Macular degeneration leads to a gradual decline in the ability to see fine details clearly. It typically develops after the age of 50 and ranks among the top causes of central vision loss worldwide.
Although individuals with macular degeneration do not experience total blindness, they struggle with everyday tasks that rely on sharp central vision, such as reading, driving, and recognizing faces.
What is macular degeneration?
Macular degeneration, also known as age-related macular degeneration (AMD), is a disorder of the macula, the central part of the retina responsible for sharp vision and fine detail. The disease damages the visual cells in the macula, leading to blurring of central vision while peripheral vision remains intact. In the early stages, the patient may notice minor changes such as difficulty distinguishing lines or words. Still, as the condition progresses, a dark area may appear in the center of the eye, making it difficult to read or see faces clearly.
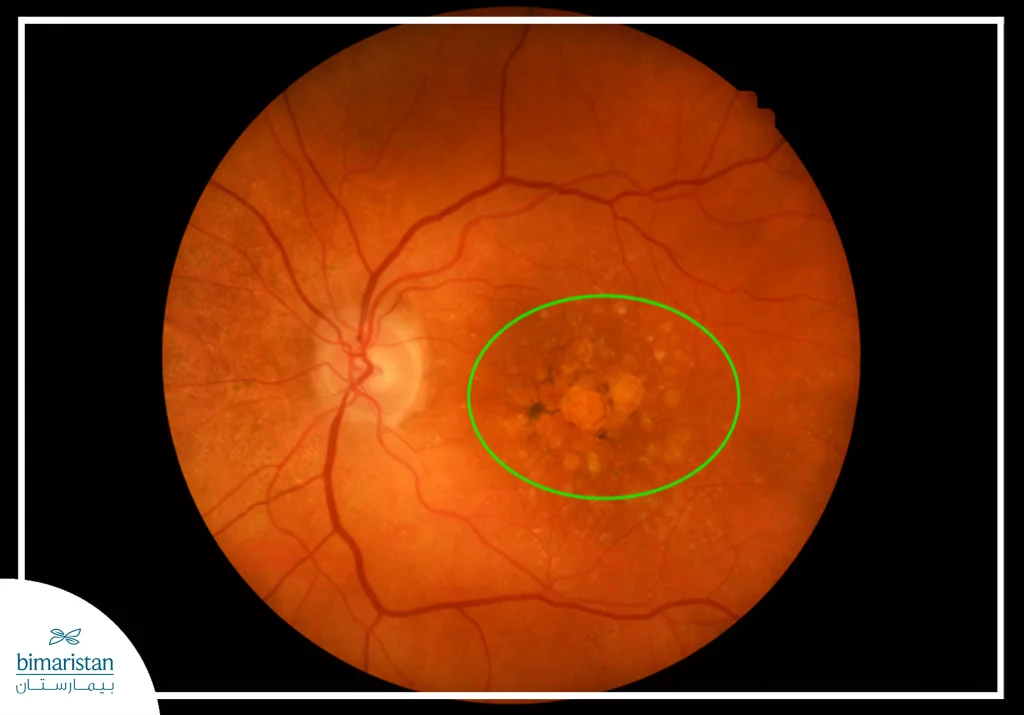
Types of Macular Degeneration
Age-related macular degeneration (AMD) is divided into two main types: Dry macular degeneration and wet macular degeneration, which differ in mechanism and speed of progression of vision loss.
1. (Dry macular degeneration (Dry AMD
It is the most common form, affecting about 80% of patients with macular degeneration. This type occurs gradually as the visual cells in the macula degenerate and do not regenerate, leading to thinning of the retina and impairment of central vision over time.
It is characterized by tiny yellow deposits known as drusen, which are collections of fats and proteins that accumulate behind the retina due to the body’s poor ability to eliminate cellular waste. As these deposits increase in size, oxygen and nutrients to the visual cells are reduced, and they gradually die and vision distortions appear, such as seeing straight lines as wavy.
In advanced stages, this type is known as geographic atrophy due to the severe thinning of the macular tissue. There is still no cure for dry degeneration, but its progression can be slowed through a healthy lifestyle that includes stopping smoking, eating a diet rich in antioxidants, and controlling blood pressure and weight.
2. Wet macular degeneration (Wet AMD)
It is the least common but most serious form, affecting about 10-15% of cases and often developing suddenly and rapidly. It develops when abnormal blood vessels grow under the macula, as the body attempts to compensate for the lack of nutrition caused by the dry type. However, these vessels are fragile and leak fluid or blood, causing scarring of the macula and acute loss of central vision within a short period of time.
Also known as Neovascular AMD, this form of macular degeneration is now effectively treated by injecting anti-VEGF drugs into the eye, which help stop the leakage of blood and fluid, prevent the progression of the disease, and, in some cases, may improve vision with early treatment.
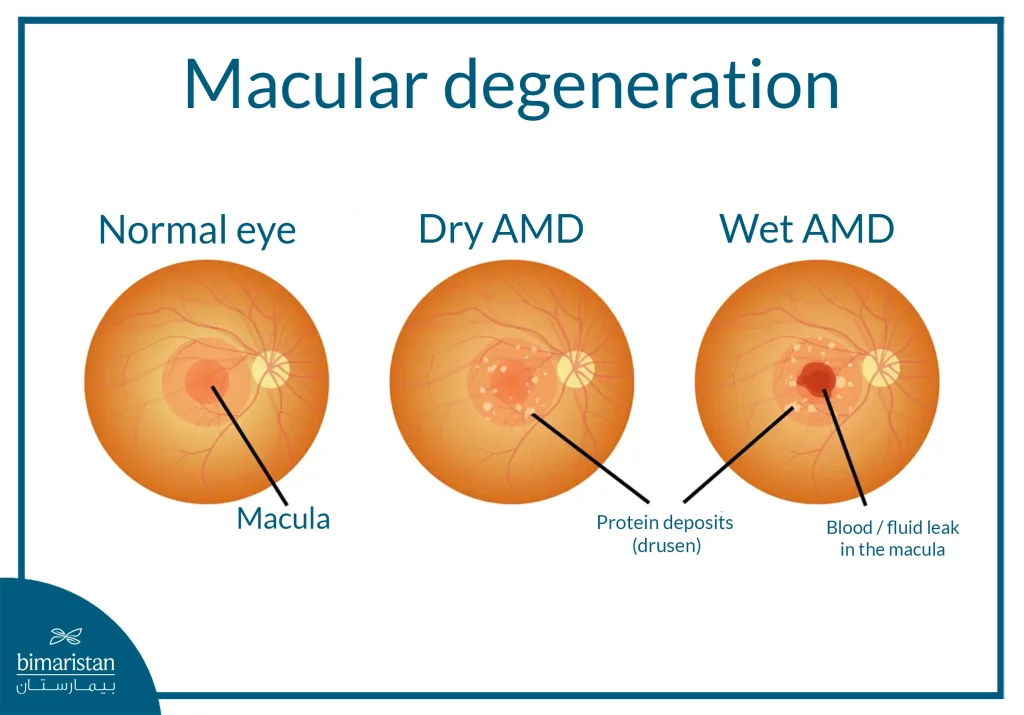
Symptoms of macular degeneration
Macular degeneration can progress slowly and without obvious symptoms in its early stages, making early detection difficult in many cases. Patients often begin to notice symptoms as the disease progresses to more advanced stages. Macular injury disrupts image processing between the eye and the brain, making it difficult for the brain to interpret what the eye sees correctly. As the condition progresses, the following symptoms may occur:
- Seeing straight lines as wavy or curved is a hallmark of the disease
- Blurry or hazy central vision that makes it difficult to read or see fine details
- Difficulty seeing in low light or when moving from light to dark
- Difficulty recognizing faces or performing delicate tasks such as sewing or reading
- Dark spots or empty areas in the center of the field of vision
- Impaired or altered color perception
In the advanced stage of macular degeneration, whether caused by the advanced dry form (geographic atrophy) or the wet form, symptoms become more pronounced and are often centered on loss of central vision with lateral vision remaining intact.
Stages of macular degeneration
Age-related macular degeneration (AMD) has four main stages that progress gradually over time:
- Sub-clinical AMD: In this stage, there are no visible changes to the macula, but the patient begins to lose their ability to adapt to darkness or experience poor night vision. The doctor can detect these changes only through specialized tests.
- Early AMD: Usually detected during a routine eye exam with no obvious symptoms, small yellowish deposits known as drusen are observed under the retina, and there is no loss of vision yet.
- Intermediate AMD: Some symptoms begin to appear, such as mild blurred vision or difficulty seeing in low light, and the doctor notices larger drusen and changes in retinal pigmentation during the examination.
- Late AMD: This is the most serious stage, as loss of central vision becomes evident. It can be due to advanced dry degeneration (geographic atrophy) caused by thinning of the macula, or wet degeneration caused by the growth of abnormal blood vessels that leak fluid, causing scarring and rapid loss of vision.
Causes and contributing factors of macular degeneration
Macular degeneration arises from a complex interaction between genetic and environmental factors that affect the cells of the macula, leading to progressive weakening. In some instances, the condition is hereditary, but it can also develop in individuals without any family history of the disease. Although the exact cause is not known, there are a number of factors that increase the likelihood of developing or accelerating the progression of the disease:
- Age: The risk increases significantly after the age of 50, as the ability of retinal cells to regenerate is impaired.
- Genetic factors: Having a family history increases the likelihood of developing the disease due to genetic mutations associated with macular degeneration.
- Smoking: It doubles the risk of injury, weakens the tiny blood vessels in the eye, and accelerates the deterioration of retinal tissue.
- High blood pressure and diabetes: These weaken the tiny vessels supplying the macula and contribute to macular damage.
- Alcohol and obesity: They reduce the effectiveness of antioxidants and negatively affect blood supply to the eye.
- Overexposure to sunlight: It leads to chronic oxidative damage to retinal cells.
- Racial factors: White people are more likely to be affected than people of other races.
- Unhealthy diet: Eating foods high in saturated fats and sugars and low in vegetables, fruits, and antioxidants increases your risk.
- Rare factors: Such as severe head injuries, certain eye infections, or chronic nutritional deficiencies.
Diagnosis of macular degeneration
Macular degeneration often does not cause noticeable symptoms in its early stages, so regular eye examinations are essential to detect the disease early and start treatment at the most appropriate time. During a comprehensive eye examination, the ophthalmologist will assess the retina and macula using a range of specialized tests to determine the type and stage of degeneration. Some of the most important diagnostic methods used are:
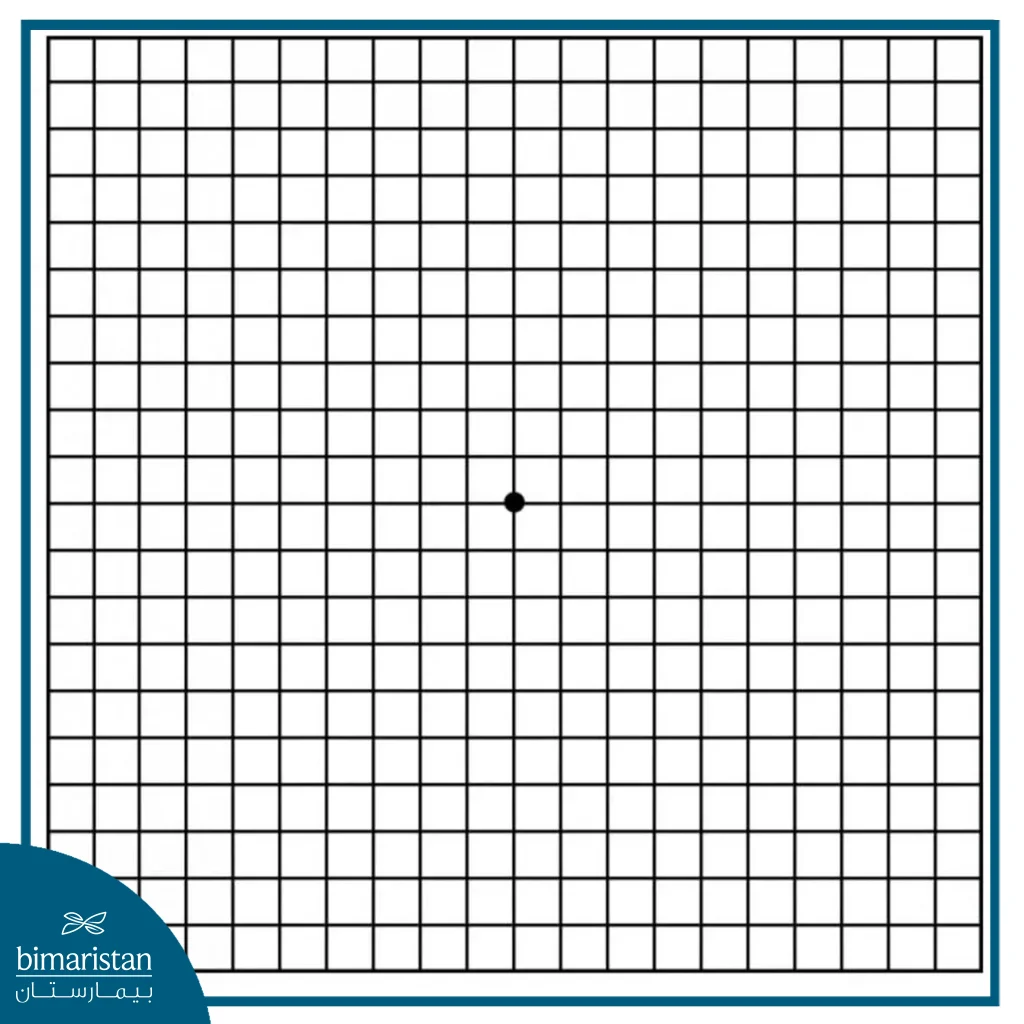
- Amsler grid test: A grid of straight lines with a dot in the center. The patient is asked to focus on the dot and report whether the lines appear wavy or if any lines seem to be missing. This test helps detect early visual abnormalities and allows for monitoring the progression of the condition at home.
- Fluorescein angiography: A fluorescein dye is injected into a vein in the arm, and then serial images of the eye are taken to assess blood flow and detect leakage or abnormal growth of vessels under the retina.
- Optical coherence tomography: An advanced imaging technique that uses light beams to create high-resolution cross-sectional images of the retina and macula, and is one of the most important tests in monitoring the disease, as it is painless and non-invasive.
- Optical coherence tomography angiography: Uses the reflection of light instead of dye to generate three-dimensional images of blood flow in the eye in a matter of seconds.
- Dilation eye exam: Drops are used to dilate the pupil, then the doctor examines the fundus with a special lens to see details of the retina and macula.
The combination of these tests helps diagnose the type and stage of macular degeneration, enabling the doctor to develop an appropriate treatment plan. People over the age of 60 are recommended to have an eye exam every 2 years, and to have it repeated annually after the age of 70, for early detection of macular changes.
Macular degeneration treatment
There is still no definitive cure for macular degeneration, but starting treatment early can slow the progression of the disease and reduce symptom severity, helping the patient maintain their vision for as long as possible. Treatment options vary depending on the type of degeneration, with dry and wet degeneration each having specific approaches.
Dry macular degeneration treatment
This type of treatment aims to support retinal cells and slow down their deterioration through the following means:
- The AREDS and AREDS2 studies have shown that a combination of vitamins and minerals can slow the progression of the disease, including vitamin C, vitamin E, zinc, copper, lutein, and zeaxanthin.
- Beta-carotene has been replaced in modern formulas with safer antioxidants to reduce the risk of lung cancer among smokers.
- A diet rich in leafy greens, fruits, and fish helps minimize the impact of free radicals and improve retinal health.
- In cases of advanced geographic atrophy, newer intraocular medications such as Pegcetacoplan and Avacincaptad pegol can be used to slow macular atrophy and delay vision loss.
Wet macular degeneration treatment
This type of treatment focuses on reducing the growth of abnormal blood vessels and fluid leakage under the retina, and includes the following:
- Intraocular injections of anti-VEGF (anti-vascular endothelial growth factor) drugs, which prevent leaky vessels and stabilize or improve vision
- The injections are administered under local anesthesia by a doctor who specializes in retinal diseases. Drugs used include Ranibizumab (Lucentis), Aflibercept (Eylea), Bevacizumab (Avastin), Faricimab (Vabysmo), and Brolucizumab (Beovu)
- Photodynamic therapy (PDT) involves injecting a photosensitive substance into a vein and then activating it with low-energy lasers to destroy the abnormal vessels without damaging healthy tissue
- Laser Photocoagulation, which is used in some cases to close leaky vessels, but is less common today due to the availability of safer and more effective alternatives
Lifestyle and macular degeneration treatment
Adhering to a healthy lifestyle helps to enhance the effectiveness of treatment and delay the progression of the disease:
- Stop smoking altogether
- Control blood pressure and blood sugar levels
- A diet rich in antioxidants and vitamins
- Engage in regular physical activity and maintain a healthy weight
Possible side effects of macular degeneration treatment
Some treatments, especially intraocular injections, carry limited risks such as:
- Inflammation or infection inside the eye
- Temporarily high eye pressure
- Retinal detachment or structural damage
The patient should commit to regular follow-up with the ophthalmologist to ensure optimal results and minimize potential complications.
Macular degeneration complications
Advanced macular degeneration leads to loss of central vision, making it difficult to perform daily activities. Major complications include:
- Difficulty reading, recognizing faces, driving, or doing delicate tasks such as cooking and sewing
- Severe central vision loss that can lead to legal blindness
- Psychological disorders such as depression and anxiety, as a result of the loss of independence
- Charles Bonnet syndrome, a condition that causes visual hallucinations in some patients
- The need for low vision aids, such as magnifying glasses or large print materials
- The importance of visual rehabilitation and training to use side vision to cope with the loss of central vision
Psychological support and regular follow-ups with your ophthalmologist help you adapt to the disease and maintain as much quality of life as possible.
When to see a doctor
It is advisable to consult an eye specialist promptly if you notice any changes in your vision, especially blurriness, waviness in straight lines, or dark spots in the center of your sight. Sudden difficulty in reading or seeing fine details should never be ignored. Individuals over 50 are encouraged to undergo regular eye exams even without symptoms, as early detection of macular degeneration can significantly slow its progression and help preserve vision.
Macular degeneration is a leading cause of central vision loss, but timely diagnosis and consistent follow-up can reduce its impact. Bimaristan Medical Center in Turkey provides advanced diagnostic and treatment solutions under the care of expert ophthalmologists to ensure optimal eye health.
Sources:
- American Macular Degeneration Foundation. (2025). What is macular degeneration? Retrieved October 21, 2025,
- Macular Society. (2025). What is macular degeneration? Retrieved October 21, 2025,
