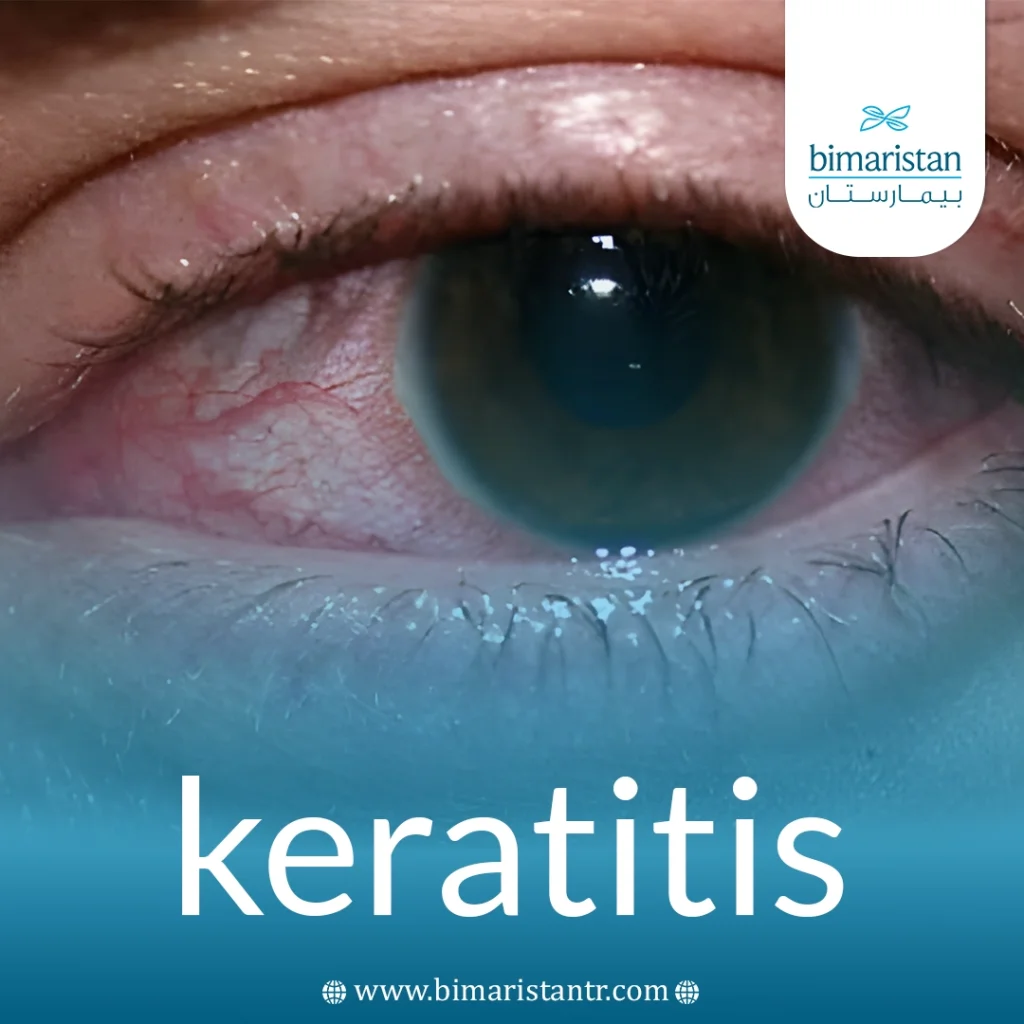
Keratitis is an inflammation that affects the front transparent layer of the eye, called the cornea, which covers the iris and pupil and maintains clear vision. This condition may be contagious or non‑contagious, arising from simple injuries such as prolonged contact lens use or the entry of a foreign body into the eye, or from bacteria, viruses, fungi, or parasites.
In mild to moderate cases, keratitis is usually treated successfully without impairing vision, but if left untreated, it may lead to serious complications, including corneal ulcers or permanent vision loss.
What is keratitis?
Keratitis is the medical term for inflammation or irritation of the cornea, which can progress to a corneal ulcer in severe cases. Keratitis is divided into two main types: contagious inflammation caused by microorganisms such as bacteria, viruses, or fungi, and non-contagious inflammation caused by mechanical irritation, dryness, or superficial injury. Globally, keratitis is a significant cause of corneal transparency loss and permanent visual impairment, especially if left untreated.
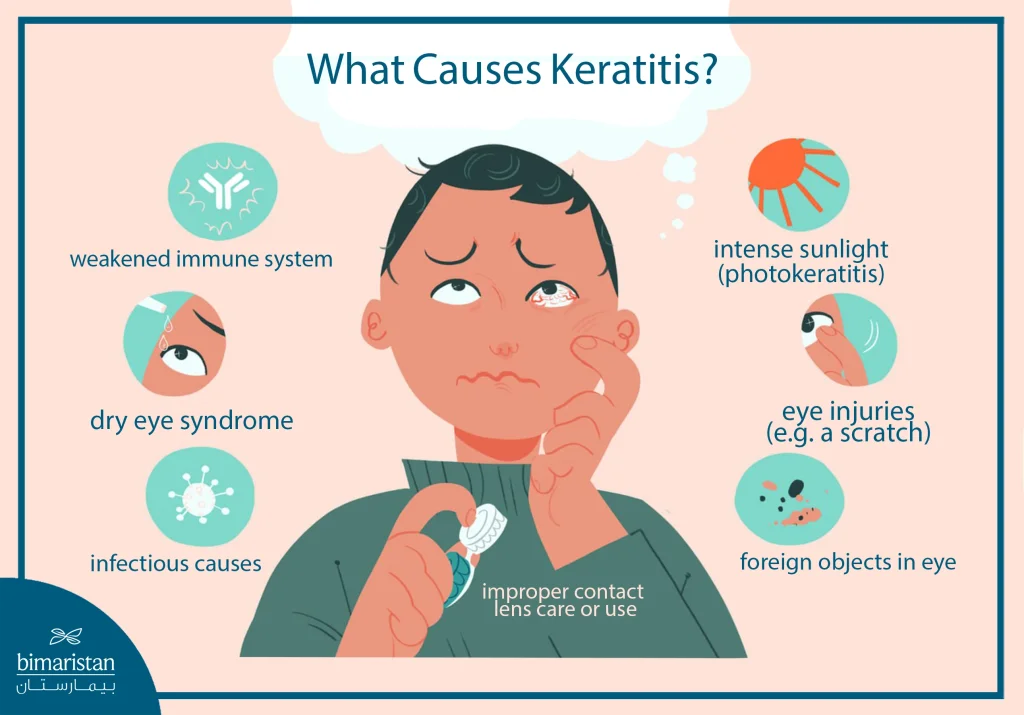
Causes of keratitis
Keratitis is the inflammation of the transparent layer that covers the front of the eye, which can occur due to either contagious or non-contagious irritation. The causes of keratitis can be categorized into two main types: contagious and non-contagious irritants.
Contagious causes of keratitis
Contagious causes include infections caused by different types of microorganisms, such as:
- Bacteria: The most common cause of keratitis, especially in contact lens users, includes Staphylococcus, Streptococcus, and Pseudomonas.
- Viruses: The most prominent are the herpes simplex virus, which causes frequent attacks, and the Varicella zoster virus, which may infect the eye after infection with chickenpox or shingles.
- Fungi: May be transmitted to the eye after a direct injury or improper use of lenses or cortisone drops, often from a plant source.
- Parasites (amoeba – Acanthamoeba): These are microscopic organisms found in fresh water and soil that cause severe inflammation, especially in people who wear contact lenses while swimming.
Non-contagious causes of keratitis
- Mechanical corneal injuries, such as scratches or a foreign object entering the eye
- Prolonged exposure to ultraviolet light (as in snowy eyes)
- Wearing contact lenses for long periods of time or without proper sterilization
- Chronic dry eye or vitamin A deficiency
- A weakened immune system or the use of medications that reduce the immune response
- Eyelid disorders, such as Bell’s palsy or eyelid eversion, which prevent regular eye lubrication
Symptoms of keratitis
Symptoms of keratitis range from mild to severe and may affect one or both eyes. The most common signs and symptoms include:
- Eye redness and blood vessel congestion
- Noticeable pain in the eye and a feeling of a foreign object or sand inside
- Increased tear production or the appearance of sticky or purulent discharge
- Blurred vision or a gradual decrease in visual acuity
- Extreme sensitivity to light (photophobia)
- Difficulty opening the eye due to pain or irritation
- Swollen eyelids or a white spot on the cornea in advanced cases
Symptoms can develop quickly in cases of bacterial or viral infections, so it is advisable to see an ophthalmologist immediately when any of these signs or symptoms appear, as delayed treatment may lead to a corneal ulcer or permanent vision loss.
Diagnosis of keratitis
The diagnosis of keratitis is based on a thorough clinical examination of the eye to determine the cause of the inflammation and its effects on the cornea and other ocular tissues. The doctor usually starts by taking the patient’s medical history and inquiring about symptoms such as pain, redness, blurred vision, or contact lens use.
The eye is then examined using special instruments, such as a Slit Lamp, which provides a magnified, detailed view of the corneal surface to determine the location and depth of the inflammation.
A Fluorescein Stain Test may also be used, where a safe dye is placed in the eye and then examined under a blue light to reveal any ulceration or damage to the corneal surface. In some cases, a sample of tears or a swab of the corneal surface is taken for laboratory analysis or bacterial and fungal culture to determine the exact type of cause, especially if the infection is severe or does not respond to initial treatment.
Light Pentest test may also be performed to assess pupillary response and check for photoreactivity. These tests help the doctor distinguish whether the inflammation is contagious or non-contagious and choose the most appropriate treatment.
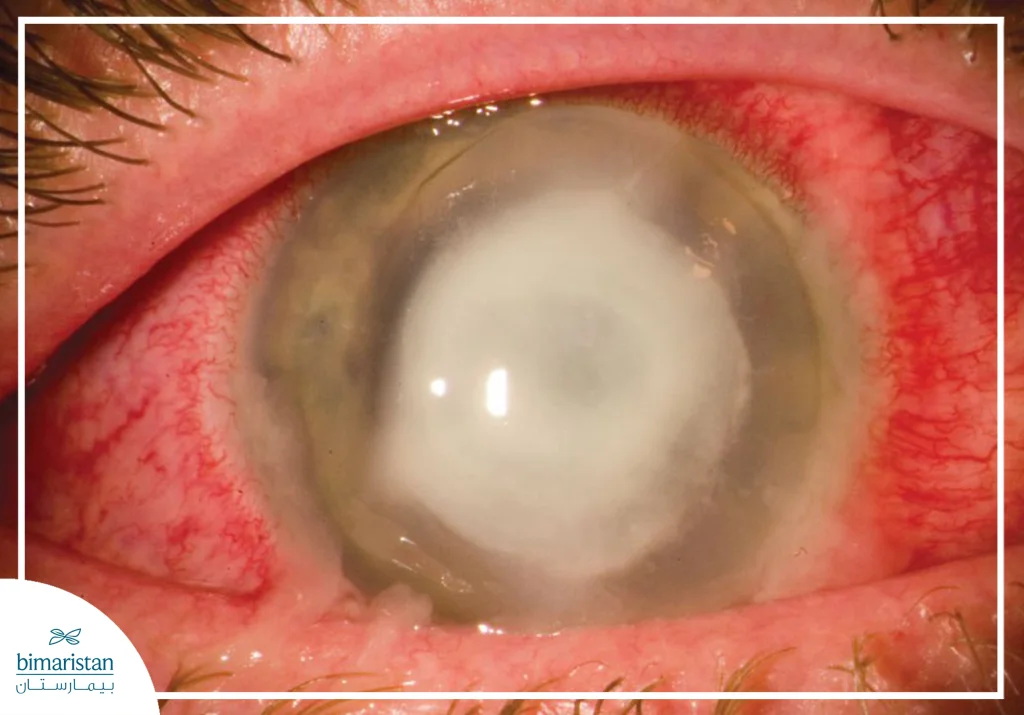
Keratitis treatment
Keratitis treatment depends on the cause and severity of the condition and aims to control inflammation and prevent corneal complications or scarring. In non-contagious cases, the doctor may use artificial tear drops to moisturize the eye and relieve minor symptoms caused by superficial scratching or irritation, while more severe cases require anti-inflammatory drops or therapeutic protective lenses to protect the eye while it heals. In contagious keratitis, specific drug therapy is used depending on the cause:
- Bacterial inflammation: The condition is treated with intensive antibiotic drops, sometimes every half hour in severe cases. Oral antibiotics may also be added if necessary.
- Viral inflammation: Antiviral treatment such as Acyclovir or Valacyclovir drops or tablets, sometimes given with supportive drops to relieve pain.
- Fungal inflammation: Requires drops and oral antifungal medications such as Amphotericin or Voriconazole.
- Amoeba inflammation: It is treated with antiparasitic drops for a long time, and the treatment may last for months.
In some severe cases that do not respond to medical treatment, or if deep scarring or ulceration has formed in the cornea, your doctor may recommend a corneal transplant to restore clear vision. After the infection improves, cortisone drops may be used to reduce swelling and prevent scarring, but only under a doctor’s supervision to avoid worsening the infection. Pupil-dilating drops are sometimes prescribed to relieve pain from muscle spasm in the eye, along with rest and avoidance of contact lenses until recovery is complete.
Complications of neglecting to treat keratitis
Neglecting keratitis treatment can lead to a host of complications that can permanently affect your vision, including the following:
- Chronic inflammation of the cornea with permanent scarring and loss of transparency
- An ulcer forms on the surface of the cornea as a result of corneal tissue erosion
- Impaired or blurred vision that may be temporary or permanent
- Recurrent episodes of viral inflammation of the cornea
- Deep corneal perforation or damage in severe cases
- High risk of secondary bacterial or fungal infections
- Partial or complete vision loss can occur if the infection is not treated promptly
Preventing keratitis
The risk of keratitis can be reduced by following simple preventive measures that keep your eyes healthy and your contact lenses clean. The most important guidelines include the following:
- Wash your hands thoroughly with soap and water before touching your eyes or contact lenses.
- Follow your doctor’s instructions on how long to wear your lenses and don’t sleep in them unless your doctor recommends it.
- Clean the lenses daily with sterile solutions designed for your type of lenses; do not use plain water or saliva.
- Replace your lenses and lens case every 3 to 6 months.
- Dispose of the contact lens solution used in the case after each use, and avoid mixing new solution with any remaining old solution.
- Avoid wearing lenses while swimming, bathing, or in hot tubs.
- Avoid touching the eyes when there are herpetic blisters or sores around the mouth to prevent transmission of the virus.
- Use only prescribed eye drops and do not share them with others.
- Wear goggles while working or playing sports to protect your eyes from injuries or foreign objects.
- Wear sunglasses to protect your eyes from UV rays.
Following these simple steps can help prevent keratitis and maintain healthy vision over time.
When should I see a doctor?
See an ophthalmologist immediately if you experience any symptoms of keratitis, such as severe redness, severe pain, blurred vision, or the sensation of a foreign body inside the eye. It is also advisable to seek urgent medical advice for increased tearing, abnormal discharge, or excessive sensitivity to light, as these signs may indicate the onset of a corneal ulcer.
Contact lens users should pay special attention to any persistent irritation or discomfort, and remove the lenses immediately if they experience pain or poor vision. Early detection and prompt treatment minimize the risk of complications and preserve corneal clarity and quality of vision.
Keratitis is a corneal condition that requires early diagnosis and precise treatment to prevent loss of transparency and permanent visual damage. Ignoring therapy or postponing medical consultation may result in severe complications such as corneal ulcers, scarring, or irreversible vision loss. Preventive measures, including proper contact lens hygiene and protection of the eye from trauma, remain the most effective way to prevent keratitis. At Bimaristan Medical Center, keratitis management is delivered using advanced diagnostic and therapeutic methods under the care of corneal specialists, ensuring safe treatment and restoring clear vision with the highest success rates.
Sources:
- American Academy of Ophthalmology. (2024). Corneal Infections (Keratitis).
- Johns Hopkins Medicine. (2023). Keratitis (Corneal Inflammation).
- National Eye Institute. (2024). Corneal Disorders.