Bilateral salpingo-oophorectomy is a surgical procedure performed as part of female reproductive system surgery and is used in specific disease states or as a preventive measure in some women at high risk of ovarian cancer.
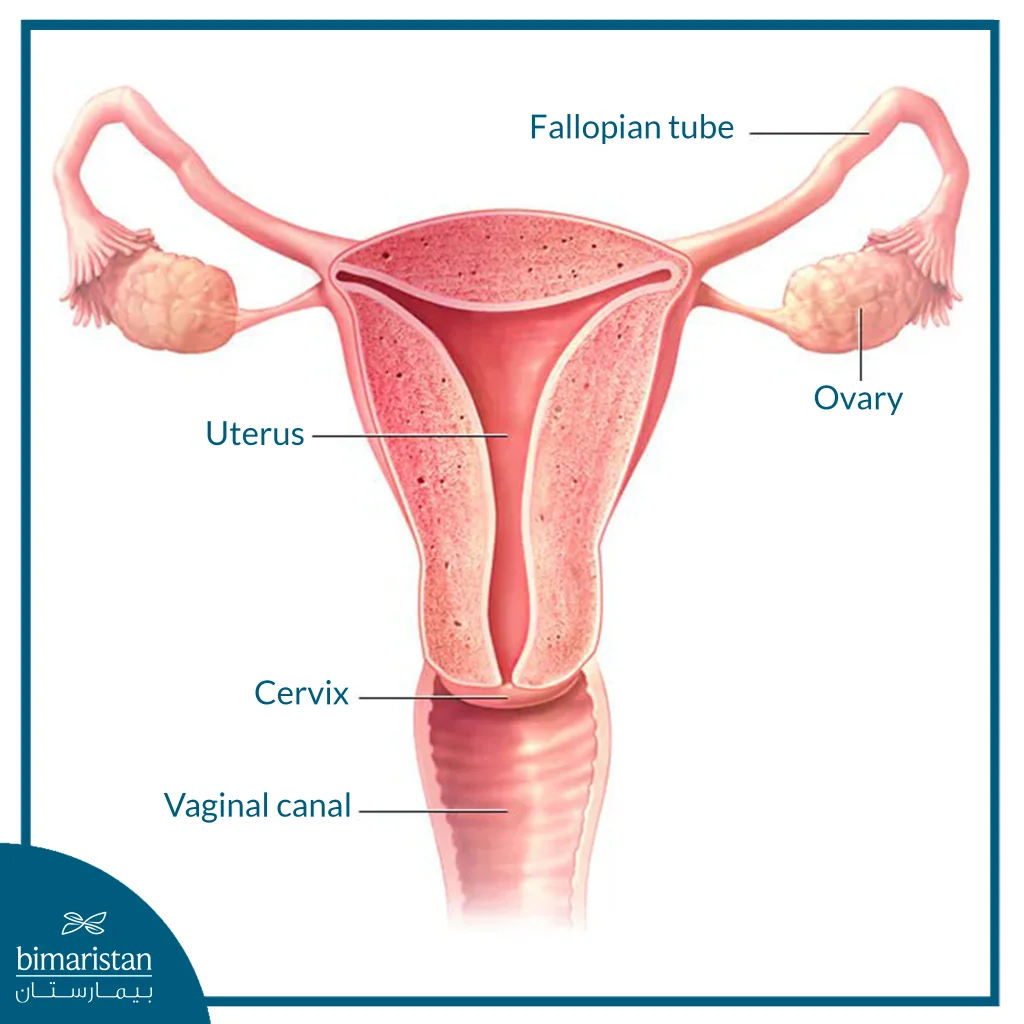
The female reproductive system includes the ovaries, fallopian tubes, uterus, cervix and vagina and is located in the lower abdomen, where the uterus is between the bladder and rectum, while the fallopian tubes and ovaries are connected to the uterus. The decision to perform this surgery is made after careful medical evaluation and a detailed discussion between the patient and the medical team about its causes and possible effects.
What is bilateral salpingo-oophorectomy?
Bilateral salpingo-oophorectomy is a surgical procedure in which both fallopian tubes and both ovaries are removed. This type of surgery is performed in several contexts, including ovarian cancer treatment, prevention in high-risk women, or as an elective procedure during hysterectomy for benign reasons. It may also be performed in cases where the ovaries or fallopian tubes cannot be preserved, such as ovarian masses that do not contain viable tissue, or severe infections that do not respond to treatment.
After a bilateral salpingo-oophorectomy, the menstrual cycle is permanently stopped and the woman is unable to have children. Menopausal symptoms such as hot flashes, night sweats, and vaginal dryness may occur whether the surgery is performed before or after menopause.
When is bilateral salpingo-oophorectomy recommended?
Bilateral salpingo-oophorectomy is recommended for specific conditions or as a preventative measure, after evaluating the patient’s health status and medical reasons for surgery. Conditions in which this procedure may be recommended include the following:
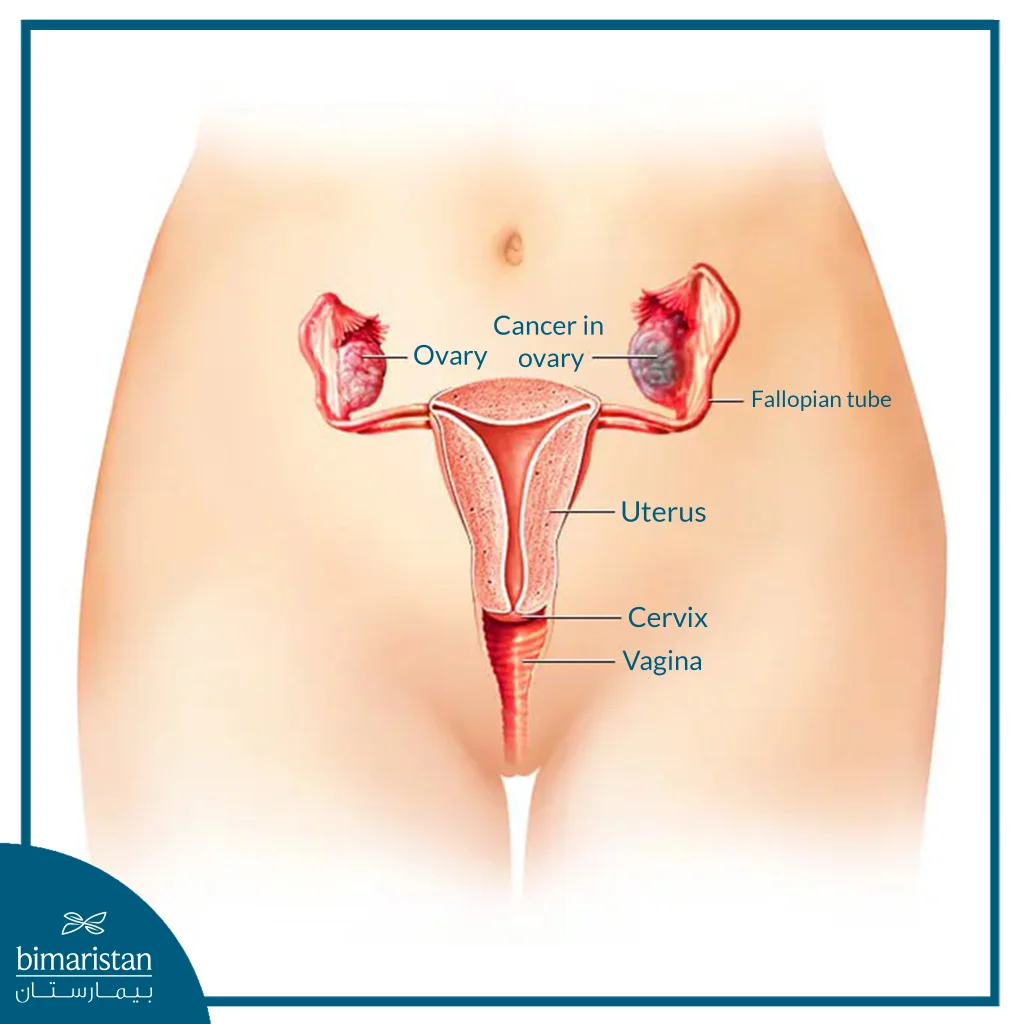
- Having uterine or ovarian cancer or having cancerous metastases to the ovaries from primary tumors in other organs
- Endometriosis in cases where the ovaries or fallopian tubes cannot be preserved
- Severe pelvic infections, including a tubo-ovarian abscess that is unresponsive to treatment
- Presence of tumors or benign ovarian cysts that do not contain healthy tissue that can be preserved
- Adnexal torsion, when it leads to ovarian or fallopian tube damage
- Ectopic pregnancy in cases where the fallopian tubes or ovaries cannot be preserved
- Reducing the risk of ovarian or breast cancer in women with genetically high risk
- An elective procedure during other surgeries, such as a hysterectomy for benign reasons, to minimize the risk of developing future ovarian disease
Bilateral salpingo-oophorectomy for cancer prevention
Bilateral salpingo-oophorectomy may be used as a preventative measure in women with a high risk of ovarian cancer and, in some cases, to reduce the risk of breast cancer. This procedure is especially recommended for women with a genetic predisposition to ovarian cancer, where the ovaries and fallopian tubes are removed to minimize the likelihood of future cancer development.
The decision to perform this type of prophylactic resection is made after careful evaluation of risk factors and discussion of the benefits and potential complications with the medical team.
Bilateral salpingo-oophorectomy procedure methods
Bilateral salpingo-oophorectomy is performed by one of three main surgical methods, and the execution varies depending on the technique used, with the primary goal being the complete and safe removal of the ovaries and fallopian tubes. Each method is explained in more detail below:
Bilateral salpingo-oophorectomy with open surgery
In open surgery, the patient is taken to the operating room and the procedure is performed under general anesthesia. The surgeon begins by making an incision in the abdominal wall, which may be transverse or vertical depending on the reason for the surgery, the patient’s body structure, and the surgeon’s discretion. After opening the abdomen, the pelvic and abdominal cavity is carefully explored, where the genitals and neighboring organs are examined for any abnormal changes.
Next, the ligaments holding the ovaries and fallopian tubes are identified and these structures are surgically separated and the ovaries and fallopian tubes are removed. After removal, the surgical area is re-examined to make sure the bleeding is under control, and the incision is closed after confirming the integrity of the tissues.
Laparoscopic bilateral salpingo-oophorectomy
Laparoscopic surgery is a technique that uses small surgical incisions instead of a large abdominal incision. After the patient is anesthetized, the surgeon makes a small incision in the abdomen that is used to insert a special needle, and then the abdominal cavity is inflated with carbon dioxide gas to create a space that allows the organs to be seen clearly.
Next, several other small incisions are made through which a long, thin surgical camera and precision surgical instruments are inserted. The camera transmits a live image of the internal organs, allowing the surgeon to precisely locate the ovaries and fallopian tubes. The ovaries and fallopian tubes are separated using surgical instruments and then removed through one of the small incisions. If the size of the organs does not allow them to exit through the opening, one of the incisions may be slightly enlarged to complete the removal.
Laparoscopic Robotic Surgery
Laparoscopic-assisted robotic surgery is similar to laparoscopic surgery in terms of the number of small incisions, carbon dioxide insufflation of the abdomen, and the use of a surgical camera. The main difference lies in the method of controlling the surgical instruments, as the surgeon uses a robotic system to control the camera and instruments instead of direct manual control.
The robotic system executes the surgeon’s movements within the abdominal cavity, helping to guide the instruments as they identify and separate the ovaries and fallopian tubes, then remove them through the same small incisions used in laparoscopic surgery.
Preparation before bilateral salpingo-oophorectomy
Preparation for bilateral salpingo-oophorectomy begins well in advance of the surgery, as the medical team works with the patient to ensure she is fully prepared for the procedure. This includes reviewing medical and surgical history, and informing the health team of all medications and supplements taken, both prescription and over-the-counter.
Preoperative tests such as blood tests, ECG, and chest x-rays may be ordered to assess overall health and safely plan for anesthesia. You will also be given clear instructions about stopping certain medications or supplements that may increase the risk of bleeding, as well as instructions about fasting before surgery.
It is also advisable to quit smoking and minimize alcohol consumption before the procedure, and inform the medical team of any special health conditions such as sleep apnea or allergies to certain medications or substances.
What happens during bilateral salpingo-oophorectomy?
What happens during a bilateral salpingo-oophorectomy depends on the type of surgery used. The procedure is usually performed under general anesthesia, so the patient does not feel any pain during the procedure. In open surgery, the surgeon makes an incision in the abdomen to access and remove the ovaries and fallopian tubes.
In laparoscopic or laparoscopic-assisted robotic surgery, several small incisions are made in the abdomen, through which a surgical camera and precision instruments are inserted after the abdomen is inflated with carbon dioxide gas to provide a sufficient viewing area. The camera helps the surgeon see the reproductive organs clearly, and the ovaries and fallopian tubes are removed through these small openings.
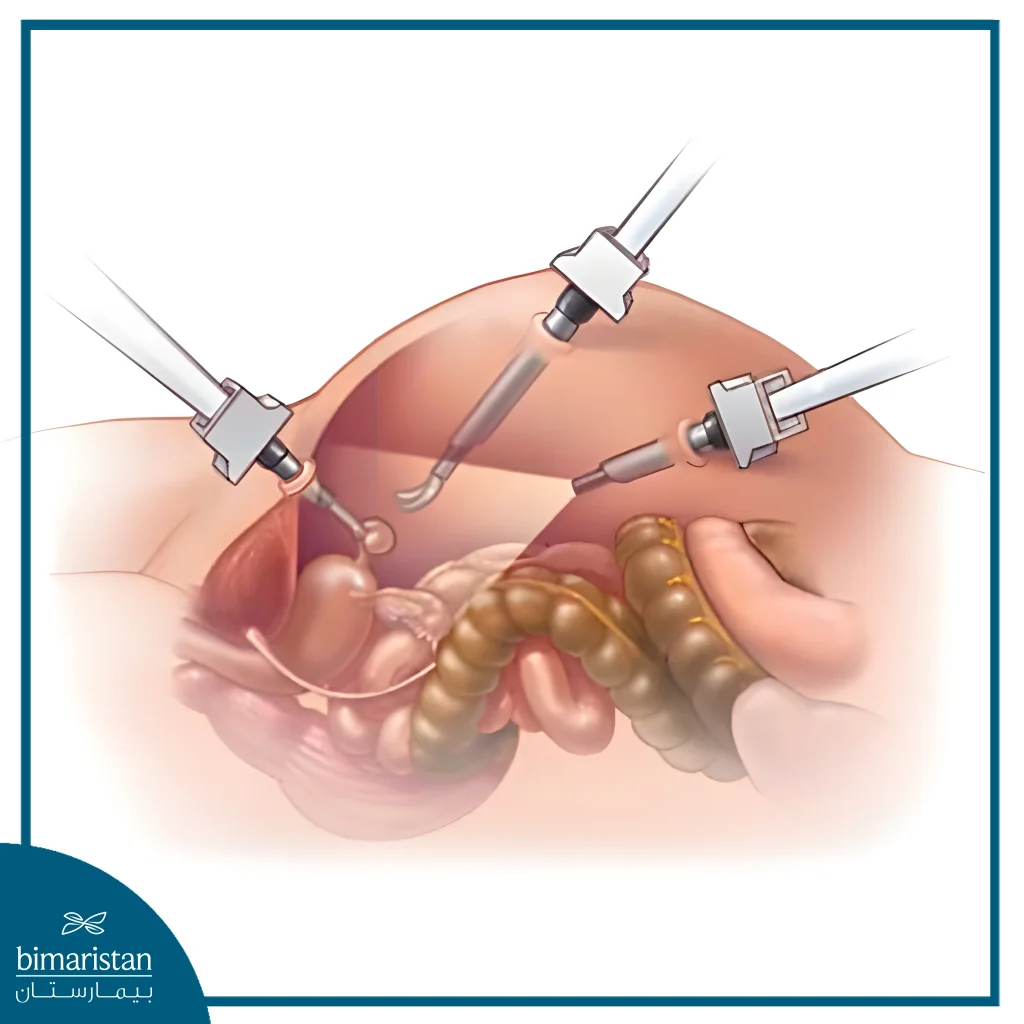
After the surgery is completed, the incisions are closed using sutures, staples or surgical adhesives, and may be covered with appropriate bandages.
Recovery after bilateral salpingo-oophorectomy
The recovery period after bilateral salpingo-oophorectomy varies depending on the type of surgery. In laparoscopic or robotic surgery, many patients can go home the same day or after a short hospital stay, and the recovery and gradual return to normal activity may take a few weeks. In the case of open surgery, the patient usually needs to stay in the hospital for several days, and the recovery is longer and may extend to several weeks before full activity is restored.
During the recovery period, patients receive detailed instructions including wound care, taking prescribed medications to prevent infection and relieve pain, permissible activity level, and follow-up appointments. Early light walking is recommended to minimize the risk of clots forming, and avoid heavy lifting or strenuous exercise for a set period of time.
Menopause-related symptoms such as hot flashes, night sweats, or vaginal dryness may also occur, and it is advisable to discuss these symptoms with your doctor for proper guidance.
Side effects and possible complications of bilateral salpingo-oophorectomy
Bilateral salpingo-oophorectomy has a number of potential side effects and complications, which vary in severity and occurrence from patient to patient. These complications include the following:
- Permanent loss of reproductive capacity as a result of removal of the ovaries and fallopian tubes
- Involvement of neighboring organs, such as the intestines, bladder or ureters
- Bleeding or vascular injury during surgery
- Intestinal obstruction
- Ovarian remnant syndrome
- Hernia at the incision site
- Formation of scar tissue or internal adhesions
If surgery is performed in premenopausal women, symptoms associated with menopause may occur, such as:
- Hot flashes
- Night sweats
- Vaginal dryness
- Difficulty falling asleep
- Anxiety or depression
Difference between bilateral salpingo-oophorectomy and hysterectomy
| Comparison | Bilateral salpingo-oophorectomy | Hysterectomy |
|---|---|---|
| Excised organs | Removal of the ovaries and fallopian tubes with the uterus remaining | Only the uterus is removed, and the ovaries may remain intact |
| Hormonal influence | The removal of the ovaries stops the production of female hormones, and menopausal symptoms may appear | Hormonal change does not necessarily occur if the ovaries are not removed |
| Impact on fertility | Loss of reproductive capacity due to the absence of ovaries and eggs | Loss of the ability to conceive due to removal of the uterus, even if the ovaries continue to function |
Medical follow-up after bilateral salpingo-oophorectomy
Regular medical follow-up after bilateral salpingo-oophorectomy is an essential step to ensure proper recovery and monitor short- and long-term health. Follow-up usually includes the following:
- Monitor hormonal changes and associated symptoms, such as hot flashes or sleep disturbances
- Monitor for any abnormal symptoms or possible complications after surgery and deal with them early
- See your doctor at scheduled appointments to assess your overall recovery and ensure wound healing
- Reviewing prescribed medications and adjusting them as needed as the condition progresses
- Discuss any questions related to general health or quality of life after surgery
- Provide guidance on physical activity and a gradual return to daily life
In conclusion, bilateral salpingo-oophorectomy is an important surgical procedure used to treat specific conditions or for prevention in some women at high risk of developing certain diseases. Despite the potential for side effects and physical changes, the decision to perform it is made after careful medical evaluation and a thorough discussion between the patient and the medical team. Adherence to medical follow-up and health instructions after surgery contributes to improving treatment outcomes, supporting a safe recovery, and helping the patient adapt to the new phase of her life with confidence and assurance.
Sources:
- National Cancer Institute. (n.d.). Bilateral salpingo-oophorectomy.
- Emory University School of Medicine, Department of Gynecology and Obstetrics. (n.d.). Hysterectomy and bilateral salpingo-oophorectomy (abdominal).
- Mersey West Lancashire NHS Trust. (n.d.). Bilateral salpingo-oophorectomy: Patient information leaflet.