Central retinal vein occlusion (CRVO) is one of the most common ocular vascular disorders and occurs when the main vein draining the retina is partially or completely blocked, leading to blood and fluid pooling in the retina and sudden vision impairment.
This blockage often affects only one eye and appears suddenly or gradually over a period of hours or days. Although some patients may have no obvious symptoms, most experience blurring or sudden loss of vision, and in some cases may be accompanied by black floaters or pain and pressure inside the eye.
What is central retinal vein occlusion?
A central retinal vein occlusion occurs when a blood clot (thrombus) forms inside the main retinal vein, the vessel that drains blood from the retinal tissue into the general circulation. This blockage leads to reduced blood drainage and fluid retention within the retina, causing edema (swelling) in the central area responsible for acute vision (the yellow smudge).
This condition leads to blurry or loss of central vision due to damage to the photoreceptors caused by a lack of oxygen (ischemia). In severe cases, abnormal blood vessels can form on the surface of the retina or iris, which can cause bleeding inside the eye and high internal pressure (vascular glaucoma). The disease usually occurs in adults over the age of 60 and is more common in people with high blood pressure, diabetes, or blood clotting disorders.
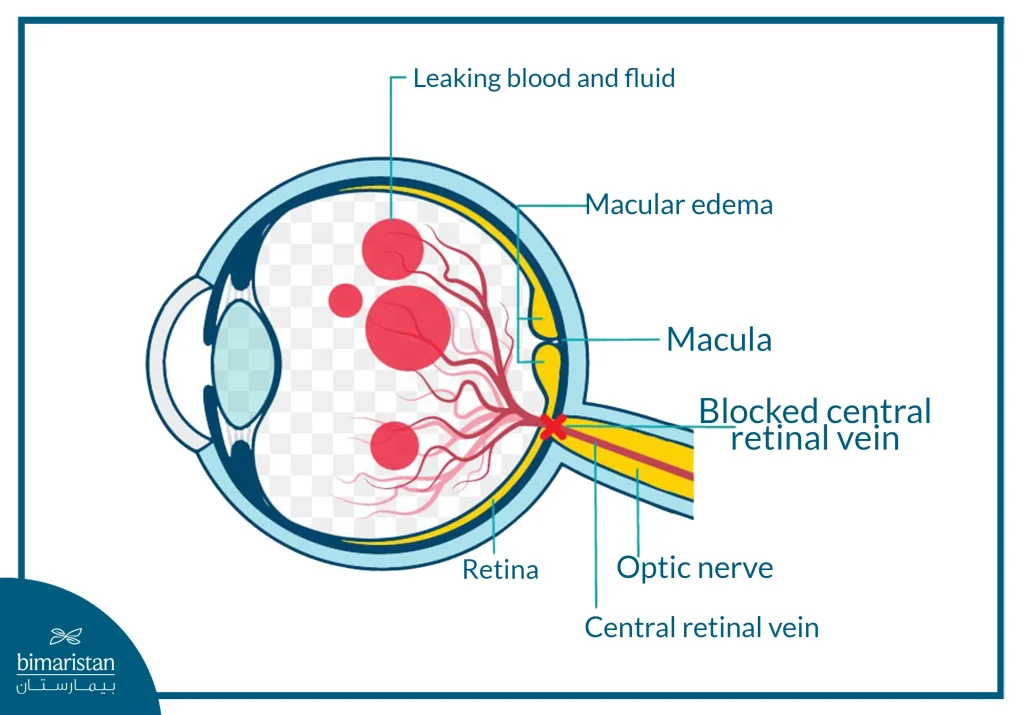
Types of central retinal vein occlusion
Central retinal vein occlusion (CRVO) is divided into two main types, which differ in terms of the severity of the occlusion and its effect on blood perfusion in the retina:
- Non-Ischemic CRVO
- The less severe and more common form
- This is accompanied by blood leakage from the tiny vessels within the retina, leading to blurred vision or partial vision loss.
- Retinal blood supply is often partially preserved, giving a better chance of visual improvement.
- Ischemic CRVO
- The more severe form of CRVO
- This leads to a decrease or interruption of blood flow to the retina and a severe lack of oxygen, causing permanent vision loss in some cases.
- It may lead to the growth of abnormal blood vessels in the iris or retina, causing bleeding or angioedema.
There is another type called Branch Retinal Vein Occlusion (BRVO), which is similar but affects a branch of the vein rather than the main vein, and the symptoms are more localized and less severe.
Causes of central retinal vein occlusion
The immediate cause is the formation of a blood clot within the central retinal vein, which prevents normal blood flow. However, there are several factors that increase the risk of injury, most notably:
- Chronic high blood pressure that weakens blood vessel walls
- Diabetes that causes damage to the tiny vessels within the retina
- High cholesterol and triglycerides increase blood viscosity and the likelihood of clotting
- Aging, especially after the age of 60
- Smoking affects the elasticity of blood vessels and increases the risk of clots
- Glaucoma, where high intraocular pressure leads to poor venous outflow
- Inflammatory eye diseases such as uveitis or retinal vasculitis
- Coagulation disorders that cause an excessive tendency to form clots
In some rare cases, vein occlusion in both eyes can occur simultaneously, often indicating a systemic blood disease or clotting disorder that requires a thorough medical evaluation.
Symptoms of central retinal vein occlusion
The severity of symptoms in central retinal vein occlusion (CRVO) varies depending on the degree of blockage and the extent to which retinal blood flow is affected. Some mild cases may go without obvious symptoms, while most patients experience a decrease in visual acuity or sudden blurred vision in one eye. Symptoms usually appear gradually over hours or days, and include the following:
- Loss or blurred vision: The most common symptom, which may be partial or complete in one eye, is caused by a buildup of fluid in the center of the retina (the yellowish-yellow smudge).
- Distorted or wavy vision: The result of swelling in the central area of the retina.
- Redness and irritation in the eye: Especially when abnormal blood vessels grow, causing secondary infections.
- Seeing black floaters: These are dark spots or streaks caused by small clumps of blood leaking into the vitreous inside the eye.
- Intermittent blurring or darkening of vision: Known as “transient vision disorders,” these may come and go frequently in the early stages.
- Pain or pressure inside the eye: Appears in severe cases or when complications such as glaucoma develop due to high intraocular pressure.
In most cases, only one eye is affected, but when both eyes are affected, it may indicate a generalized blood or clotting disorder that needs a thorough medical evaluation.
Diagnosis of central retinal vein occlusion
The diagnosis of central retinal vein occlusion is based on a careful clinical examination of the eye along with a range of advanced imaging tests. The doctor usually starts by dilating the pupil with special drops and then examining the retina to assess for bleeding and swelling. Basic diagnostic tools include the following:
1. Clinical eye examination
The ophthalmologist dilates the pupil using special drops and then examines the retina using an ophthalmoscope. The examination usually shows flame-shaped retinal hemorrhages and swelling of the retina or optic nerve, typical signs of central venous occlusion. Visual acuity, color discrimination, and field of vision are also assessed to estimate how much the occlusion affects vision.
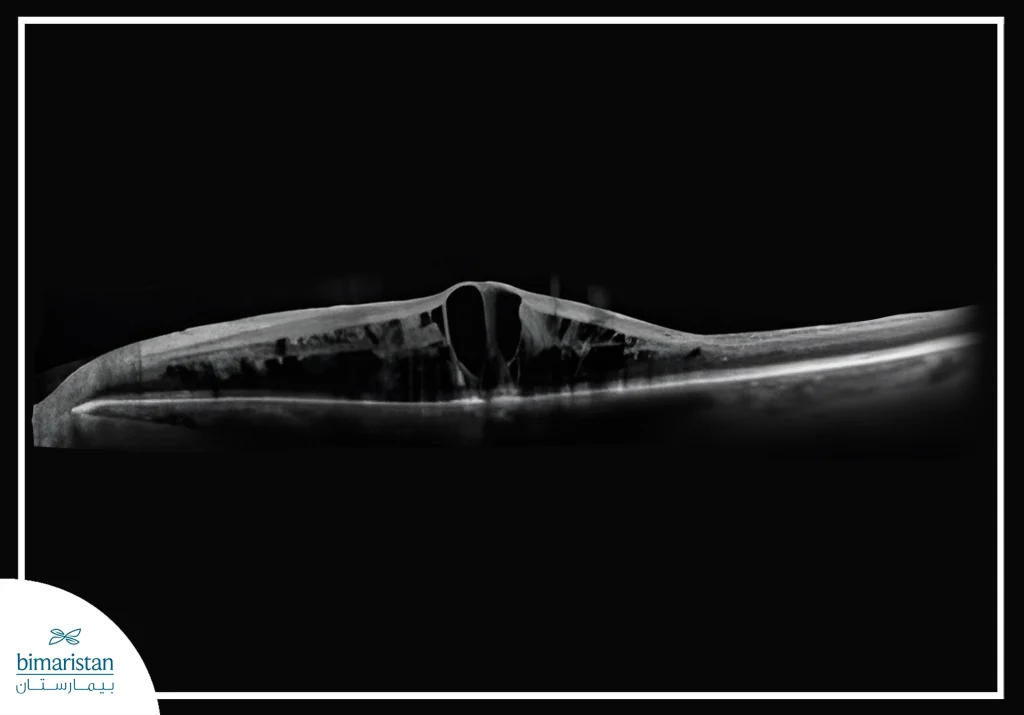
2. Optical coherence tomography
One of the most important modern tests for retinal evaluation, it detects the edema of the yellow smudge caused by the accumulation of fluid in the center of vision and accurately measures the thickness of the retinal layers, and helps follow the progression of the condition and the patient’s response to injection or laser treatment.
3. Fluorescein angiography
A yellow fluorescein dye is injected into a vein in the arm, and then sequential images of the retina are taken as the dye passes through the vessels. The scan shows areas of blocked vessels, ischemia, leaking blood, and abnormal vessels, and is also used to differentiate CRVO from similar diseases such as diabetic retinopathy.
4. Optical coherence angiography
A new dye-free technique that provides detailed images of the tiny blood vessels within the retina. It is useful for accurately assessing retinal blood flow and tracking subtle changes over time.
5. Laboratory tests
It is performed to check for systemic diseases that may be causing the blockage, such as:
- Diabetes
- High blood pressure
- Lipid and cholesterol disorders
- Blood clotting disorders: Especially recommended for young people under 40 years of age or when both eyes are clogged.
6. Additional tests and differential diagnosis
An examination with a hematologist or internist may be ordered to rule out systemic causes. Your doctor will also aim to distinguish CRVO from other retinal diseases, such as:
- Diabetic retinopathy
- Retinopathy due to anemia or thrombocytopenia
An accurate diagnosis aims to determine the degree and type of obstruction (ischemic or non-ischemic) and rule out other diseases that may resemble it such as diabetic retinopathy or anemia and thrombocytopenia, which helps in developing an effective treatment plan to preserve vision.
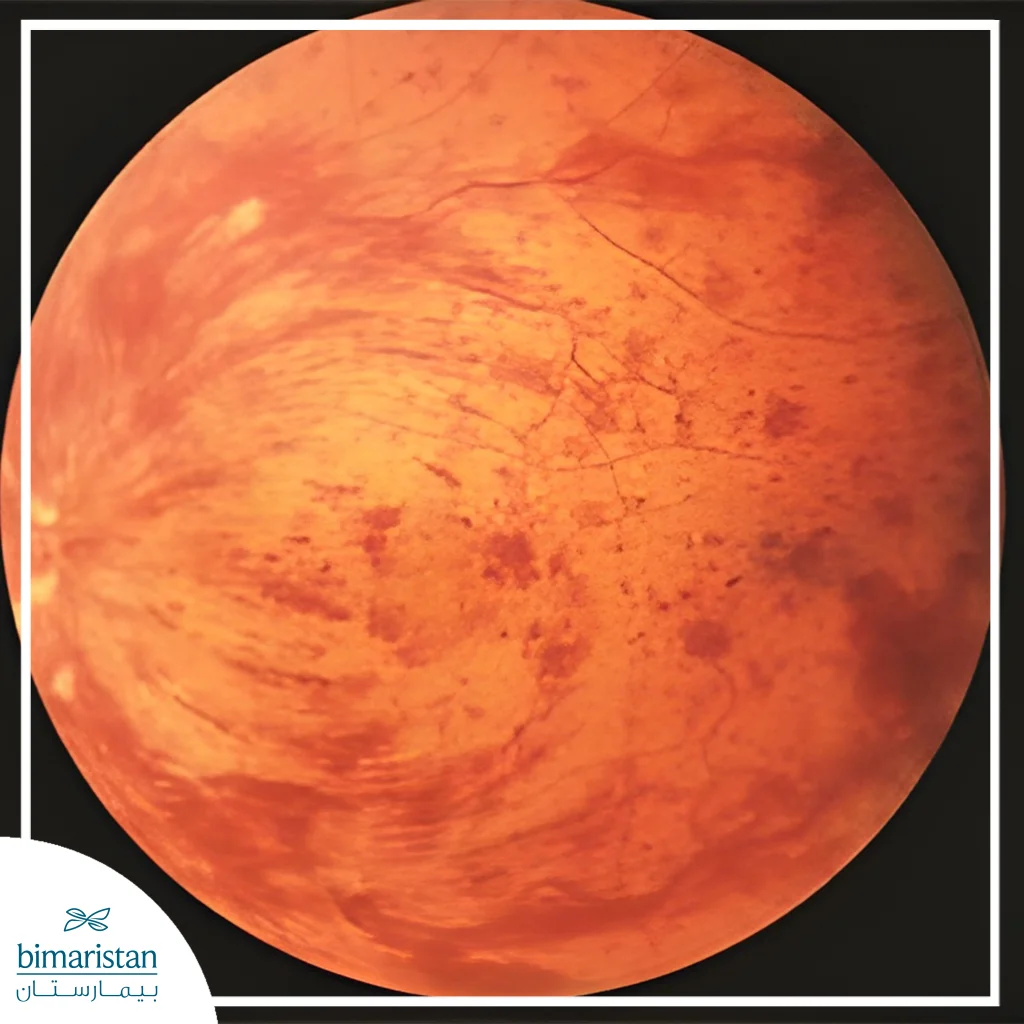
Central retinal vein occlusion treatment
There is no complete cure for central retinal vein occlusion (CRVO), but the goal of treatment is to preserve vision and prevent worsening retinal damage. The treatment plan depends on the type of blockage (ischemic or non-ischemic) and the severity of the swelling or associated complications.
1. Intraocular injections
It is the most commonly used treatment today and is administered directly into the vitreous body of the eye:
Anti-VEGF
such as ranibizumab (Lucentis®), aflibercept (Eylea®) and bevacizumab (Avastin®). These drugs work by inhibiting VEGF, which is responsible for fluid leakage and abnormal blood vessel formation in the retina, reducing macular edema and improving vision. Treatment usually begins with four consecutive monthly injections, followed by injections spaced as the patient responds.
Intraocular steroids
such as triamcinolone or dexamethasone (Ozurdex®), help reduce inflammation and minimize swelling of the spot. The Ozurdex implant lasts about 4 to 6 months and is repeated as needed. Possible side effects include high eye pressure or cataract formation, which can often be controlled with medication or surgery if necessary.
2. Laser therapy
In severe cases where abnormal blood vessels form within the retina or on the iris, the diffuse retinal laser is used. The laser stops the growth of the abnormal vessels, prevents bleeding inside the eye, and reduces the risk of vascular glaucoma. This treatment does not improve central vision, but it protects the eye from future complications.
3. Periodic follow-up and visual rehabilitation
After starting treatment, the doctor monitors visual improvement through OCT and visual field scans and adjusts the injection or laser intervals according to the response.
In some cases where permanent vision loss occurs, the patient can benefit from vision rehabilitation programs and low vision aids to improve the quality of daily life.
Early treatment with Anti-VEGF or steroid injections is key to improving visual outcome, while delaying treatment increases the risk of permanent complications.
Possible complications of central retinal vein occlusion
Central retinal vein occlusion can lead to a number of potentially sight-threatening complications if not treated early, including:
- Chronic macular edema: This is the most common cause of long-term vision impairment.
- Cataract formation: The result of prolonged use of intraocular steroids.
- Permanent damage to the retina: Especially in ischemic or neglected cases, it can lead to irreversible visual loss.
- Abnormal blood vessel growth: These can cause bleeding within the vitreous or in the iris.
- Vascular glaucoma: Severely elevated eye pressure due to blockage of the fluid drainage pathway.
- Intraocular infection: This is a rare complication after ocular injection (about 1 per 1000 patients) but can cause complete loss of vision if not treated promptly.
Prevention of central retinal vein occlusion
While some conditions cannot be completely prevented, adhering to a healthy lifestyle can significantly reduce the risk of injury or recurrence of blockages. Preventive measures include:
- Control blood pressure, diabetes, and cholesterol through regular monitoring and proper treatment
- Quit smoking, which increases the risk of blood clots and atherosclerosis
- Regular moderate physical activity to improve circulation
- Avoid obesity and a sedentary lifestyle
- Treat any clotting or inflammatory disorder of the eye or blood early
- Regular eye exams, especially for elderly patients or those with heart disease, high blood pressure, and diabetes
Central retinal vein occlusion is one of the causes of sudden vision loss, but early diagnosis and regular treatment with VEGF antagonist injections or lasers can help preserve vision. Bimarestan Medical Center in Turkey offers the latest treatment options under the supervision of top ophthalmologists.
Sources:
- National Eye Institute. (2024, November 27). Central retinal vein occlusion (CRVO). National Institutes of Health.
- East & North Hertfordshire NHS Trust. (n.d.). Treatment – Central Retinal Vein Occlusion (CRVO) .