Gastroesophageal reflux disease (GERD) is a common chronic digestive disorder that occurs when stomach acids reflux back into the esophagus, causing unpleasant symptoms such as heartburn, acid reflux, and sometimes difficulty swallowing or chest pain. Although many patients respond to drug therapy and lifestyle modifications, some patients experience persistent symptoms or complications, making surgical intervention a necessary option.
GERD surgery aims to strengthen the valve between the stomach and esophagus and prevent acid from coming back up. Nissen fundoplication is the most common and effective technique for this condition and has shown us excellent results in improving patients’ lives as well as reducing dependence on long-term medications.
What is gastroesophageal reflux disease (GERD)?
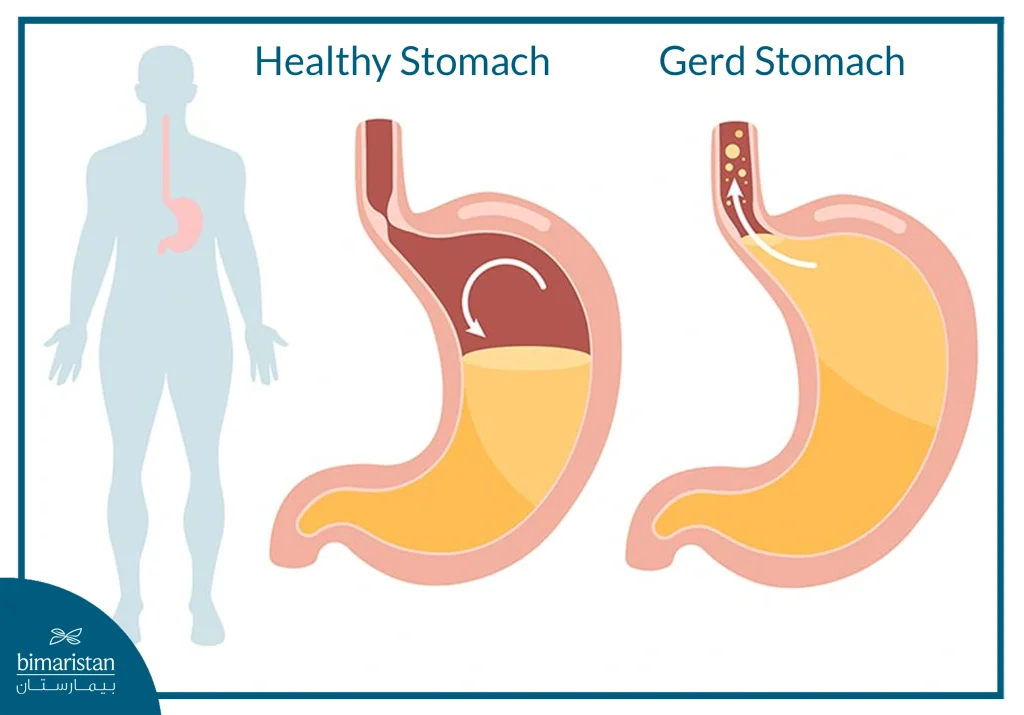
Gastroesophageal reflux disease (GERD) is a chronic disorder that occurs when stomach contents, especially acid, repeatedly flow into the esophagus. This backflow irritates the lining of the esophagus and leads to chronic symptoms and complications if left untreated. Normally, the lower esophageal sphincter (LES) prevents this reflux, but when it becomes abnormally weak or loose, reflux becomes more frequent, especially after meals or when lying down.
Common causes of acid reflux
- Weakness or relaxation of the lower esophageal sphincter (LES): The root cause of most cases of GERD, when this sphincter doesn’t close tightly, it allows acid to back up from the stomach into the esophagus.
- Hiatal Hernia: A condition that occurs when part of the stomach pushes into the chest, weakening the sphincter pressure and worsening reflux.
- Obesity: Obesity increases pressure on the abdomen, which increases the likelihood of acid reflux.
- Pregnancy: Hormonal changes and uterine pressure on the stomach contribute to sphincter loosening.
- Eating large meals or lying down immediately after eating affects stomach function and increases the chance of reflux.
- Some medications, Such as muscle relaxants or asthma medications, may affect the efficiency of the esophageal sphincter.
Common symptoms of acid reflux
- Heartburn: A burning sensation in the chest that often occurs after eating and may increase when bending over or lying down.
- Acid regurgitation: The reflux of stomach contents into the throat or mouth, and the patient feels a bitter or sour taste.
- Chest pain: Sometimes similar to heart pain but originating from the gastrointestinal tract.
- Hoarseness or chronic cough: The result of irritation of the larynx from ascending acid.
- Difficulty swallowing (dysphagia): Due to inflammation or narrowing of the esophagus caused by frequent reflux.
When does GERD surgical treatment become necessary?
GERD surgery is an important option in certain cases, especially when drug treatments do not provide adequate relief or complications arise that affect the patient’s health:
- Symptoms persist despite drug therapy: When symptoms such as heartburn, regurgitation, or chest pain persist despite adherence to treatment with PPIs or other medications, this is an indication of the need for surgical intervention.
- Impact of symptoms on daily life: If the daily symptoms of reflux significantly affect sleep, work, and social activities, and behavioral and medication modifications do not help, surgery may be recommended.
- Complications resulting from chronic reflux: Esophagitis, ulcers, strictures, or the development of Barrett’s esophagus are changes in the lining of the esophagus that may pose a future risk of esophageal cancer.
Types of surgery used to treat GERD
Surgical options for treating GERD are numerous, depending on the patient’s condition and severity of symptoms, as these procedures aim to strengthen the lower esophageal sphincter to prevent reflux of stomach acid and minimize complications:
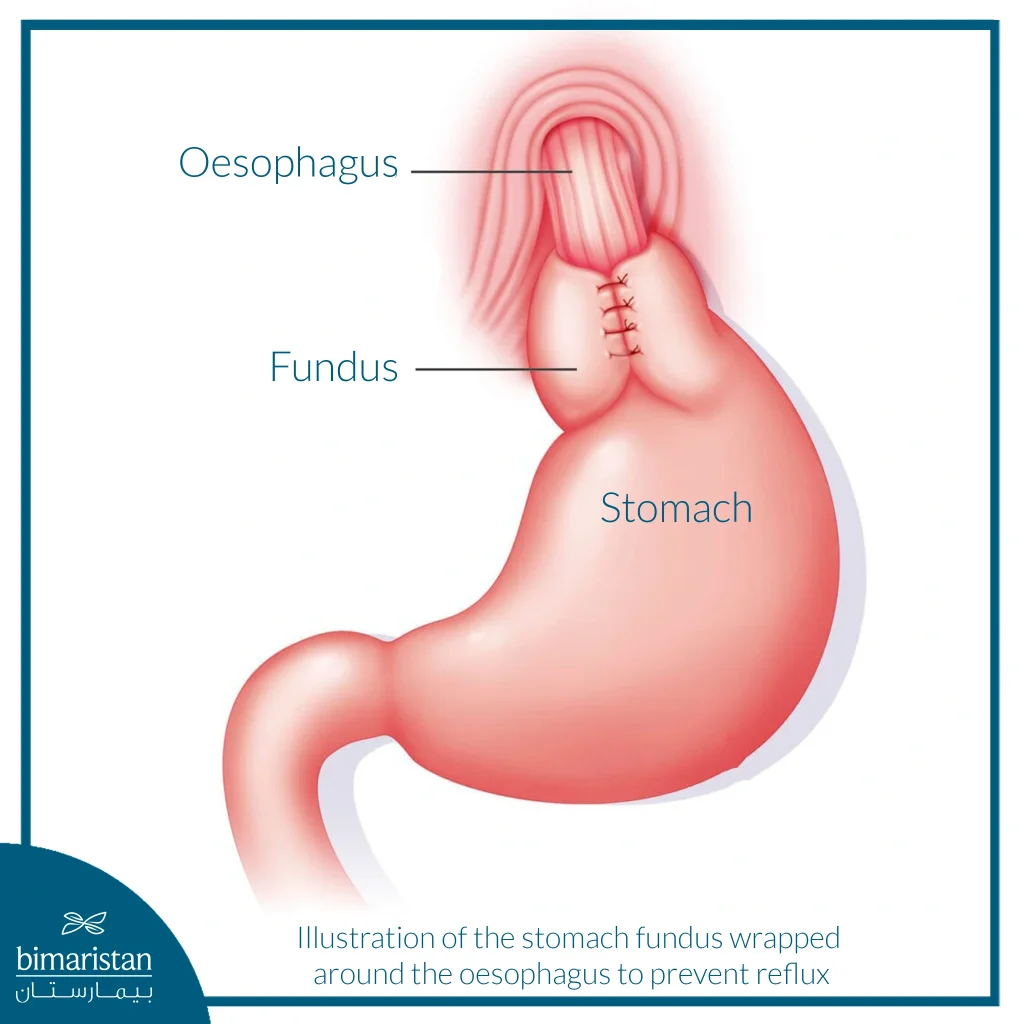
Nissen Fundoplication
The 360-degree Nissen fundoplication is the most common surgical procedure for treating GERD, in which the surgeon wraps the upper part of the stomach around the lower esophagus to strengthen the lower sphincter and prevent acid reflux. This procedure can be performed through open or laparoscopic surgery, and laparoscopy is often preferred for many reasons, including shorter recovery time and lower complication rate.
Floppy Nissen
In this type, a full fundoplication, but loose or less tight, is used to minimize post-surgical complications, such as bloating or dysphagia.
Partial Fundoplication
In some cases, especially when the movement of the esophagus is poor, a partial wrap is performed instead of a full wrap:
- Toupet Fundoplication: 270-degree rear winding.
- Dor Fundoplication: 180-degree front winding.
These procedures aim to minimize excess pressure on the esophagus, reducing the risk of dysphagia or excess gas while maintaining reasonable effectiveness against reflux
Laparoscopic vs. open surgery
All of these operations can be performed surgically in two ways:
- Laparoscopic: Performed through small incisions using a camera and precision instruments, it is characterized by less pain, shorter hospital stay, and faster recovery.
- Open surgery: Used for large hiatal hernias or complex cases, but is often associated with greater pain and a longer recovery period.
Other procedures: TIF (Transoral Incisionless Fundoplication)
TIF (Transoral Incisionless Fundoplication) is a newer option performed using a transoral endoscope without any external incision, which is used to strengthen the lower esophageal valve without traditional surgery and is suitable for patients who wish to avoid invasive surgery.
Steps to Laparoscopic Surgery for GERD
The surgery is based on strengthening the sphincter between the esophagus and the stomach and sometimes includes treatment of a hiatal hernia, if any, and is performed under general anesthesia using precise instruments through small incisions in the abdomen:
- General anesthesia: The procedure begins by giving the patient general anesthesia, which puts the patient in a deep sleep with no awareness or pain during the surgery.
- Making small incisions and inflating the abdomen: The surgeon makes 4 to 6 small incisions of 0.5 to 1 cm each in the abdominal wall, then inflates the abdomen with carbon dioxide gas to expand the space and improve visibility during the procedure.
- Insertion of the scope and surgical instruments: The surgeon inserts an endoscope with a high-definition camera to view the internal cavity, along with precision remote-controlled surgical instruments that use the camera to guide the next steps with high precision.
- Fundoplication strengthens the sphincter between the esophagus and stomach: The surgeon wraps the upper part of the stomach around the lower end of the esophagus
- Repair a hiatal hernia (if present): If there is a hiatal hernia, the slipped portion of the stomach is pulled into the abdominal cavity, the hiatal opening is sutured to narrow it, and surgical mesh may be used to support the repair area.
- Examine the area and close the incisions: After ensuring successful coiling and hernia repair, the abdominal cavity is washed with a sterile solution, the instruments are removed, the small incisions are sutured, and covered with bandages. The resulting scars are usually small and heal quickly.
- Post-operative follow-up: The patient is transferred to the post-anesthesia care unit, where his vital status is monitored, and he is allowed to take fluids after several hours, and the diet is graduated over the following days.
Advantages of GERD surgery
- Eliminating chronic medications: Surgery allows many patients to discontinue or significantly reduce the dosage of proton pump inhibitors (PPIs), minimizing the side effects associated with long-term use.
- Significantly improved symptoms: Heartburn, reflux, and associated respiratory symptoms (such as chronic coughing or asthma) are significantly reduced.
- Long-term efficacy: Studies show that a significant percentage of patients achieve lasting symptom improvement for years after surgery with low rates of recurrence.
- Improved quality of life: After surgery, most patients feel a great deal of physical and psychological relief due to the absence of unpleasant symptoms and the ability to eat and sleep normally without the need for ongoing medication.
- Simultaneous hiatal hernia repair: If a hiatal hernia is present, it is repaired during surgery to minimize the occurrence of reflux in the future.
Risks and possible complications
Although surgery to treat GERD is safe and effective in most cases, there are some risks and potential complications to consider:
- Temporary difficulty swallowing, especially in the first few weeks after surgery
- Gas buildup and bloating due to changes in airflow during eating
- Inability to burp or vomit easily after surgery
- Reflux symptoms may return in a small percentage of patients, especially in the long term
- Injury to the vagus nerve or neighboring organs during surgery (rare)
- Infection or bleeding at the surgery site
- The need for reoperation in very rare cases due to failure or disintegration of the coil
Life after GERD surgery
After GERD surgery, the patient begins a recovery phase that includes three main aspects: Diet, recovery, and medical follow-up. He usually starts with clear liquids for a few days and then gradually moves to full liquids and pureed foods for up to 4-6 weeks, until the lining of the esophagus stabilizes after Nissen reflux surgery, and the patient is encouraged to move lightly and walk for the first few days, and avoid strenuous activities for several weeks. To prevent respiratory complications, a motivational spirometer is used for respiratory exercises.
Regular follow-up 10-14 days after discharge, for dietary adjustment and clinical monitoring, enhances the chances of successful GERD surgical treatment and long-term stability.
GERD surgery is an effective and safe option for patients who have not responded to pharmacological treatments or suffer from chronic reflux complications. Nissen reflux surgery, thanks to its advanced techniques, provides excellent results in terms of reducing symptoms and improving quality of life. Although there are some potential risks and complications, they are limited and manageable when the surgery is chosen at the right time and under specialized medical supervision. Regular follow-up and adherence to post-operative recommendations, especially in terms of diet and physical activity, play an important role in the long-term success of GERD surgical treatment.
Sources:
- Katz, P. O., Gerson, L. B., & Vela, M. F. (2024). Gastroesophageal Reflux Disease. In StatPearls. StatPearls Publishing.
- MedlinePlus. (2024). GERD. U.S. National Library of Medicine.