Many people around the world suffer from hemifacial spasm, a painful condition that affects the facial nerve and causes involuntary contractions. Studies indicate that this issue affects approximately 5 to 10 people per 100,000 annually and is more common in middle-aged women. The symptoms of hemifacial spasm may start suddenly or gradually, affecting facial expressions and, in some cases, vision. Although the exact cause is not always known, several effective treatments can help relieve discomfort and improve quality of life.
What is hemifacial spasm?
Hemifacial spasm is a neuromuscular disorder that causes involuntary muscle contractions on one side of the face. Symptoms usually start with eyelid twitches that appear as rapid, frequent eye closure, and may then spread to the muscles of the cheeks and the area around the mouth as the condition progresses.
These involuntary movements are caused by abnormal stimulation of the facial nerve, which controls the facial muscles. This condition is more commonly observed in women, and the symptoms typically appear between the ages of 40 and 60.
Causes of hemifacial spasm
Hemifacial spasm is caused by repeated involuntary stimulation of the facial nerve. Repeated stimulation of the facial nerve may occur for one of the following reasons:
- A tumor-like mass pressing on the seventh nerve
- A malformed blood vessel pressing on the facial nerve
- Direct traumatic injury to the nerve
- Unknown reasons
Symptoms of hemifacial spasm
Spasms of the right or left half of the face cause unpleasant symptoms and embarrassment for the patient, due to fear of their appearance. The symptoms appear as follows:
- Frequent eye twitching (fluttering) on one side
- Sleep apnea wakes the patient from sleep
- Some people experience hearing loss and tinnitus
- Increased facial contractions when you’re tired, stressed, emotional, or crying
- Over time, spasms may occur in other facial muscles, such as those in the cheeks and around the mouth
- In severe cases, the lower jaw may spasm, causing it to shift to one side
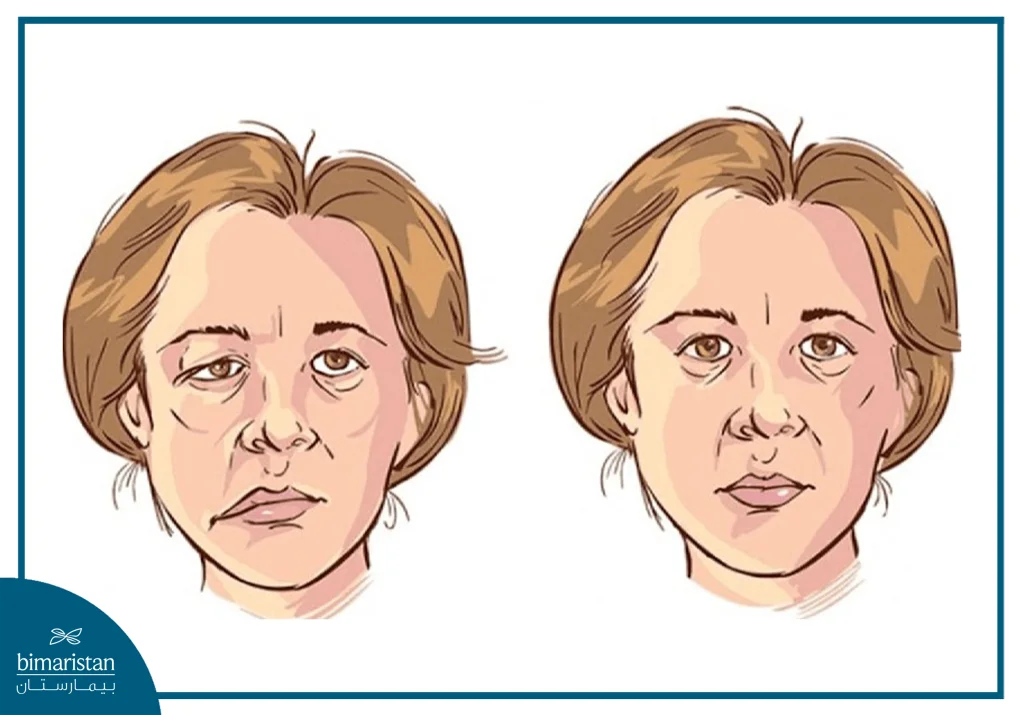
Diagnosis of hemifacial spasm
Hemifacial spasm is diagnosed by observing involuntary movements on one side of the face during a clinical examination, the doctor usually requests a magnetic resonance imaging (MRI) to rule out other possible causes such as tumors, structural abnormalities, or diseases such as multiple sclerosis, but in some cases, the doctor may resort to injecting a contrast agent to visualize abnormal blood vessels that may compress the facial nerve, and overall, the diagnosis depends mainly on clinical signs and ancillary imaging tests.
Treating hemifacial spasm once and for all
Treatment methods vary depending on the severity of symptoms and the degree of response:
Drug therapy
For mild symptoms, anticonvulsant medications (carbamazepine, clonazepam) can be used to intercept the nerve signals that cause tics.
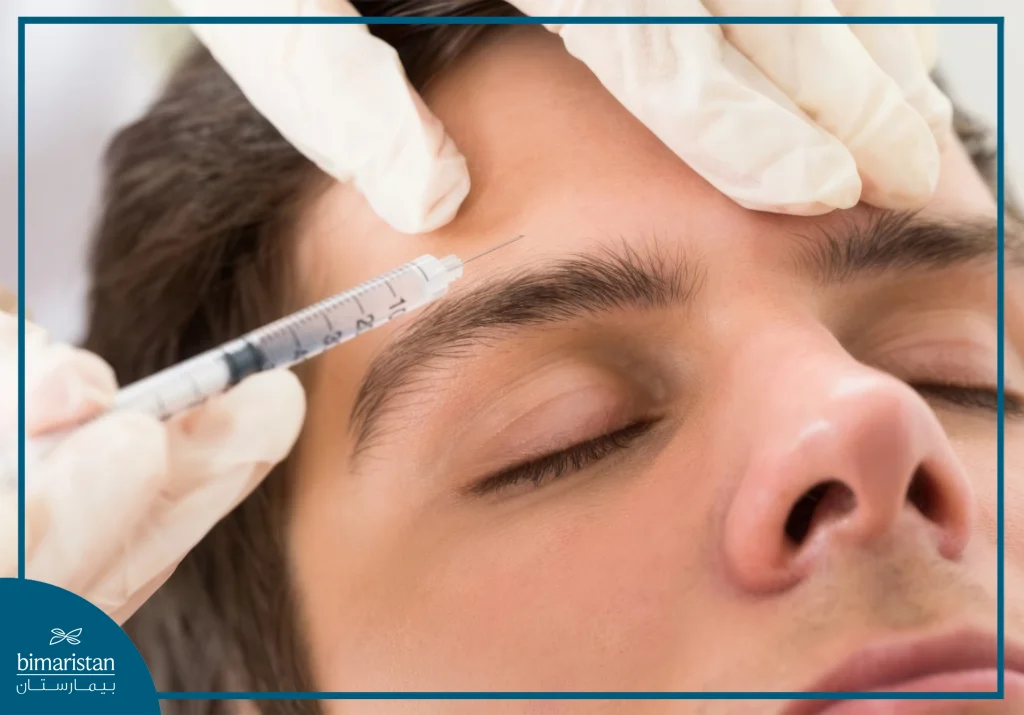
Botulinum toxin injections
It is considered the most effective treatment in most cases, and it involves injecting low doses of botulinum around the muscles affected by tics, as botulinum weakens the movement of the injected muscles and helps prevent spasms. Botox injections must be repeated in most patients once every 3-6 months. Botulinum injection may be associated with muscle discomfort, fatigue, dizziness, fever, skin rash, and dry mouth, and rarely, serious symptoms may occur if the dose is increased.
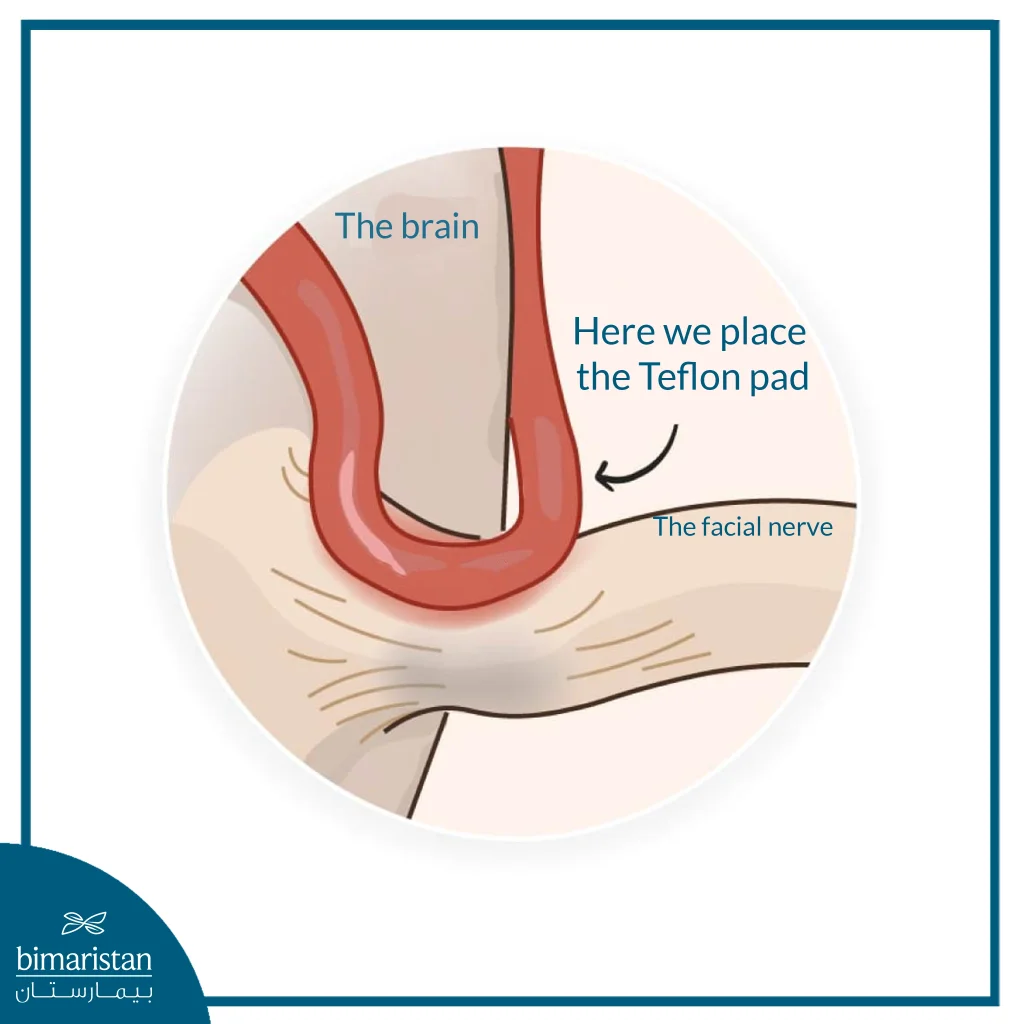
Microvascular decompression surgery
If blood vessels are pressing on the facial nerve, surgery can be performed. The neurosurgeon makes an opening in the skull and exposes the facial nerve where it exits the brainstem. The blood vessels in contact with the nerve are identified, and the surgeon places a small Teflon pad to separate the blood vessels from the facial nerve.
What are the results of the surgery?
This surgery usually achieves excellent and satisfactory results for patients, with most leaving the hospital within two to three days after the procedure. When performed efficiently by an experienced surgeon, the symptoms disappear immediately after the intervention.
Risks of surgical work
No surgical procedure is completely risk-free; some patients have reported temporary facial muscle weakness after surgery, and rare cases of hearing loss have been reported.
Prevention of hemifacial spasm
Unfortunately, there are no specific preventive methods to prevent the occurrence of hemifacial spasm, as its causes are often not known precisely, but nevertheless, it is recommended to control stress and anxiety factors that may contribute to worsening symptoms, and avoiding sudden exposure to cold air or strong air currents may help reduce the possibility of triggering seizures, and it is also recommended to periodically follow up with a doctor when any initial symptoms such as eyelid twitching are noticed, but in the end early diagnosis and prompt treatment remain the best ways to control this condition.
Diseases similar to hemifacial spasm
There are other diseases that present with symptoms somewhat similar to facial spasm, such as:
- Facial nerve palsy, also commonly known as Bell’s palsy
- Head and neck tumors, benign or malignant
- Oculomotor neuritis (third nerve damage)
- Blepharospasm is a disease; it is important to distinguish between the two diseases, as Blepharospasm usually affects only the small muscles around the eyelids, while Bell’s palsy can affect several muscles in the face.
In conclusion, Bell’s palsy is a condition that can be successfully managed with proper diagnosis and early treatment. At Bimaristan Medical Center, we provide comprehensive care, including the latest diagnostic and therapeutic techniques, to ensure the best outcomes for patients. With our team of experienced specialists, we ensure a comfortable treatment journey and satisfying results that restore the quality of life you deserve.
Learn about the causes and symptoms of hemifacial spasm and its effective treatments. Discover medical tips and accurate diagnoses to relieve pain and improve quality of life.
Sources:
- National Institute of Neurological Disorders and Stroke. (2022). Hemifacial spasm information page
- American Association of Neurological Surgeons. (2020). Hemifacial spasm.

