Microsurgical varicocelectomy is one of the most advanced surgical options for treating varicocele and is performed in many fertility centers worldwide. Studies show that varicocele affects about 15–20% of adult men and contributes to nearly 35% of male infertility cases. Microsurgical varicocelectomy has demonstrated significant improvement in semen parameters with very low complication rates. The technique aims to create an optimal environment for the testicle by precisely ligating dilated veins while preserving the artery and lymphatic channels.
What is a varicocele?
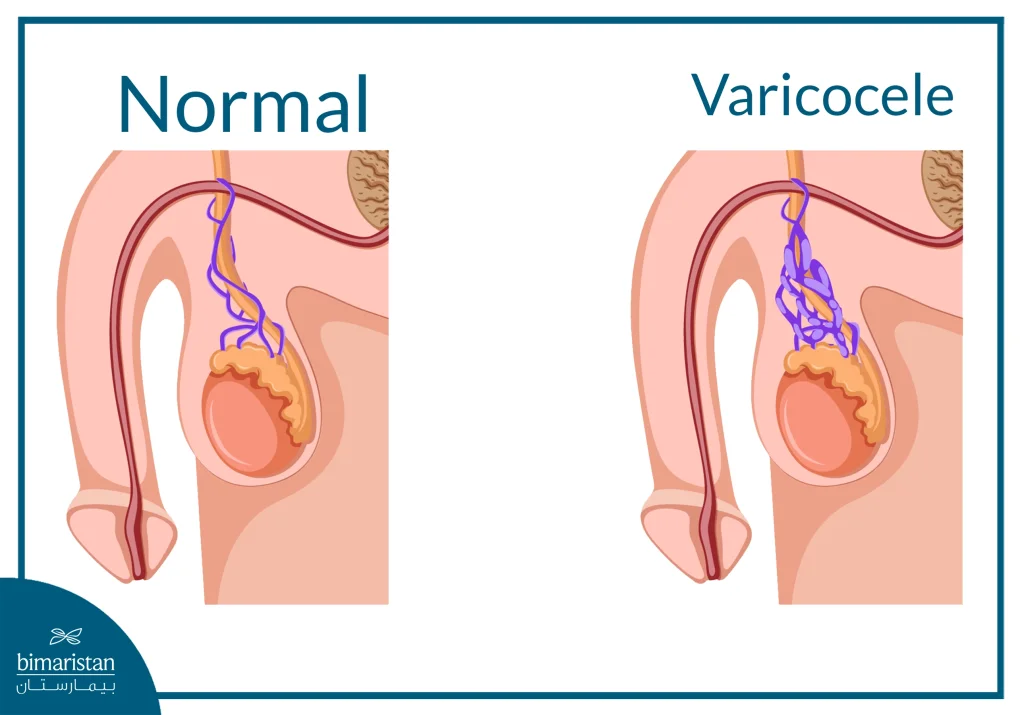
Varicocele is an abnormal enlargement of the veins surrounding the spermatic cord within the scrotum, caused by malfunctioning venous valves responsible for returning blood from the testicle to the body. Failure of these valves leads to venous stasis and elevated venous pressure, causing vein dilation and varicose veins.
Varicocele is one of the most common causes of male infertility. It can affect sperm count, quality, and motility, leading to sperm dysfunction, and may be associated with pain or heaviness in the testicle that increases with standing or exertion. The disorder is diagnosed clinically and by ultrasound and is treated when it causes symptoms or affects fertility, using procedures that close the affected veins and divert blood to healthy veins.
Indications for microsurgical varicocelectomy
Microsurgical varicocelectomy is indicated in the following cases:
- Large varicose veins accompanied by pain or heaviness in the scrotum
- Chronic testicular pain associated with varicose veins that has not responded to conservative treatment
- Men who have clinically or ultrasound-observed varicose veins
- A child or adolescent with a noticeable difference in testicular size or the potential for atrophy development
- Men with secondary infertility or low sperm count and quality
Relative and absolute contraindications to microsurgical varicocelectomy
- Absolute contraindications: Severe allergy to general anesthesia if it is required and cannot be replaced, or medical conditions that prevent any surgical intervention.
- Relative contraindications: Having another cause of infertility that can be corrected without surgery, or expecting a limited effect of the procedure if female infertility is the main factor.
Therapeutic goals of microsurgical varicocelectomy
This procedure is performed with the aim of:
- Closing dilated varicose veins and re-establishing a favorable thermal and functional environment for the testicle
- Maintain the testicular artery and lymphatic drainage systems to restore proper perfusion and avoid hydrocele
Preparation before microsurgical varicocelectomy
Thorough preparation for the procedure helps achieve the best results and significantly reduces complications. This includes:
- A thorough clinical examination to clinically confirm and categorize the presence of varicose veins
- Semen analysis at least two times at an appropriate interval
- Discussing the risks, benefits, and alternatives; record written informed consent
- Stopping anticoagulant medications should be done according to protocol and in coordination with your physician
- Providing preoperative instructions for the patient, including fasting requirements based on the type of anesthesia and infection precautions
- Ultrasound imaging when needed to confirm the diagnosis or to evaluate the anatomy before surgery
Microsurgical varicocelectomy steps
Microsurgical varicocelectomy requires great precision and full adherence to the following steps:
- Anesthesia: General anesthesia or local anesthesia with epidural anesthesia according to the risk assessment and preference of the medical team.
- Patient position: Lying down with the testicles supported and the surgical area disinfected and sterilized.
- Skin incision: A small skin incision approximately 2-3 centimeters long is made at the top of the scrotum.
- Stripping and accessing the spermatic cord: Exposing the spermatic cord and isolating the cord within the sheath.
- Microscope placement: The operating microscope is positioned to provide high‑magnification visualization, enabling precise identification of microanatomical structures.
- Identification of the testicular artery and lymphatics: The testicular artery is identified using pulsation, Doppler assistance, or vascular dye. Lymphatic channels are preserved to prevent postoperative hydrocele formation.
- Identification of dilated veins: All dilated veins are meticulously dissected free from surrounding tissues under magnification.
- Isolation and ligation: Each pathological vein is individually isolated and ligated using fine microsutures or microclips. Thermocoagulation may be used when appropriate, although microsuture ligation remains the standard technique.
- Ensure there is no bleeding: Hemostasis is confirmed while preserving the integrity of the testicular artery and lymphatic vessels.
- Closing the seams: Repositioning the spermatic cord and closing the layers of subcutaneous tissue and skin with cosmetic sutures.
- Coverage: A sterile bandage is applied, followed by postoperative care instructions tailored to the patient’s recovery.
Studies indicate that the success rate of microsurgical varicocelectomy is significantly high, as it achieves a significant improvement in sperm count and motility in about 70-80% of cases, with pregnancy rates ranging from 30-50% within 6-12 months after the procedure.
Possible complications after microsurgical varicocelectomy and how to manage them
The patient may experience some complications after undergoing microsurgical varicocelectomy, such as:
- Varicose recurrence: Needs re-treatment.
- Inflammation or postoperative infection: Managed with appropriate antibiotic therapy; surgical intervention and repair are considered if necessary.
- Chronic pain: Painkillers are administered for a short period; if symptoms persist, other causes are evaluated.
- Hydrocele: Rare with preserved lymphatic ducts; if it occurs, it may need drainage or subsequent surgery.
Microsurgical varicocelectomy surgery cost in Turkey
Bimaristan Medical Center in Turkey provides the highest standards of care and quality in performing microsurgical varicocelectomy, while offering competitive costs compared with European countries, thereby ensuring a comfortable and effective treatment experience without sacrificing quality. A table showing the prices of microscopic varicocele surgery in Turkey compared to European countries:
| Country/Center | Average cost in U.S. dollars | Notes |
|---|---|---|
| Turkey | 2,000 – 2,500 | Pre-operative check-ups, accommodation, and post-operative follow-up |
| Germany | 5,500 – 7,000 | High cost due to private hospitals and long-stay expenses |
| France | 6,000 – 7,500 | Surgery only, often not including accommodation or post-operative care |
| Switzerland | 7,000 – 9,000 | One of the most expensive in Europe, with excellent quality but very high cost |
| Netherlands | 5,000 – 6,500 | High quality, sometimes longer waits for appointments, and additional costs for post-operative care |
By performing microsurgical varicocelectomy within a precise clinical protocol, significant improvements in semen parameters and overall chances of conception can be achieved for couples. The procedure is carried out in specialized centers equipped with advanced technology and experienced surgical teams. Bimarestan Medical Center is proud to be one of the leading institutions in Turkey offering this treatment as part of a comprehensive medical‑tourism and postoperative‑care program, ensuring patients experience a comfortable and effective treatment journey.
Sources:
- Tatem, A. J., Goldstein, M., & Schlegel, P. N. (2017). The role of microsurgical varicocelectomy in treating male infertility. PMC
- Phan, H. T., et al. (2021). Efficacy of scroto-inguinal microsurgical varicocelectomy in infertile men. Arab Journal of Urology
- Liu, J. et al. (2025). “Microsurgical Varicocelectomy and Revascularization: A Novel Approach to Varicocele Treatment.” ScienceDirect
- Elbardisi, H., et al. (2017). Does the number of veins ligated during microsurgical varicocelectomy affect outcome? Translational Andrology and Urology
- Seo, J. T., Kim, K. T., & Moon, M.H. (2010). “The significance of microsurgical varicocelectomy in the treatment of subclinical varicocele.” Fertility and Sterility, 93(6), 1907-1910