساريقي للمستقيم مع الحفاظ على الأعصاب والعضلة العاصرة قدر الإمكان، الأمر الذي يساهم في تحسين النتائج الوظيفية بعد الجراحة وتقليل الحاجة إلى الكيس الدائم. وبعد الجراحة، يُستكمل العلاج بالعلاج الكيميائي التكميلي لمدة تتراوح بين خمسة وستة أشهر، بهدف القضاء على أي خلايا سرطانية متبقية وتقليل خطر عودة المرض على المدى الطويل.
علاج سرطان المستقيم في المرحلة الرابعة (Stage IV)
في علاج سرطان المستقيم في المرحلة الرابعة (Stage IV) يكون المرض قد انتشر خارج المستقيم إلى أعضاء بعيدة مثل الكبد أو الرئتين، ما يجعل الخطة العلاجية أكثر تعقيدًا ومرتكزة على السيطرة على انتشار السرطان وتحسين جودة حياة المريض. في هذه المرحلة يُعد العلاج الكيميائي هو الخط الأول للعلاج، حيث يهدف إلى تقليص حجم الأورام والحد من انتشار الخلايا السرطانية في الجسم.
تشمل بروتوكولات العلاج الكيميائي أدوية معروفة مثل Fluorouracil (5-FU) وOxaliplatin وCapecitabine وIrinotecan، وغالبًا ما يتم دمجها مع العلاجات الموجهة مثل Bevacizumab أو Cetuximab وفق الخصائص الجزيئية للورم وحالة المريض. يساعد هذا النهج العلاجي المتكامل على تحسين الاستجابة للعلاج وإطالة فترة السيطرة على المرض.
في حالات مختارة، يمكن اللجوء إلى الجراحة أو العلاج الإشعاعي لإزالة الورم الأساسي في المستقيم أو بعض النقائل، خاصة عندما يكون انتشار المرض محدودًا وقابلًا للاستئصال، وذلك بهدف تحسين الأعراض أو إطالة البقاء. أما في الحالات التي لا تكون فيها الجراحة ممكنة، فيتركز العلاج على التخفيف من الأعراض وتحسين جودة الحياة من خلال السيطرة على الألم، النزيف، أو انسداد الأمعاء، مع متابعة طبية دقيقة ومستمرة.
الفغرة (الكيس) بعد علاج سرطان المستقيم
- فغرة مؤقتة: تُستخدم للسماح بالتئام الأمعاء بعد الجراحة. غالبا يستخدم فغر اللفائفي (Ileostomy).
- فغرة دائمة: غالباً ما يستخدم فغر القولون (Colostomy) في هذه الحالة. تكون ضرورية في حال إزالة الشرج والعضلة العاصرة.
يتم تحديد نوع الفغرة (مؤقتة أو دائمة) حسب نوع الجراحة ومكان الورم.
علاج سرطان المستقيم في تركيا ونسب الشفاء وجودة الحياة بعد العلاج
أصبحت تركيا من الوجهات الرائدة في علاج سرطان المستقيم بفضل توفر جميع التقنيات الطبية الحديثة في مراكز متقدمة ومتخصصة في جراحة وأورام الجهاز الهضمي. تعتمد هذه المراكز على أحدث الأساليب العلاجية، بما في ذلك الجراحة بالمنظار، الجراحة الروبوتية، التقنيات الجراحية عبر الشرج، إضافة إلى العلاج الإشعاعي والكيميائي المتقدم، ويتم اختيار الخطة العلاجية لكل مريض بشكل فردي وفق مرحلة المرض وموقع الورم.
تلعب خبرة الجراحين دورًا محوريًا في نجاح العلاج، إذ تسهم الدقة الجراحية واختيار التقنية المناسبة في تحقيق نسب شفاء مرتفعة وتقليل المضاعفات، خاصة في الأورام المنخفضة أو القريبة من العضلة العاصرة. وقد أثبتت الدراسات أن استخدام التقنيات الحديثة يؤثر بشكل مباشر على النتائج طويلة الأمد، حيث يساعد على تقليل خطر الانتكاس الموضعي والحفاظ على الوظائف الحيوية للمستقيم.
أما الحياة بعد العلاج الحديث لسرطان المستقيم، فهي تشهد تحسنًا ملحوظًا مقارنة بالجراحة التقليدية، إذ يتيح التعافي السريع والعودة التدريجية للوظيفة الطبيعية للمستقيم للمريض استعادة نمط حياته اليومي بشكل أفضل. كما تُعد المتابعة طويلة الأمد جزءًا أساسيًا من الخطة العلاجية، حيث تشمل فحوصات دورية لمراقبة الشفاء والكشف المبكر عن أي عودة محتملة للمرض، مما يعزز فرص الاستمرار في حياة صحية وآمنة.
أخيراً، في ظل التطور الكبير في علاج سرطان المستقيم، لم يعد التشخيص يعني بالضرورة فقدان جودة الحياة أو الاعتماد على الجراحة التقليدية. فقد أتاحت التقنيات الحديثة، إلى جانب الخبرة الطبية المتقدمة، خيارات علاجية دقيقة تُحقق نسب شفاء مرتفعة وتقلل من المضاعفات والانتكاس، مع الحفاظ على الوظائف الطبيعية للمستقيم قدر الإمكان.
في تركيا، يجتمع توفر هذه التقنيات مع خبرة جراحين متخصصين ضمن مراكز متقدمة، ما يمنح المرضى فرصة حقيقية للحصول على علاج فعّال وآمن مبني على تقييم فردي دقيق لكل حالة. إن اتخاذ القرار العلاجي الصحيح، في الوقت المناسب، يشكل خطوة أساسية نحو الشفاء والعودة إلى حياة طبيعية مستقرة.
المصادر:
- National Cancer Institute. (2025, May 16). Rectal cancer treatment (PDQ®)–Patient version. U.S. Department of Health and Human Service
- Johns Hopkins Medicine. (n.d.). Rectal cancer treatment. Johns Hopkins Medicine
- Cancer Research UK. (2025, January 17). Treatment for bowel (rectal) cancer
- American Cancer Society. (2024, February 5). Rectal cancer treatment, by stage