Congenital heart defects are one of the most common cardiac disorders from birth, ranging from simple cases that may not cause obvious symptoms to others that need early evaluation and treatment to avoid affecting the heart and lungs over time. In recent years, significant advances in cardiology have improved diagnostic methods and expanded treatment options, especially with the spread of minimally invasive interventional procedures. Patent ductus arteriosus (PDA) closure is one such modern intervention that has changed the way some heart defects are treated, in terms of safety, outcomes, and speed of recovery.
What is a patent ductus arteriosus?
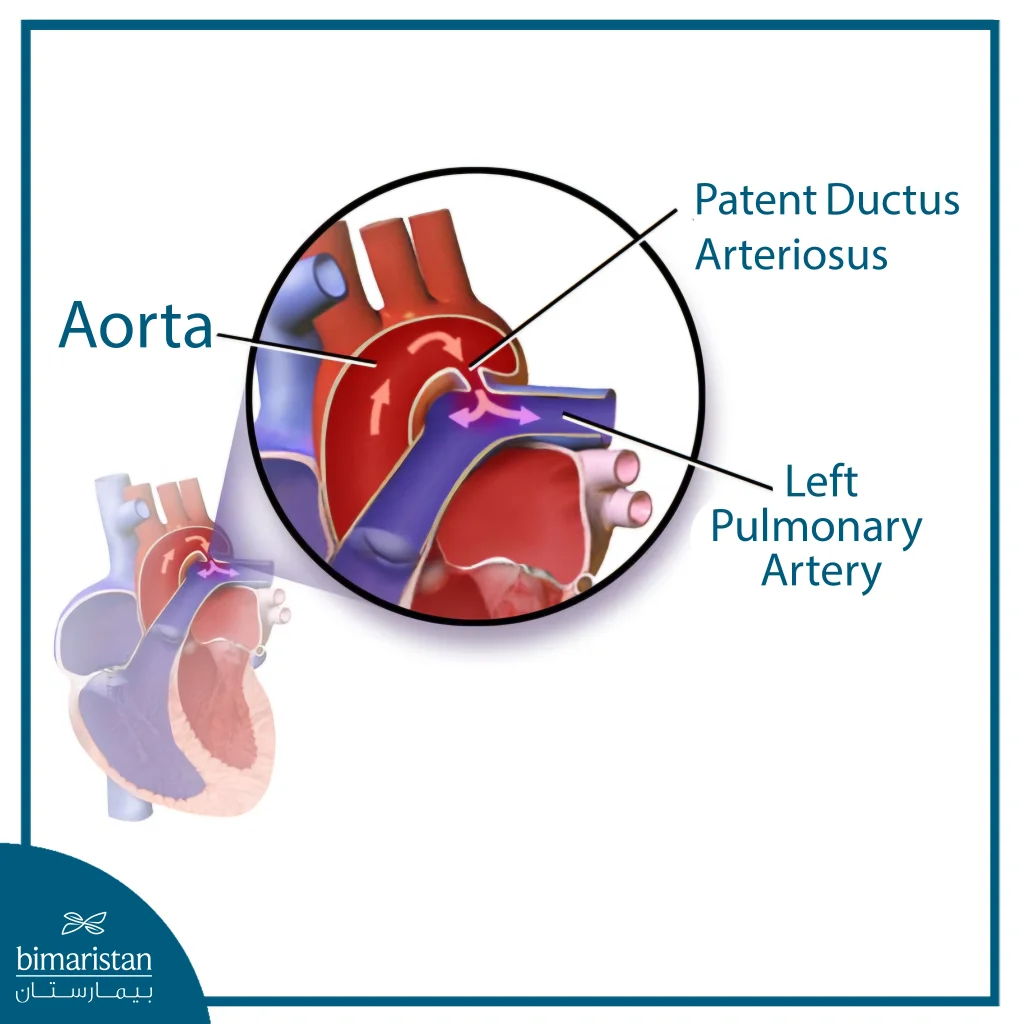
The ductus arteriosus is a normal blood vessel found in the fetus before birth, connecting the aorta to the pulmonary artery, whose function is to allow blood to pass away from the non-functioning lungs in the womb. After birth, with the first breaths and the lungs beginning to function, the course of the blood circulation changes, and the ductus arteriosus should close spontaneously within a short time.
In some babies, the ductus arteriosus does not close as expected and remains open after birth, a condition known as patent ductus arteriosus. In this condition, blood passes from the aorta into the pulmonary artery, resulting in abnormal blood flow to the lungs. A small patent ductus arteriosus may not cause any obvious issues, while a larger ductus may put more strain on the heart and lungs, making closure of the patent ductus arteriosus necessary in some cases to avoid later complications.
Causes of patent ductus arteriosus
In some cases, the exact cause of a patent ductus arteriosus is not known, as this condition can occur without an obvious factor explaining the lack of normal closure after birth, but there are known factors that may increase the likelihood of it occurring, including the following:
- Premature birth, where the ductus arteriosus is more likely not to close in premature babies than in full-term babies
- Genetic factors or a family history of congenital heart defects
- Female gender, as patent ductus arteriosus is seen more often in females than in males
- The mother had rubella during pregnancy, which increases the risk of this condition in the newborn
- Neonatal respiratory distress syndrome, which occurs in babies whose lungs don’t produce enough sorfactant for normal lung function
- Associated with other congenital heart defects in some cases
Even if the cause is unclear, a patent ductus arteriosus may lead to increased blood flow to the lungs and heart, requiring medical evaluation to determine the need for patent ductus arteriosus treatment and appropriate follow-up.
Patent ductus arteriosus symptoms
Symptoms of a patent ductus arteriosus vary depending on the size of the opening and may be mild or unnoticeable in some cases, especially when the duct is small. On the other hand, a larger duct may lead to obvious symptoms, and some of these symptoms may appear during infancy or childhood. Possible symptoms include the following:
- Rapid or difficult breathing
- shortness of breath
- Rapid fatigue or exhaustion
- Sweating while feeding or eating
- Difficulty nursing or feeding
- Slow weight gain or delayed growth
- Rapid heartbeat or strong pulse
- A heart murmur caused by abnormal blood flow
- Increased susceptibility to recurrent respiratory infections
In some cases, a patent ductus arteriosus may be asymptomatic and discovered accidentally during a routine medical examination.
Is a patent ductus arteriosus dangerous?
The severity of a patent ductus arteriosus depends on its size and how long it remains untreated. Small cases may not cause any significant complications, but a large duct left untreated can lead to significant health complications over time due to abnormal blood flow between the heart and lungs. Possible complications include
- High pulmonary artery pressure: Excess blood flow increases the pressure within the blood vessels in the lungs, and over time, this can cause permanent damage to the pulmonary vessels and, in severe cases, can lead to life-threatening Eisenmenger syndrome.
- Heart failure: This is the result of excessive strain on the heart muscle, and may manifest as rapid breathing or difficulty breathing with poor weight gain.
- Inflammation of the lining of the heart (endocarditis): A patent ductus arteriosus increases the risk of germs adhering to the heart walls or valves, which can lead to serious harm if not treated quickly.
For this reason, early evaluation is essential to determine the severity and choose timely closure of the patent ductus arteriosus in order to prevent these complications.
How is a patent ductus arteriosus diagnosed?
The diagnosis of a patent ductus arteriosus usually begins with a clinical examination and history taking, as the doctor may notice abnormal signs while listening to the heart, such as a heart murmur. When the condition is suspected, diagnostic tests are used to help confirm the diagnosis and assess the impact of the duct on the heart and lungs. The tests used include the following:
- Echocardiography: This is the most important test to diagnose a patent ductus arteriosus, as it shows blood flow within the heart and blood vessels, determines the presence and size of the opening, and helps assess the pressure within the pulmonary arteries.
- Chest X-ray: This is used to assess the size of the heart and the condition of the lungs, and may show signs of increased blood flow to the lungs.
- Electrocardiogram (ECG): Records the electrical activity of the heart and helps detect arrhythmias or signs of myocardial strain.
- Cardiac catheterization: It is not necessary in most diagnostic cases, but may be used in selected cases, especially when other heart defects are suspected, and can sometimes be used as a therapeutic method to perform patent ductus arteriosus closure.
Patent ductus arteriosus can be diagnosed in childhood or later in life, especially in small cases that don’t cause obvious symptoms early on.
When does a patent ductus arteriosus need treatment?
Not all people with a patent ductus arteriosus need immediate treatment, and intervention is decided based on a set of medical criteria that assess how the ductus is affecting the heart and lungs. Factors that may prompt a cardiologist to consider treating a patent ductus arteriosus include the following:
- The size of the ductus arteriosus: Large ductus arteriosus, which allows significant blood flow from the aorta to the pulmonary artery, are more likely to require treatment than small ductus arteriosus, which may be asymptomatic.
- Symptoms or effects on vital functions: Poor growth, rapid fatigue, or breathing difficulties, indicating that the channel is affecting the activity of the heart and lungs.
- Presence of effects on the heart or pulmonary vessels: Evidence of increased pressure in the pulmonary arteries or excessive pumping of the heart is an indication for therapeutic intervention.
- Abnormal blood flow within the heart: When there are signs of abnormal blood flow or enlargement of the heart cavities due to the conduit.
However, in cases where the duct is small, does not affect vital functions, and does not cause obvious symptoms, the doctor can sometimes only observe and follow up without immediate treatment, allowing it to be monitored over time.
Patent ductus arteriosus treatment methods
Patent ductus arteriosus treatment methods depend on the patient’s age, the size of the duct, and its effect on the heart and lungs. In some cases, especially when the duct is small and does not cause severe symptoms, treatment may not be necessary, and regular medical follow-up is sufficient. In other cases, several treatment options are available to close the duct and prevent continued abnormal blood flow.
Drug therapy in selected cases
Drug therapy is mainly used in premature babies with patent ductus arteriosus, where drugs from the NSAID class can be given to help stimulate closure of the duct. The effectiveness of this treatment is limited in certain cases and is not usually used in full-term babies or in older children and adults, as it does not lead to closure of the duct.
Surgical treatment
Surgical treatment is a treatment option in cases that do not respond to drug therapy, or when the ductus arteriosus is large or causing obvious health issues. During surgery, the duct is accessed and closed directly using sutures or metal clips. Although effective, this option requires a longer recovery period compared to modern interventional procedures.
Catheter closure of the patent ductus arteriosus
Used as a treatment option in older children and adults, transcatheter patent ductus arteriosus closure is an interventional procedure performed without the need for open-heart surgery. It is less invasive than traditional surgery and is often associated with a shorter hospital stay and faster recovery, making it an appropriate option in many cases where medical evaluation allows it.
Catheter closure steps for patent ductus arteriosus
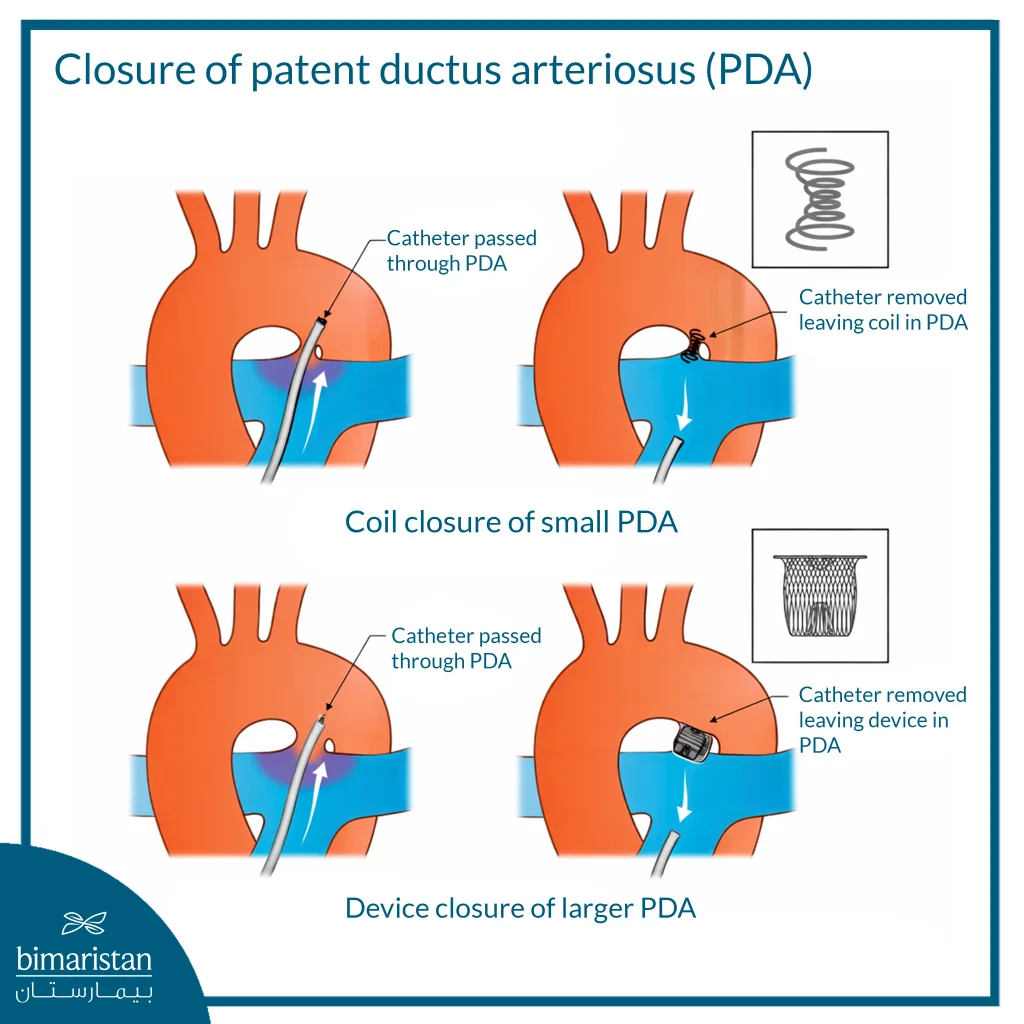
Catheter closure of a patent ductus arteriosus is a common interventional procedure that aims to close the duct without the need for open-heart surgery. The procedure relies on the use of a thin catheter that is precisely guided to the site of the duct. The steps of the procedure generally include the following:
- Inserting a thin, flexible catheter through a blood vessel, often from the groin area
- Guide the catheter through the blood vessels until it reaches the heart and the location of the ductus arteriosus
- Passing a special tool through the catheter, such as a coil or plug, and placing it inside the canal to close it
- Ensure that the abnormal blood flow through the canal has stopped after the device is in place
This procedure is not usually used in premature babies due to the small size of their blood vessels, but it can be performed later if the canal is still present, and in most cases the patient does not need to stay in the hospital for a long time, and the recovery period is shorter compared to traditional surgery.
Results of patent ductus arteriosus (PDA) closure and follow-up after treatment
The results after patent ductus arteriosus treatment are very good in most cases, especially in children who do not have other heart defects. After closure of the conduit, most children are able to lead a normal life, with significant improvement in activity and growth, with no restrictions on daily activities.
In very rare cases, additional intervention may be needed if the duct reopens after treatment, but this is uncommon, and people who received treatment in childhood are advised to follow up later with a doctor who specializes in adult congenital heart disease as they age.
Medical follow-up after treatment
Even after the ductus arteriosus is closed, some patients may need periodic medical follow-ups for long periods of time, sometimes for life, to make sure no subsequent cardiac or pulmonary issues arise. These follow-ups include tests that are determined by the cardiologist based on the individual case and the appropriate care plan.
Recovery period after surgery
After surgery, most children stay in the hospital for several days, and some may require special care in the pediatric intensive care unit. The speed of recovery depends on the child’s age and overall health, and after discharge, parents are given clear instructions regarding nutrition, wound care, medications, physical activity, and follow-up appointments.
After the catheterization procedure
After the catheter closure, the child is kept under observation in the hospital for several hours, often able to go home the same day, but in some cases an overnight stay may be required. An X-ray is taken to make sure the closure is in place, and this test may be ordered the next day.
Subsequent review and prevention of infections
A follow-up appointment is scheduled with the cardiologist about six months after the procedure, during which an echocardiogram is performed to confirm complete closure of the canal. Antibiotics may be recommended before and after certain dental procedures for six months after treatment to prevent endocarditis, and the doctor will determine if there is a need to extend this period.
Patent ductus arteriosus is a congenital heart defect that can be effectively diagnosed and treated when detected in a timely manner. Careful medical follow-up helps determine the need for treatment and select the most appropriate option for each case, ensuring that the heart and lungs are protected from the long-term effects. With the development of treatments, closure of the patent ductus arteriosus has become a safe and successful procedure in most cases, allowing patients to return to a normal life with significant improvements in health and development, especially when adhering to the follow-up plan after treatment.
Sources:
- American Heart Association. (n.d.). Patent ductus arteriosus (PDA).
- Hopkins Medicine. (n.d.). Patent ductus arteriosus (PDA). Johns Hopkins Medicine.

