Transanal total mesorectal excision (TaTME) is one of the latest surgical techniques for rectal cancer treatment, combining high precision with minimally invasive surgery, maximizing the chances of a quick recovery and minimizing complications. This method gives patients, especially those with lower rectal tumors, the opportunity to completely remove the tumor while preserving the surrounding nerves and bowel function.
Turkey has become a distinctive destination for this surgery, thanks to the expertise of specialized doctors, hospitals equipped with the latest technology, and the provision of integrated medical tourism services for Arab patients. In this article, we will explain everything you need to know about TaTME: From the appropriate categories, how the surgery is performed, its benefits and risks, and even the steps to recovery after the procedure.
What is transanal total mesorectal excision (TaTME)?
Transanal total mesorectal excision (taTME), also known as “bottom-up” surgery, is a minimally invasive robotic alternative to traditional surgery for patients with lower rectal cancer. The main advantage of this procedure is that it allows the surgeon to better visualize and remove the tumor in cases of lower rectal cancer, while avoiding a large incision in the skin. In the taTME procedure, the entire tumor is removed, while maintaining all the advantages of traditional laparoscopic surgery, including a shorter recovery period, less scarring, and less pain. Importantly, this procedure allows the surgeon to perform a precise resection without removing the anus, sparing patients the need for a permanent colostomy (pouch).
Surgery remains the gold standard for treating locally advanced rectal cancer. Total mesorectal excision (TME) is the most effective approach for reducing local tumor recurrence. However, achieving a complete TME can be challenging, especially in low rectal tumors and in anatomically difficult pelvises. TaTME was developed to facilitate dissection in the lower pelvis and potentially improve oncologic outcomes.
TaTME is a modern surgical technique for treating rectal tumors. It was developed to provide the shortest and most direct access to tumors in the lower rectum, allowing excellent visualization of the distal margin and enabling more precise excision. Introduced in 2010, TaTME differs from conventional laparoscopic or robotic approaches by offering a “bottom‑up” perspective, which helps surgeons operate more safely and accurately in patients with a narrow pelvis or low rectal tumors. Its use has since expanded to include complex non‑cancerous conditions such as inflammatory bowel disease, redo surgery after Hartmann’s procedure, and correction of anastomotic strictures.
Patients suitable for transanal total mesorectal excision (TaTME) surgery
- Low or intermediate rectal cancer
- Patients with tumors located in the lower part of the rectum, where traditional surgical access is difficult due to pelvic narrowing or the tumor’s proximity to the anus.
- Total transanal resection provides excellent visibility of the distal margin of the tumor, reducing the likelihood of cancer cells remaining.
- in cases where conventional proctectomy is difficult, such as
- patients with a deep or narrow pelvis
- Relatively obese patients, where dissection is difficult with conventional laparoscopy
- Patients who wish to preserve anal function and the surrounding muscles
- TaTME provides a greater opportunity to preserve the nerves and muscles surrounding the rectum, which helps maintain bowel, sexual, and bladder function.
- Cases requiring precise coloanal anastomosis
- Patients who require accurate coloanal anastomosis, especially when using single stapler technology.
- Complex non-cancerous conditions
- Chronic inflammatory bowel disease (IBD), such as Crohn’s disease and ulcerative colitis
- Anastomotic strictures
- Re-procedures after the Hartmann procedure
Why is transanal total proctectomy used to treat rectal cancer
- Accessing difficult tumors in a narrow pelvis: Some rectal tumors are located very low or in a narrow pelvis, making resection by traditional surgery or laparoscopy difficult. TaTME provides a direct bottom-up pathway, allowing the surgeon to clearly see the distal margin of the tumor and perform a precise resection.
- Improved quality of resection and purity of surgical margins: Studies have shown that TaTME helps achieve a high percentage of complete or near-complete rectal resection, with a lower likelihood of cancer cells remaining in the margin. This precision reduces the risk of local tumor recurrence and improves long-term patient outcomes.
- Preservation of anal function and surrounding nerves: Better visualization of neuromuscular structures during the procedure allows for preservation of bowel, bladder, and sexual function. This is critical for patients who wish to avoid the need for a permanent colostomy.
- Reduce the difficulties of traditional surgery: TaTME helps overcome the challenges of surgery in obese patients or in cases of very low tumors, where traditional instruments are limited in reach and mobility.
- Facilitate accurate colonic anastomosis: After tumor removal, the remaining colon can be connected to the anus in a precise and safe manner, with the possibility of using a single stapler technique to minimize the possibility of leakage.
- Scalability for non-cancerous conditions: TaTME can also be used to treat some complex non-cancerous conditions, such as inflammatory bowel disease, junctional stenosis, or re-Hartmann, demonstrating the technique’s flexibility and versatility.
Surgeons choose TaTME when there are low tumors in a narrow pelvis, or when they want to improve resection accuracy and preserve neuromuscular function.
Difference between transanal total proctectomy and laparoscopic surgery
| Criterion | Transanal total mesorectal excision (TaTME) | Laparoscopic or robotic surgery |
|---|---|---|
| Surgical path | Bottom-up, that is, starting the process through the anus | Direct visualization of surrounding muscles and nerves, better ability to maintain anal, bladder, and sexual function |
| Tumor Access | Ideal for low tumors in the narrow pelvis, direct view of the distal margin | Challenges in the deep pelvis, you may need to move multiple tools to achieve good visibility |
| Precision at the far margin | Excellent visualization of the distal margin of the rectum reduces the likelihood of cancer cells surviving | Depending on the surgeon’s skill and laparoscopic/robotic experience, the distal margin may be harder to reach |
| Maintaining nerves and muscles | Urethral injury, joint leakage, and temporary effect on anal function | Nerves can be preserved, but vision is less clear compared to TaTME in some cases |
| Possible complications | Urethral injury, joint leakage, temporary effect on anal function | Similar complications, but the biggest challenge is the reach and margin |
Preparation before total transanal rectal resection
Before undergoing transanal total mesorectal excision (TaTME) surgery, the patient undergoes thorough preparation to ensure the highest level of safety and precision. This begins with a complete medical evaluation, which includes a digital rectal examination, a CT scan of the chest and abdomen, as well as an MRI or endoscopic ultrasound to determine the exact extent of the tumor.
The bowel is then mechanically prepared to ensure that the surgical part is easy to perform through the rectum and to minimize any potential complications. The patient is also given prophylactic antibiotics according to the hospital’s usual protocol to minimize the risk of infection. Finally, the patient is given general anesthesia so that they are completely asleep and unable to feel any pain during the procedure.
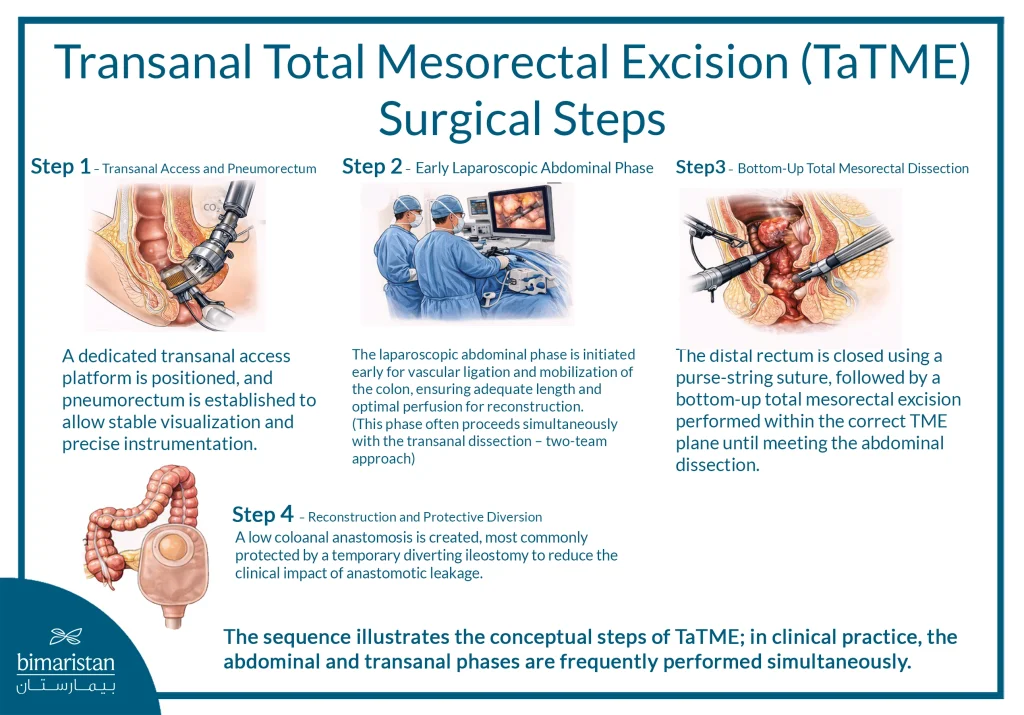
Transanal total mesorectal excision (TaTME) steps
After full preparation, the surgical team begins setting up in the operating room, where the patient is placed in the lithotomy position to facilitate surgical access from both pathways: Abdominal and transanal. Two specialized teams, one to work on the abdominal and the other on the anal pathway, are also prepared with laparoscopic equipment, making sure that all team members are fully aware of the steps of the operation and the possibilities of complications.
- The surgeon evaluates the abdomen using a laparoscope to check for any adhesions or possible spread of the disease. Next, the inferior mesenteric artery is ligated, and the entire left colon is freed to ensure there is enough length to complete the connection at the end.
- Transanal surgery, where a suitable laparoscopic platform is placed with the anal muscles stretched to provide a clear field of view. Next, a ring is sewn over the tumor to close the rectal cavity and prevent leakage of bowel content during resection. The surgeon then makes a full circular incision in the rectal wall around the tumor and carefully separates the tissue all the way to the abdominal cavity.
- Complete resection: The surgeon continues to carefully separate the rectum and surrounding tissue to ensure that the entire affected area is removed while maintaining a healthy margin, and in some cases, the specimen is removed through the rectum to minimize abdominal wall injuries.
- After the tumor is removed, the joining stage comes: The remaining colon is connected to the anus, either with hand sutures or staples. In many cases, a temporary shunt (Ileostomy) is created to protect the connection and prevent any possible leakage.
To minimize risks, the surgeon sometimes uses fluorescence angiography before and after the connection to make sure that blood has good access to both ends of the connection. Finally, instruments and scopes are removed, the operation site is inspected, and any incisions are closed, leaving drainage tubes if necessary to ensure a safe recovery.
Recovery after total transanal transanal rectal excision (TaTME)
After TaTME surgery is completed, the patient begins the recovery phase in the hospital, usually staying for two to five days under close observation to ensure the patient’s health is stable. On the first day, the patient starts with a liquid diet, then gradually switches to a regular diet depending on the tolerance of the digestive system. Walking and light movement are recommended from the day after surgery, as these steps help speed up recovery, improve blood circulation, and minimize the risk of complications.
Upon discharge from the hospital, the patient continues to monitor their health status and pain control as instructed by the physician. You may notice an increase in bowel movements for a short period, but this gradually improves.
Moderate daily activities, such as walking slowly and doing light tasks, can be gradually resumed. In the case of a temporary ileostomy, it is usually removed after 3 to 6 months, after making sure the joint has healed and completing any supportive treatment, such as chemotherapy or radiation if needed, to ensure the best results and full recovery.
Advantages of Transanal Total Rectal Excision
Transanal total proctectomy offers several key benefits over traditional methods:
- Better visibility to access tumors: The surgeon can see the distal margin of the rectum with greater precision.
- Achieve high quality in the resection specimen: Studies have shown 97.3% complete or near-complete rectal resection with very low rotational and distal margins.
- Minimize surgery time: Using two synchronized teams reduces operation time by up to 60 minutes.
- Single stapler techniques can be used: This reduces the need for duplicate staples and decreases the likelihood of leakage in some studies.
- Protection of neuromuscular function: Bladder, sexual, and bowel function can be preserved when the technique is mastered.
- Multiple applications: They can be used for non-cancerous conditions such as Hartmann’s reattachment, joint stenosis, and inflammatory bowel disease.

Complications of total transanal rectal resection
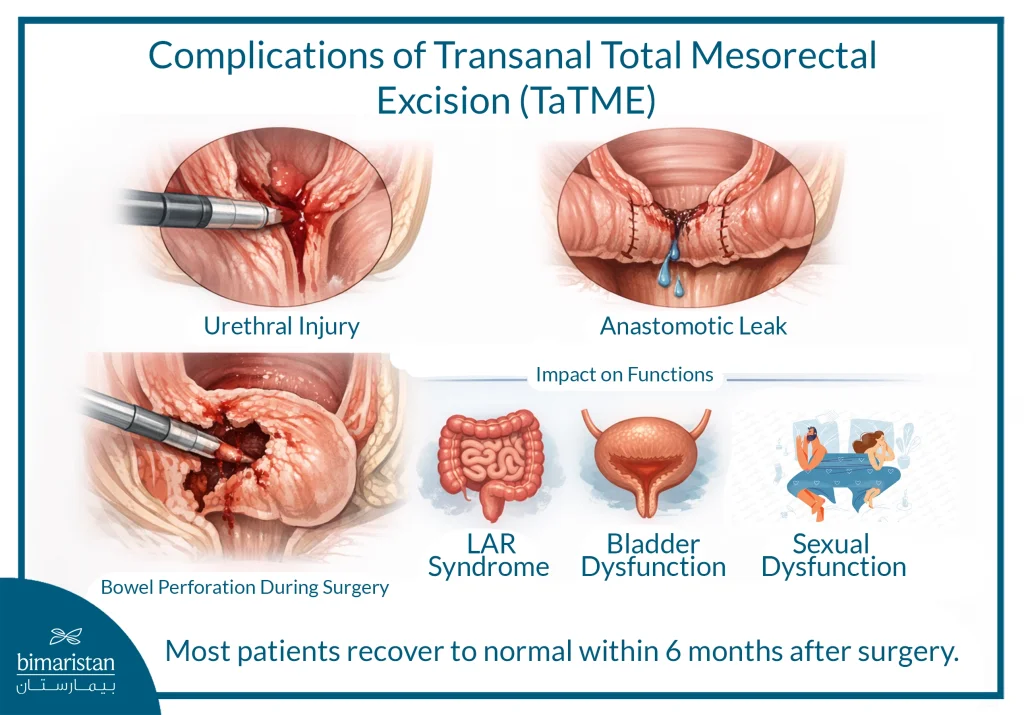
Despite the benefits, transanal total proctectomy carries potential complications due to the change in surgical perspective and the use of new pathways:
- Urethral injury: Especially in males during the first stage of transanal proctectomy, with a rate of about 1.9% according to international studies, often occurring in the first cases of the surgical team.
- Connection leakage: Although the use of mono-conduction may reduce the likelihood, data is inconsistent between studies, and patient selection and appropriate surgical technique remain important factors.
- Other rare complications: These include air bubbles in the intestinal tract (pneumatosis), intestinal perforation during the procedure, and even one case of air embolism.
- Impact on function: There may be a temporary impact on bowel function (LAR syndrome), bladder, and sexual function, but most patients return to normal within 6 months after the procedure.
Total Transanal Proctocolectomy (TaTME) Cost in Turkey
The cost of transanal total mesorectal excision (TaTME) in Turkey varies depending on several factors, including the chosen hospital, the experience of the surgeon, the type of technique used, whether laparoscopic or robotic, and the length of the patient’s stay.
In general, the estimated cost ranges between $8,000 and $18,000 USD, which usually includes hospital and surgery fees, anesthesia, pre- and post-operative care, hospital stay, and sometimes some basic lab tests. Compared to European countries or the United States, where the cost may exceed 20,000 to 35,000 USD, Turkey is an economical and attractive option for patients seeking advanced treatment at affordable prices without compromising on the quality of medical care.
Why do patients choose Turkey for transanal total proctectomy?
- High-quality specialized centers: Turkey has advanced hospitals equipped with the latest laparoscopic and robotic technology, with specialized surgery teams for rectal cancer.
- Experience of surgeons: TaTME-trained surgeons with extensive experience in transanal surgery, with a reliance on proctoring and structured training programs.
- Modern technologies at affordable prices: Compared to European or American countries, Turkey provides the same level of medical care at a significantly lower cost.
- Easy travel and accommodation: Turkey is geographically close to many Arab patients, with full medical tourism services including accommodation, transportation, and translation.
- Successful operations and good results: Post-operative recovery and function rates in advanced Turkish centers are comparable or better than some European countries, especially in carefully selected patients.
Transanal total mesorectal excision (TaTME) surgery is a true revolution in the treatment of rectal cancer, providing a precise view of the distal margin, preserving anal function and surrounding nerves, and facilitating precise colonic connections. This technique is an ideal option for patients with low rectal tumors or anatomical challenges such as a narrow pelvis, and is also applied in some non-cancerous conditions, such as inflammatory bowel disease and Hartmann recurrence.
Turkey has become a leading destination for this type of surgery, due to the presence of advanced hospitals, expert surgeons, and affordable costs compared to European or American countries, taking into account the quality of medical care and the success of the results. Among these distinguished centers, Bimaristan Medical Center stands out as one of Turkey’s leading centers for TaTME, with a specialized surgical team and structured training programs to ensure the highest levels of safety and optimal results for patients.
Sources:
- Trépanier JS, Lacy FB, Lacy AM. Transanal Total Mesorectal Excision: Description of the Technique. Clin Colon Rectal Surg. 2020 May;33(3):144-149
- Ng JY, Chen CC. Transanal total mesorectal excision for rectal cancer: it’s come a long way and here to stay. Ann Coloproctol. 2022 Aug;38(4):283-289
- Cassinotti, E., Palazzini, G., Della Porta, M., Grosso, I., & Boni, L. (2017). Transanal total mesorectal excision (TaTME): Tips and tricks of a new surgical technique. Annals of Laparoscopic and Endoscopic
- Scott N, Jackson P, al-Jaberi T, Dixon MF, Quirke P, Finan PJ. Total mesorectal excision and local recurrence: a study of tumor spread in the mesorectum distal to rectal cancer. Br J Surg. 1995 Aug;82(8):1031-3
- Stefanou, C. K., et al. (2024). Transanal total mesorectal excision: Understanding indications, managing complications, and effective prevention methods. Journal of Surgical Oncology and Practice