Stereotactic radiotherapy is a modern medical technique that aims to treat tumors with high precision, delivering concentrated radiation directly to the tumor while preserving the surrounding healthy tissue. This technique represents a major advancement in managing small and delicate tumors, especially in the brain, lung, and liver, as it offers high effectiveness with fewer side effects compared to conventional radiotherapy.
What is stereotactic radiotherapy?
Stereotactic body radiotherapy is a cancer treatment that uses 3D or 4D imaging and precisely focused beams of radiation to deliver high doses to the target area while minimizing damage to surrounding healthy tissue. As with other forms of radiotherapy, stereotactic radiotherapy works by damaging DNA in tumor cells. Radiation-induced damage prevents cells from forming additional tumor cells. This causes tumors to shrink.
Unlike conventional radiotherapy, stereotactic radiotherapy delivers the optimal radiation dose over a shorter period (days rather than weeks). High doses of radiation are delivered to the tumor while minimizing exposure to surrounding healthy tissues and organs to avoid damage.
Types of cancers treated by stereotactic radiotherapy
Stereotactic radiotherapy is used to treat tumors, which are growing cells. Stereotactic radiotherapy is also used to treat cancerous tumors and non-cancerous tumors called benign tumors. Stereotactic radiotherapy is a non-invasive alternative to surgery. It is used to treat tumors and conditions located within the skull, brain, and skull base, including:
- Brain metastases
- Acoustic tumor
- Skull base tumors
- Trigeminal neuralgia
- Arteriovenous malformations
- Types of cancers for which stereotactic radiotherapy is used include:
- Lung cancer
- Head and neck cancer
- Abdomen (liver, pancreas, and adrenal gland cancers)
- Pelvic cancer
- Bone cancer
- Prostate cancer
- Spine cancer
Types of stereotactic radiotherapy
Types of stereotactic radiotherapy include:
- Linear Accelerator (LINAC): A robotic arm that rotates around the patient while lying on the table, directing X-rays to the tumor from different angles, allowing the dose to be delivered precisely to the targeted area while minimizing the impact on healthy tissue.
- Proton radiation: This newer type of stereotactic radiotherapy uses protons to treat tumors in multiple sessions. Proton beam therapy can be used to treat tumors in parts of the body that have already undergone radiotherapy. It can also treat tumors located near vital organs.
How does stereotactic radiotherapy work?
Stereotactic radiotherapy targets small tumors with high precision using concentrated doses of radiation. This technique is accurate to within 1 mm, does not require surgery, and can be performed on an outpatient basis. The radiation can be delivered using a frameless system or a conventional framed system. The beams are directed at the tumor to conform to its shape, allowing cancer cells to be destroyed while sparing the surrounding healthy tissue.
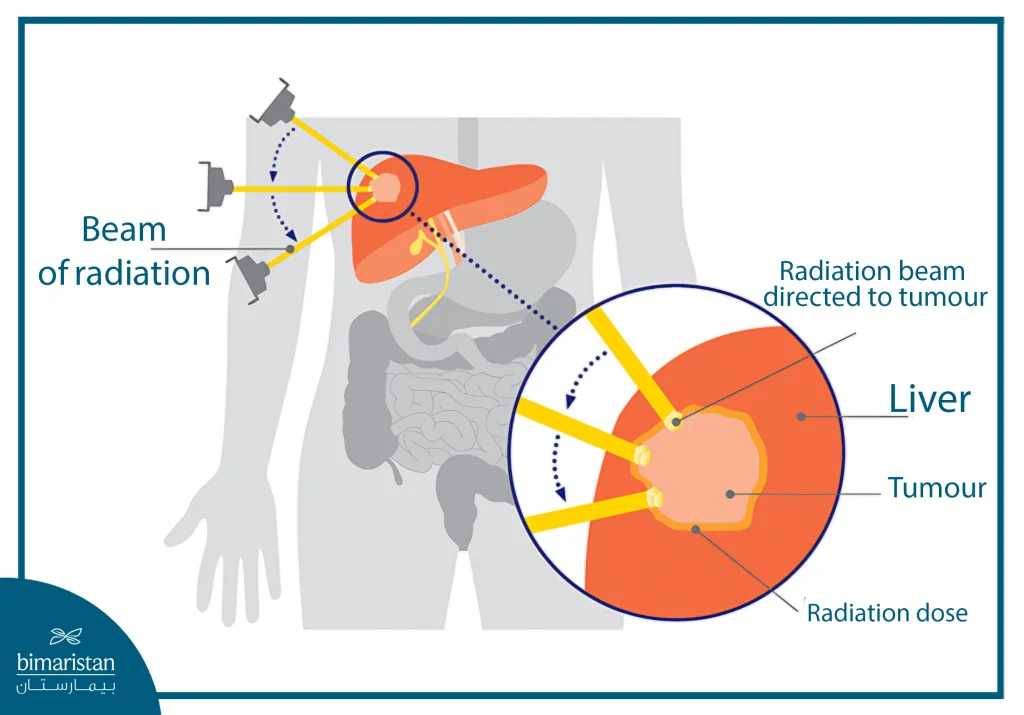
Preparation before stereotactic radiotherapy
Preparation before stereotactic radiotherapy is done in the following steps:
- Medical evaluation: Your doctor will review your medical history and perform tests and X-rays (such as a CT scan or MRI) to determine the exact location of the tumor.
- Simulation session:
- Three-dimensional or four-dimensional imaging devices are used to determine the tumor’s size, shape, and motion during breathing
- The patient is asked to lie on a specialized table in the same position they will hold during treatment
- Restraining devices, such as masks or vacuum cushions, are used to ensure that the patient remains still
- Placing directional signs:
- Tiny tattoos may be drawn on the skin to mark the position of the radiation in each session precisely
- In some cases, small metal tags are implanted inside the tumor to help machines track the movement of the tumor
- Computerized treatment planning: The treatment team uses the images obtained to design an accurate 3D plan that determines the optimal radiation angles, directions, and dose to target only the tumor while minimizing damage to healthy tissue.
Stereotactic radiotherapy steps
During a stereotactic radiotherapy session, the following procedures take place:
- Preparing for the session: The patient lies on the table, as in the simulation session, and the position is stabilized with specialized devices.
- Carrying out treatment: The Linear Accelerator or CyberKnife system rotates around the patient at multiple angles, directing multiple precise beams of high-energy radiation toward the tumor to intersect at the target point with pinpoint accuracy, destroying cancer cells without damaging surrounding healthy tissue.
- Monitoring during the session: The medical team is in a separate room to control the device and monitor the progress of the procedure, with the option of continuous voice communication with the patient through the loudspeaker. The session is painless, but some sounds may be heard from the device during operation; these are normal and do not cause discomfort.
- Duration of the session: A session typically lasts 30-60 minutes, depending on the tumor type and location. The number of sessions varies with the treatment plan, typically ranging from one to five, completed over one to two weeks.
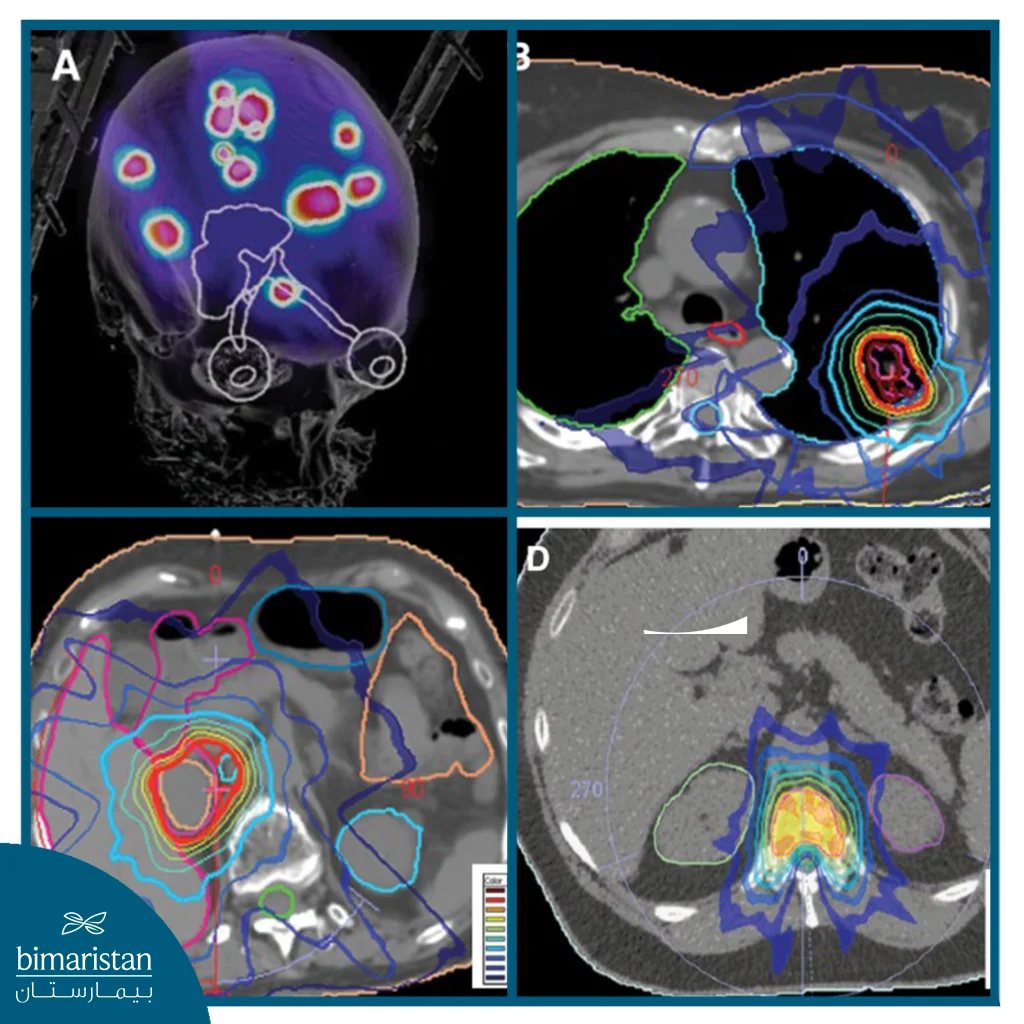
After stereotactic radiotherapy
The treatment does not require an overnight hospital stay, and the patient can go home immediately after the session. The patient may experience fatigue or mild swelling in the treatment area, which are transient effects that typically resolve within a few days after the procedure.
Benefits of stereotactic radiotherapy
Stereotactic radiotherapy has many benefits, including:
- Non-surgical alternative to surgery for some conditions
- High accuracy in targeting the tumor while protecting healthy tissue
- Reduces the number of treatment sessions compared to conventional radiotherapy
Side effects and risks of stereotactic radiotherapy
Side effects depend on the type of cancer and the patient’s general condition, and vary from person to person. For example:
- Lung cancer: The patient may experience generalized fatigue, a mild cough, or sputum production.
- Prostate cancer: The patient may notice a frequent need to urinate, changes in bowel function, or discomfort during bowel movements.
- Liver and pancreatic cancer: Nausea or diarrhea may occur, and your doctor may recommend medications to relieve these symptoms and minimize their impact on daily life.
Most of these effects are temporary and gradually improve after treatment sessions. The medical team monitors the patient and provides guidance to alleviate bothersome symptoms.
Delayed side effects
Rarely, side effects may appear in some people months or even years after treatment. They may include:
- Swelling of the arms or legs, also known as lymphedema
- Weakness in bones that can lead to fractures
- Changes in the bowel or bladder
- Changes in the spinal cord
- Changes in the lungs
- New cancer emerges
Potential risks of stereotactic radiotherapy
Despite the accuracy of stereotactic radiotherapy, there are some rare risks to consider:
- Some of the healthy tissue surrounding the tumor may be damaged, and there may be long-term effects depending on the organ being treated
- Very little chance of developing new cancers as a result of radiation exposure, which is very rare with modern techniques that focus on the tumor with high precision
These limited risks help weigh the benefits against the harms, and it is always best to follow the patient periodically after treatment to ensure the tumor is responding and to address any potential side effects promptly.
Comparison of stereotactic radiotherapy and conventional radiotherapy
The following table shows the difference between stereotactic radiotherapy and conventional radiotherapy:
| Comparison | Stereotactic radiotherapy | Conventional radiotherapy |
|---|---|---|
| Accuracy | very high (millimeter), precisely targeting the tumor without harming healthy tissue | Relatively less precise, the surrounding healthy tissue may be affected |
| Number of sessions | 1 – 5 sessions only | sessions over 25-40 weeks |
| Duration of the session | Relatively longer (30-90 minutes) | Shorter (10-20 minutes per session) |
| Side effects | Minor and temporary (fatigue, mild nausea, localized redness) | More common (fatigue, skin irritation, digestive or urinary disorders) |
| Effectiveness | Local tumor control up to 90% in some cases | Good effectiveness, but less precise and targeted |
| The type of tumors that are suitable | Small or well-defined tumors (brain, lung, liver, spine) | Larger or metastatic tumors require wider coverage |
| Risks | Very rare, slight possibility of harm to healthy tissue | Higher likelihood of surrounding tissues being affected by radiation |
Recovery period after stereotactic radiotherapy
The recovery period after stereotactic radiotherapy is generally short compared with conventional treatments, as it is non‑invasive and does not require extended healing time. Most patients can resume their daily activities within a day or two after the session, experiencing only mild fatigue or temporary localized swelling that gradually improves.
It is recommended to adhere to the regular follow-up schedule with the specialist to perform necessary imaging tests, evaluate the tumor’s response to treatment, and detect potential side effects early. Maintaining a healthy lifestyle that includes balanced nutrition and adequate rest is also beneficial for supporting full recovery and enhancing treatment effectiveness.
Stereotactic radiotherapy is one of the most advanced and precise techniques in cancer treatment, enabling highly accurate targeting of the tumor while reducing damage to surrounding healthy tissue. This approach is known for its high efficacy, fewer treatment sessions, and lower complication rates than conventional radiotherapy, making it a suitable option for many patients.
It is essential to consult a specialist to evaluate the case and determine whether stereotactic radiotherapy is the most appropriate treatment option, as the treatment plan depends on the tumor type, location, and the patient’s overall condition. Selecting a specialized medical center with an experienced team helps ensure the best treatment outcomes with the lowest possible risk of complications.
Sources:
- U.S. National Cancer Institute. (n.d.). Definition of stereotactic radiation therapy. In NCI Dictionary of Cancer Terms.
- MedlinePlus. (n.d.). Stereotactic radiosurgery – CyberKnife.
- Centers for Medicare & Medicaid Services (2020, April 1). Local Coverage Determination (LCD): Stereotactic Radiation Therapy: Stereotactic Radiosurgery (SRS) and Stereotactic Body Radiation Therapy (SBRT) (L35076).
- Hall, W. A., & Das, J. M. (2025, July 6). Stereotactic Radiosurgery (SRS) and Stereotactic Body Radiotherapy (SBRT). In StatPearls . StatPearls Publishing.