With the global surge in obesity and its associated health risks and complications, relying solely on dieticians and nutritional programs is no longer sufficient. Bariatric surgery has become a transformative solution for thousands worldwide. Among the most widely performed procedures are gastric sleeve and biliopancreatic diversion with duodenal switch (BPD-DS), also known as pancreatic bypass, two distinct surgeries. The primary difference between pancreatic bypass and gastric sleeve lies in their surgical approach and their effects on digestion, weight regulation, and chronic conditions such as diabetes.
Understanding the difference between pancreatic bypass and gastric sleeve is crucial when selecting the most suitable procedure. Gastric sleeve primarily reduces stomach size to curb appetite, while pancreatic bypass combines stomach reduction with intestinal rerouting to limit nutrient absorption. This makes the difference between pancreatic bypass and gastric sleeve especially significant in terms of long-term outcomes and nutritional implications.
Turkey has recently gained prominence in bariatric care, offering advanced medical expertise, modern facilities, and competitive pricing, attracting patients globally. As options expand, the difference between pancreatic bypass and gastric sleeve continues to be a key consideration in choosing the optimal path to overcome obesity.
What is Gastric Sleeve?
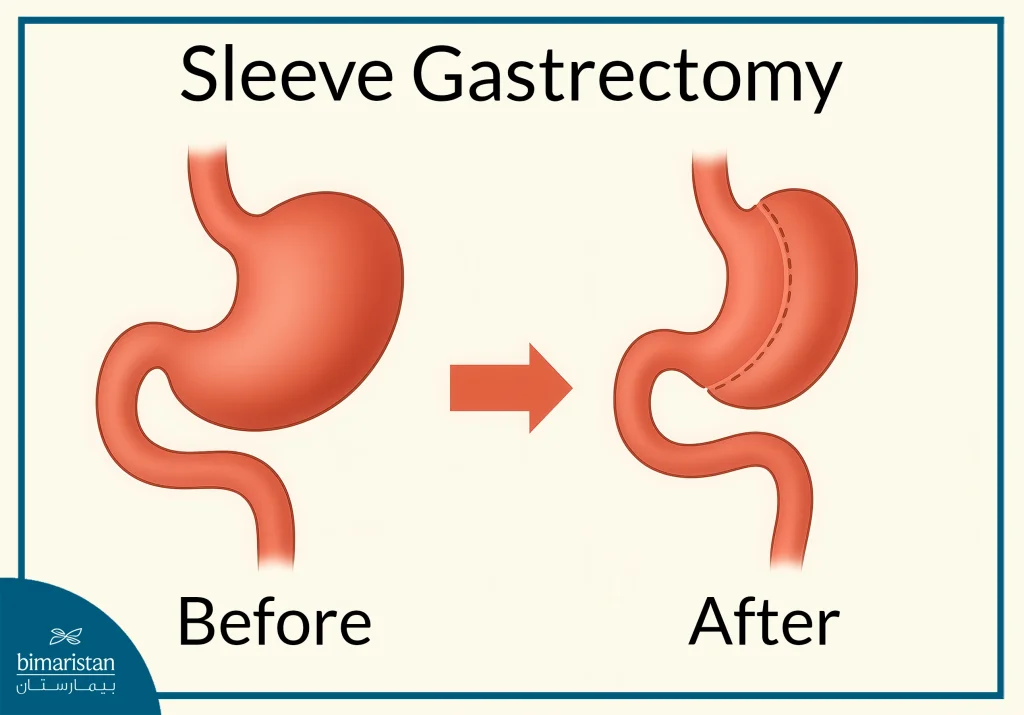
Gastric Sleeve surgery involves reducing the stomach’s natural size, causing it to fill quickly and trigger early satiety, which promotes weight loss with less effort and helps treat obesity. Unlike procedures that alter nutrient absorption, the gastric sleeve works solely by limiting stomach capacity, similar to gastric bypass surgery. This highlights a key difference between pancreatic bypass and gastric sleeve, as the latter does not involve intestinal rerouting or malabsorption mechanisms. By reducing stomach volume, the gastric sleeve also lowers the secretion of ghrelin, the hormone responsible for hunger, thereby decreasing appetite and further supporting weight loss.
Types of Gastric Sleeve
- Laparoscopic Gastric Sleeve: A minimally invasive procedure, sleeve gastrectomy is a popular choice due to its low risk of complications.
- Open Gastric Sleeve: In recent years, it has fallen out of favor as it has a higher rate of complications and risk compared to laparoscopic sleeve gastrectomy.
What is Pancreatic Bypass (BPD-DS)?
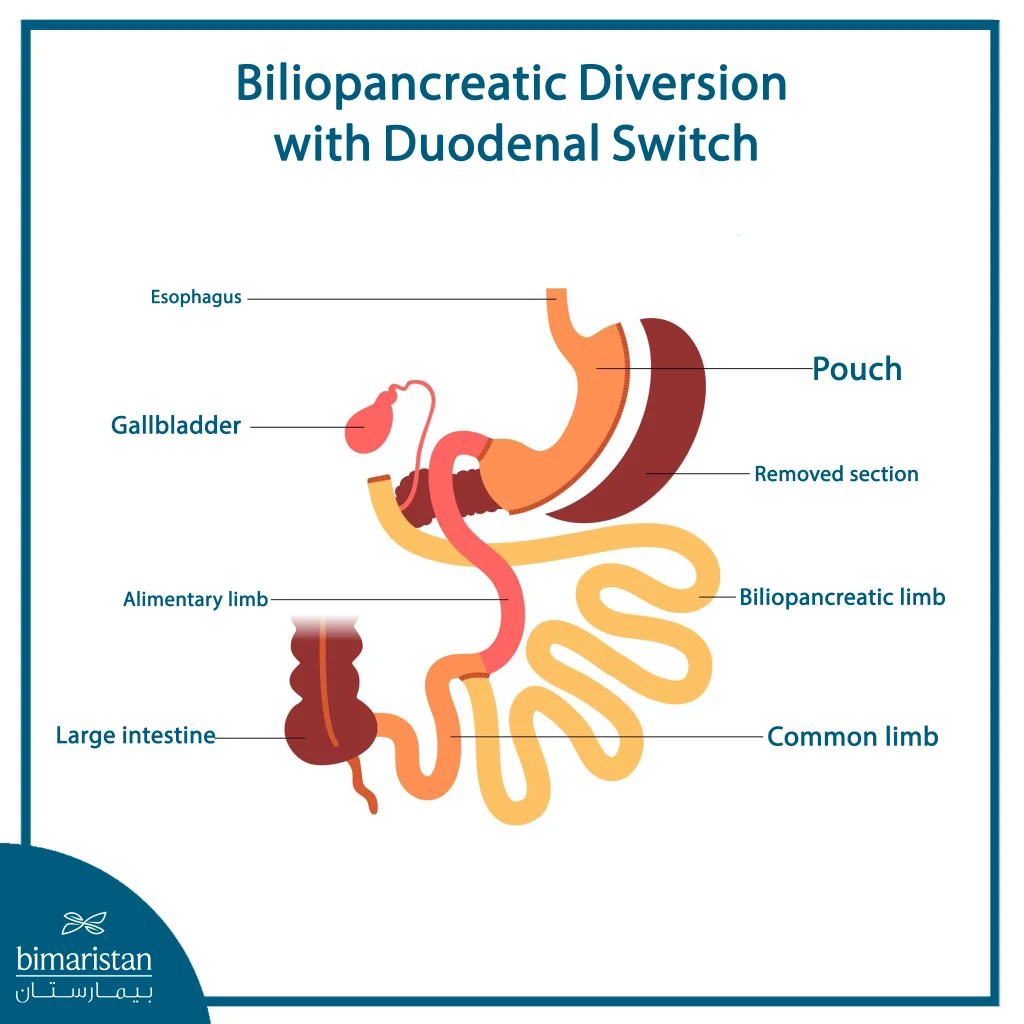
Pancreatic bypass, also known as biliopancreatic diversion with duodenal switch, is a complex bariatric procedure that significantly reduces the absorption of nutrients, vitamins, and minerals. As a result, patients tend to lose more weight with pancreatic bypass compared to gastric sleeve or gastric bypass. However, this increased weight loss comes with a higher risk of nutritional deficiencies, some of which may become life-threatening if not properly managed. When considering surgery, it’s essential to weigh these risks and complications against the potential benefits.
The difference between pancreatic bypass and gastric sleeve lies in their dual mechanisms. Pancreatic bypass promotes weight loss through two pathways: restriction by reducing stomach size (similar to the gastric sleeve) and malabsorption by rerouting the intestines. This combination often leads to more substantial weight loss than gastric sleeve alone, making the difference between pancreatic bypass and gastric sleeve evident in both technique and outcomes.
Studies show that the average excess weight loss after pancreatic bypass surgery reaches approximately 70%, highlighting the procedure’s effectiveness. This reinforces the difference between pancreatic bypass and gastric sleeve in terms of long-term weight reduction and metabolic impact.
What is the difference between pancreatic bypass and gastric sleeve for weight loss?
The difference between pancreatic bypass and gastric sleeve must be understood to determine the mechanism of weight loss, the percentage of weight lost, and its effects on other diseases, such as diabetes. Accordingly, we select the most suitable option based on the patient’s condition and preferences.
What is the difference between pancreatic bypass and gastric sleeve in terms of their weight loss mechanism?
Gastric sleeve relies solely on reducing the size of the stomach, which makes the patient feel full quickly and eat less, but the intestines are not altered or bypassed, so absorption is not affected much. Pancreatic bypass relies on two common factors: reducing the size of the stomach (as in a gastric sleeve), in addition to diverting the intestine to reduce the absorption of calories and fats, which leads to rapid and significant weight loss in a short period of time.
What is the difference between pancreatic bypass and gastric sleeve in terms of weight loss percentage?
Patients undergoing pancreatic bypass surgery typically lose between 70% to 85% of their excess weight within the first 12–18 months. The results appear rapidly, with noticeable weight loss often beginning in the first month. The decline is most pronounced during the initial 3–6 months, contributing to swift improvements in obesity-related conditions such as diabetes and hypertension. After the sixth month, the rate of weight loss slows down, and the weight gradually stabilizes over time.
In comparison, gastric sleeve surgery results in a 50% to 70% reduction in excess weight over the same 12–18 month period. While visible changes begin within the first two months, the pace is slower than that of pancreatic bypass. However, adhering to dietary guidelines and engaging in physical activity can accelerate progress. After month six, the rate of reduction tapers off, and weight stabilization may occur by the second year.
What is the difference between pancreatic bypass and gastric sleeve in their effect on diabetes?
After gastric sleeve surgery, blood sugar levels tend to drop noticeably within the first few weeks, even before significant weight loss occurs. This is because the procedure enhances insulin sensitivity and reduces insulin resistance, resulting in improved glycemic control. Gastric sleeve surgery is particularly effective for patients with type 2 diabetes in its early or uncomplicated stages, due to the reduced stomach size and hormonal changes that influence glucose regulation, especially hormones like GLP-1.
In contrast, pancreatic bypass surgery often results in complete diabetes remission within days or weeks, with many patients achieving complete blood sugar control without medication. The difference between pancreatic bypass and gastric sleeve becomes clear in this context, as pancreatic bypass exerts a more substantial effect on insulin resistance through both nutrient malabsorption and hormonal shifts,especially in the small intestine, where rerouted food flow alters the secretion of diabetes-related hormones.
This makes pancreatic bypass especially suitable for patients with severe or medication-resistant type 2 diabetes, highlighting the difference between pancreatic bypass and gastric sleeve in terms of metabolic impact and diabetes resolution.
What is the difference between pancreatic bypass and gastric sleeve in terms of side effects?
It is essential to understand the difference between pancreatic bypass and gastric sleeve not only in terms of their mechanisms and weight loss effectiveness, but also in relation to their side effects and how to manage them for optimal outcomes. The complications associated with each procedure vary significantly, making the difference between pancreatic bypass and gastric sleeve a critical factor in selecting the most suitable surgical option for each patient.
Research has demonstrated the benefits of gastric sleeve surgery in enhancing insulin sensitivity for diabetic patients, reducing cardiovascular risks, preventing liver cirrhosis, improving thyroid function, alleviating snoring and sleep apnea, boosting self-esteem, and improving overall mood. However, it remains important to consider the potential drawbacks of the procedure. The disadvantages linked to gastric sleeve surgery include the following:
- Surgery-related complications (bleeding, infection, anesthesia issues)
- Gallstones form due to rapid weight loss
- Esophageal reflux
- Gastric sleeve does not affect the absorption of calories, so you may gain weight again when you increase food consumption
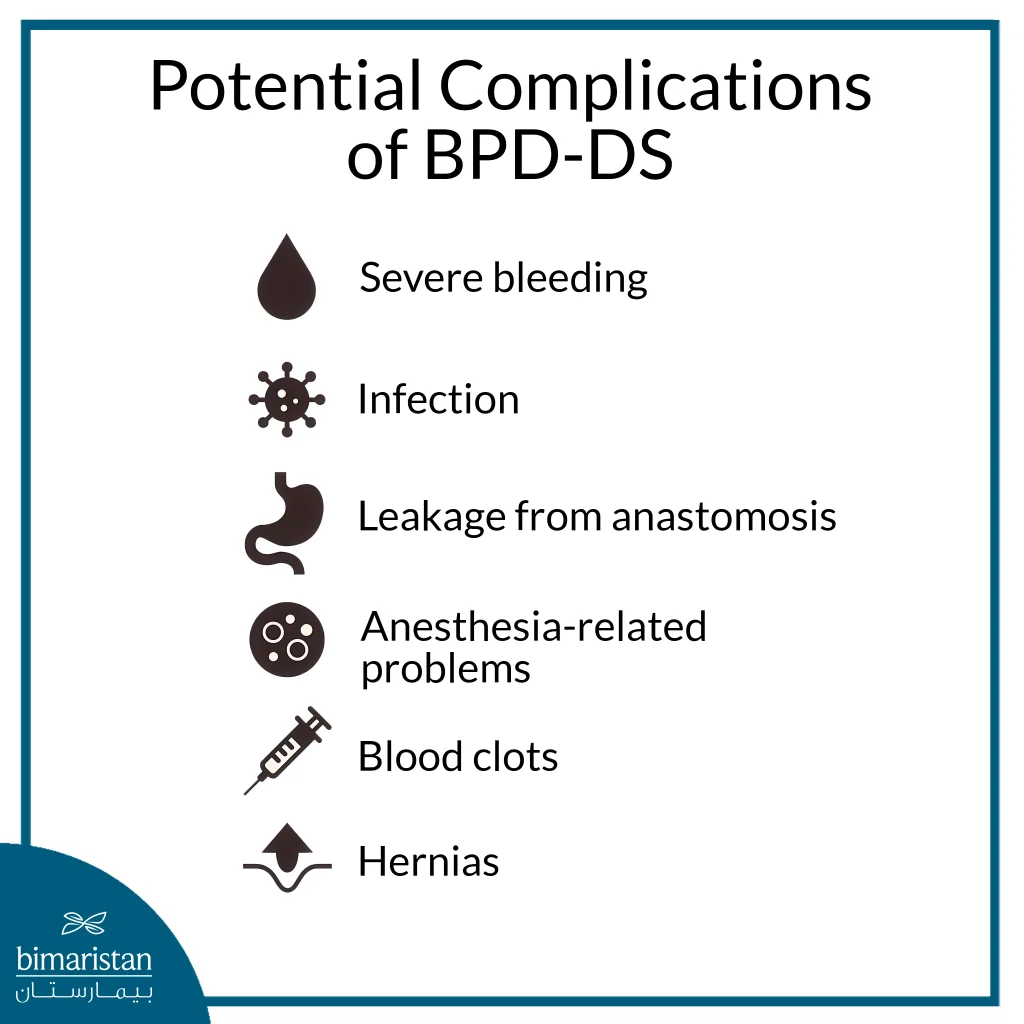
On the other hand, one of the main reasons why pancreatic bypass (BPD-DS) is less commonly performed is its higher risk of side effects compared to other obesity treatments. Understanding the difference between pancreatic bypass and gastric sleeve, as well as other methods like gastric botox injections or smart gastric balloon placement, is crucial when weighing the risks and benefits of each option. Below are the potential complications associated with pancreatic bypass surgery:
- Heavy bleeding
- Infection
- Leak from anastomosis
- Anesthesia-related issues
- Formation of blood clots
- Hernias
In the end, the difference between pancreatic bypass and gastric sleeve is not only about the mechanism of the procedure, but also about knowing the risks and the likelihood of complications after the procedure.
What is the difference between pancreatic bypass and gastric sleeve in follow-up and diet after surgery?
The difference between pancreatic bypass and gastric sleeve in follow-up and diet after surgery lies in the effect each procedure has on food absorption and the way the gastrointestinal tract is handled after surgery. Therefore, the follow-up and dietary requirements differ between the two procedures, which significantly affects the success of the treatment and the patient’s comfort after the procedure.
Pancreatic bypass (BPD-DS)
Pancreatic bypass is one of the most effective bariatric surgeries for nutrient absorption, which necessitates careful and regular follow-up. The American Society for Metabolic and Bariatric Surgery (ASMBS) recommends periodic monitoring of vitamin and mineral levels and prescribing necessary nutritional supplements, typically starting from the second week after surgery. These supplements may include:
- Vitamins A, D, and K: Start taking them within 2-4 weeks after the operation.
- Calcium: Divide into 3-4 daily doses (500-600 mg).
- Vitamin B12: In the form of daily supplements or monthly injections as needed.
- Stick to small, protein-rich meals that include vegetables, fruits, whole grains, and omega-3 fatty acids, and avoid high-sugar foods
A healthy lifestyle after surgery is not limited to diet alone, but also includes regular exercise, ongoing follow-up with the doctor, and periodic laboratory tests. This surgery leads to significant weight loss and improvement in chronic diseases associated with obesity, but in return, it requires a strict lifelong commitment.
Gastric sleeve
Despite the relative ease and simplicity of the procedure, gastric sleeve requires adherence to a healthy lifestyle, especially in the early months. The diet starts with clear, sugar-free, and non-carbonated beverages for one week. Then you move on to pureed foods for 3 weeks. After about 4 weeks, you can gradually start eating regular food. In terms of supplements, vitamins and calcium are prescribed, as well as a monthly vitamin B12 injection, which is often taken for life.
It is common for the body to undergo changes within the first 3 to 6 months, including:
- Muscle pain
- Feeling overwhelmed
- Feeling cold
- Dry skin or hair loss
- Mood swings
Although both operations aim to reduce weight and improve overall health, the difference between them after surgery is clear. Pancreatic bypass requires a strict lifestyle and lifelong dietary supplements to avoid vitamin and mineral deficiencies, while gastric sleeve is easier to care for after surgery, but requires a dietary commitment to maintain the results and prevent weight gain later on.
What is the difference between pancreatic bypass and gastric sleeve in terms of which option is more suitable?
Healthcare providers may recommend pancreatic bypass (BPD/DS) for people who are excessively obese. These people typically have a body mass index (BMI) of 45 or higher, or when other methods have failed, with serious type 2 diabetes and other serious health issues. These health issues include
- Type 2 diabetes
- Sleep apnea
- Heart disease
- Lung diseases
- High blood pressure
- High cholesterol
- Non-alcoholic fatty liver disease
The body mass index (BMI) must be between 35 and 40 for a patient to be a candidate for gastric sleeve surgery, and those with health complications of obesity, such as high blood pressure, diabetes, or sleep apnea, may be accepted for gastric sleeve surgery even if their BMI is less than 35. Some of the conditions that are preferred include the following:
- Patients are motivated and able to commit to a healthy lifestyle after gastric sleeve surgery
- Being able to visit the doctor regularly after gastric sleeve surgery
- Lack of medical conditions that prevent the procedure from being performed
- If you have an issue that prevents you from having a sleeve gastrectomy or don’t want to undergo a surgical procedure that carries some risks, you can try a gastric balloon capsule that helps you lose weight without surgery.
Finally, the difference between pancreatic bypass and gastric sleeve lies in their mechanism of action and how each procedure influences nutrient absorption and contributes to the management of obesity-related diseases. While gastric sleeve offers a straightforward and effective approach to weight loss, pancreatic bypass is a more advanced technique designed for complex cases such as morbid obesity and type 2 diabetes.
If you’re considering a step toward a healthier life, Bimaristan Medical Center provides the latest bariatric surgery options, supported by a specialized medical team and individualized care for each patient, ensuring safe, effective, and lasting results.
Sources:
- Johns Hopkins Medicine. (n.d.). BPD/DS weight-loss surgery. Johns Hopkins Medicine
- NHS. (2024, February 5). What is weight-loss surgery? NHS
- American Society for Metabolic and Bariatric Surgery. (n.d.). Biliopancreatic diversion with duodenal switch

