Lumbar stabilization surgery is a common surgical procedure used to treat issues that affect the stability of the spine in the lumbar region, in this procedure, advanced techniques are used to ensure the stabilization of the affected vertebrae, which contributes to reducing pain and improving the patient’s ability to move, this surgery is resorted to in certain cases when other treatments such as medication or physical therapy have failed.
Thanks to medical advances in this field, it has become possible to obtain effective results while minimizing the risks associated with the procedure; however, the choice to perform this procedure depends on the diagnosis of the condition and the patient’s response to conventional treatment.
What is lumbar stabilization surgery?
Lumbar stabilization surgery is a surgical procedure used to treat spinal issues in the lower back (lumbar region), which may include herniated discs, fractures, or degenerative diseases such as arthritis. The procedure aims to restore stability to damaged vertebrae by fusing them together using metal instruments such as pins and rods. The primary goal of lumbar stabilization surgery is to relieve pain caused by the spinal disorder and improve spinal function, helping to restore normal mobility.
This surgery is resorted to when non-surgical treatments such as medications and physical therapy do not bring relief to the patient. Surgeons use advanced techniques, such as minimally invasive surgery, to minimize complications and speed up the healing process, and it is an effective option in cases where spinal issues are interfering with the patient’s daily life. Although it significantly improves health, it may require constant monitoring after surgery to make sure there are no complications.
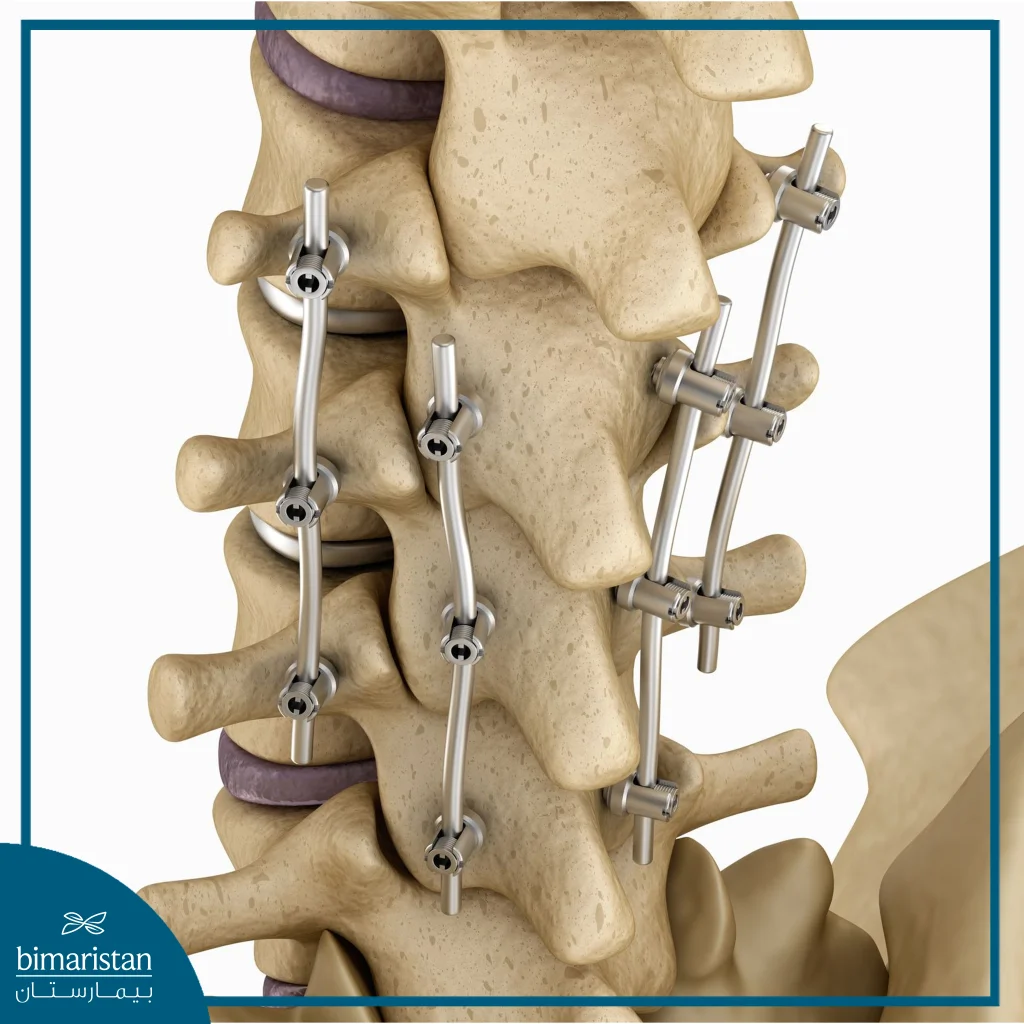
Indications for lumbar stabilization surgery
Lumbar stabilization surgery is performed when the vertebrae in the lower back experience issues that affect spinal stability and mobility, with the goal of restoring stability, relieving pain, and improving spinal function in cases that do not respond to conservative treatments:
- Herniated disc: Occurs when the disc protrudes between the vertebrae and presses on the nerves, causing severe pain, numbness, and weakness in the lower limbs, and requires stabilization.
- Joint degeneration (arthritis): Damage to the cartilage between the vertebrae causes chronic pain and difficulty in movement, and stabilization can help improve spinal function and relieve symptoms.
- Bone infections: Such as inflammation of the spine caused by infection, where the damage leads to loss of stability, stabilization is necessary to maintain the integrity of the spine.
- Fractures of the spine: Including fractures resulting from accidents or osteoporosis, stabilization is needed to ensure the vertebrae heal properly and prevent deformities.
- Bone tumors: Some tumors cause destruction of the surrounding bone, and stabilization is the way to maintain stability and prevent complications.
- Congenital deformities: Such as congenital scoliosis, surgery helps to correct the deformity and improve the function of the spine.
- Failure of conservative treatments: Cases that have not improved with medication or physical therapy require spinal stabilization to relieve pain and improve mobility.
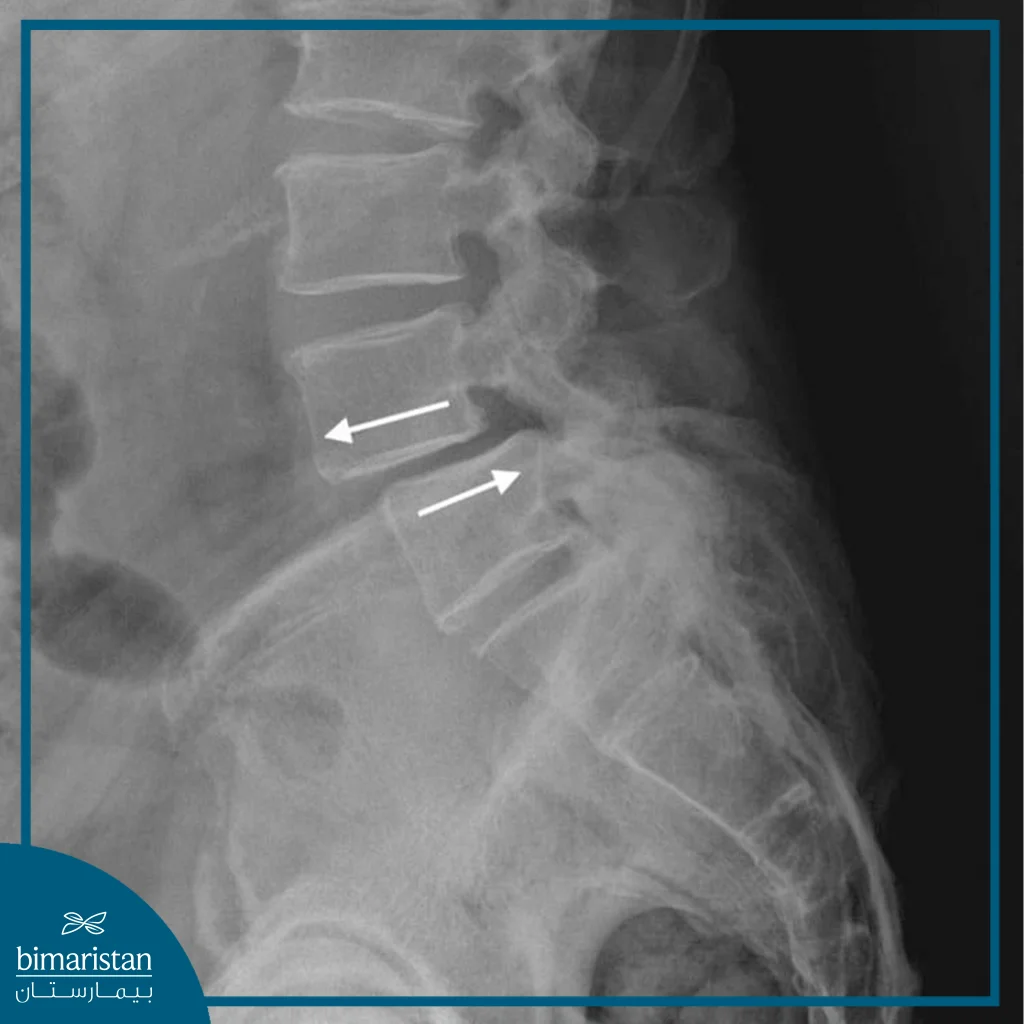
Lumbar stabilization surgery steps
Lumbar stabilization surgery begins with careful preparation to ensure the patient’s readiness to undergo surgery and avoid complications, including assessing the general health status, laboratory tests, and radiography to determine the exact location of the stabilization. After that, the surgical team proceeds to apply step-by-step procedures to ensure complete stabilization of the vertebrae and achieve the best therapeutic results. The most important steps include:
- General anesthesia and surgical preparation: The patient is placed under general anesthesia to ensure no pain, and the patient is positioned on the surgical table in a way that gives the surgeon optimal access to the targeted vertebrae, taking into account the protection of surrounding nerves and organs.
- Making a proper incision: The surgeon makes an incision through the skin and soft tissue to the targeted vertebrae, taking care to minimize damage to the surrounding muscles and minimize blood loss.
- Preparing the vertebrae for fusion: The vertebral space is cleared of damaged tissue or a damaged disk, and the bone surface is prepared to receive bone fusion materials or bone grafts that help the vertebrae heal together in a stable manner.
- Installing the metal pins and rods: The surgeon attaches the metal pins to the targeted vertebrae and then attaches them to the rods to ensure spinal stability, making sure the vertebrae are properly aligned to prevent any future deformity.
- Adding bone grafts or fusion-inducing materials: Bone grafts or fusion-inducing materials are placed between the vertebrae to ensure they are firmly and permanently fused, which helps reduce unwanted movement and increases the stability of the spine.
- Check for stability and alignment: The surgeon uses imaging during the procedure to make sure that the screws and rods are in place and the vertebrae are perfectly aligned to avoid any later complications.
- Incision closure and final sterilization: After confirming the success of the fixation, the incision is closed layer by layer with drainage tubes if necessary, the area is cleaned and sterilized, and the patient begins the recovery phase under close supervision.
Follow-up after surgery
After completing the lumbar stabilization surgery, the patient begins the recovery phase under the supervision of the medical team to ensure that the vertebrae heal and normal spinal function is restored. During the first few days, the patient’s vital signs, such as blood pressure, pulse rate, and temperature, are monitored to ensure there are no acute complications.
The patient is given painkillers and anti-inflammatory medications on a regular basis to reduce pain and swelling, and is encouraged to move lightly under the supervision of specialists to avoid blood clots and improve blood circulation. The patient is also advised to wear a special back brace to support the stabilized vertebrae and reduce pressure on them during movement.
In the following weeks, radiographs are taken to ensure that the screws and rods are stable and the vertebrae are properly aligned, and a physical therapy program is prescribed to strengthen the muscles surrounding the spine and improve flexibility. Regular follow-up is essential to ensure the success of the procedure and minimize any potential complications. It also helps to assess the patient’s progress and adjust the treatment program as needed to ensure the best possible outcome and return to normal daily activity.
Success rates
Lumbar stabilization surgery has high success rates when the right patients are selected and performed under the supervision of a specialized surgical team. Medical studies indicate that the success rate usually ranges between 85% and 95% in stabilizing the spine and significantly reducing pain. The success of the operation depends on several factors, such as age, general health status, the degree of damage to the vertebrae, and the patient’s commitment to the recovery plan after the operation.
Patients who follow a physical therapy program and adhere to the doctor’s instructions after the procedure usually have better results after lumbar stabilization surgery, including improved daily mobility and reduced risk of future complications. Ongoing follow-up scans and examinations show that the stabilized vertebrae are healing well, allowing the patient to return to their daily activities with confidence and stability. This procedure is an effective option to improve the quality of life for patients with spinal disorders.
Advantages of lumbar stabilization surgery
Lumbar stabilization surgery offers significant benefits to patients with unstable spinal disorders or chronic pain. The procedure helps restore stability in the lower back and improves mobility, significantly enhancing quality of life. It also minimizes future complications associated with curvatures or deformities of the vertebrae, among other benefits:
- Significant pain relief: The procedure decompresses the nerves and reduces abnormal movement of the vertebrae, resulting in a decrease in chronic pain in the lower back and lower extremities.
- Restores stability to the spine: Stabilizing the vertebrae with metal pins and rods restores spinal stability and prevents slippage or abnormal movement of the vertebrae.
- Improved mobility: After the vertebrae have healed, the patient feels a significant improvement in the ability to walk, bend, and engage in daily activities without pain.
- Prevent deterioration of the condition and the development of deformities: The procedure prevents the worsening of curvatures or slipped vertebrae, minimizing the need for future surgical interventions.
- Improved sleep quality and rest: Relieving persistent pain contributes to better sleep and less stress and fatigue caused by chronic pain.
- Enhance muscle strength and peripheral support: In conjunction with physical therapy programs, the procedure helps strengthen the muscles surrounding the spine and improves balance and support.
- Long-term and stable results: When the procedure is successful and follow-up is adhered to, spinal stabilization and improved physical functioning can last for many years, allowing the patient to return to a normal, stable life.
Possible complications of lumbar stabilization surgery
Despite the significant benefits of lumbar stabilization surgery, there are some potential complications that patients should anticipate and discuss with their medical team prior to the procedure. These complications include issues related to the surgery itself or recovery, and their severity may vary from patient to patient, depending on health status and the type of damage to the spine:
- Infection at the surgical site: Postoperative infection can occur in the skin, deep tissues, or bone and may require antibacterial therapy or additional surgical intervention.
- Excessive bleeding during or after surgery: Blood loss can be severe in some cases, sometimes requiring a blood transfusion or additional procedures to control bleeding.
- Bone Fusion Failure: In some cases, the vertebrae may not heal completely, leading to abnormal movement between the vertebrae and requiring re-surgery.
- Nerve damage or numbness: The nerves surrounding the vertebrae can be compressed or damaged during surgery, causing numbness or weakness in the lower limbs.
- Persistent pain or recurrence of pain: Despite the success of the procedure, some patients may experience mild to moderate pain due to other issues in the spine or surrounding muscles.
- Moving or breaking metal devices: Metal pins or rods may move or break, necessitating a doctor’s review and possibly re-intervention.
- Problems with wound healing or abnormal scarring: Some patients may experience delayed skin healing or significant scarring, requiring careful medical follow-up to ensure proper healing.
Advantages of treatment in Turkey
Treatment in Turkey is a preferred option for many patients requiring lumbar stabilization surgery, owing to the country’s high standard of medical care, modern equipment, and specialized surgical staff. Turkish hospitals are also characterized by providing integrated services that include consultations, examinations, surgery, and post-operative follow-up, which ensures a smooth and safe medical experience:
- Affordable cost compared to other countries: Turkey offers competitive prices for surgical treatments without compromising the quality of care, making the process more affordable for international patients.
- Highly specialized surgeons: Our surgeons have extensive experience performing lumbar stabilization surgery using the latest techniques, maximizing the success of the procedure and minimizing risks.
- Modern hospitals and equipment: Turkish hospitals rely on advanced medical equipment and accurate imaging systems that contribute to accurate surgical planning and perfect results.
- Comprehensive post-operative follow-up services: Follow-up programs include physical therapy and regular check-ups to ensure that the vertebrae heal and normal spinal function is restored.
- Easy travel and accommodation for international patients: Hospitals provide dedicated services for international patients, including transportation, accommodation, and translation, making it easier for patients to access and follow-up treatment without complications.
- Focus on patient experience and quality of life: Turkish hospitals provide a supportive environment for patients with personalized care, reducing anxiety and increasing patient comfort during treatment and recovery.
- Ability to integrate modern treatments: Surgery, physical therapy, and other modern techniques can be combined in Turkey to ensure the best possible results and minimize potential complications.
Medical development in Turkey has made lumbar stabilization surgery a procedure characterized by accuracy and safety, with high success rates and remarkable patient satisfaction, as the combination of surgical expertise, modern techniques, and integrated care before and after the operation contributed to enhancing patients’ confidence in Turkish medical services.
The well-equipped treatment environment and humane follow-up care made the treatment experience more comfortable and reassuring, making Turkey an advanced medical destination that combines efficiency and affordability, making it a preferred choice for patients looking for high-quality spine surgery.
Sources:
- Aghayev, K., Mayers, A., Coppa, C. P., Cammisa, F. P., Girardi, F. P., & Lebl, D. R. (2023). Lumbar spinal fusion and fixation: Overview and current concepts. EFORT Open Reviews, 8(11), 1069-1081.
- Al Barbarawi, M. M., Audat, Z. M., & Allouh, M. Z. (2015). Analytical comparison study of the clinical and radiological outcome of spine fixation using posterolateral, posterior lumbar interbody and transforaminal lumbar interbody spinal fixation techniques to treat lumbar spine degenerative disc disease. Scoliosis, 10, Article 40.
- Liang, Q., Wang, Q., Sun, G., Ma, W., Shi, J., Jin, W., Shi, S., & Wang, Z. (2018). Five-year outcomes of posterior affected-vertebrae fixation in lumbar tuberculosis patients. Journal of Orthopaedic Surgery and Research, 13(1), 210.



