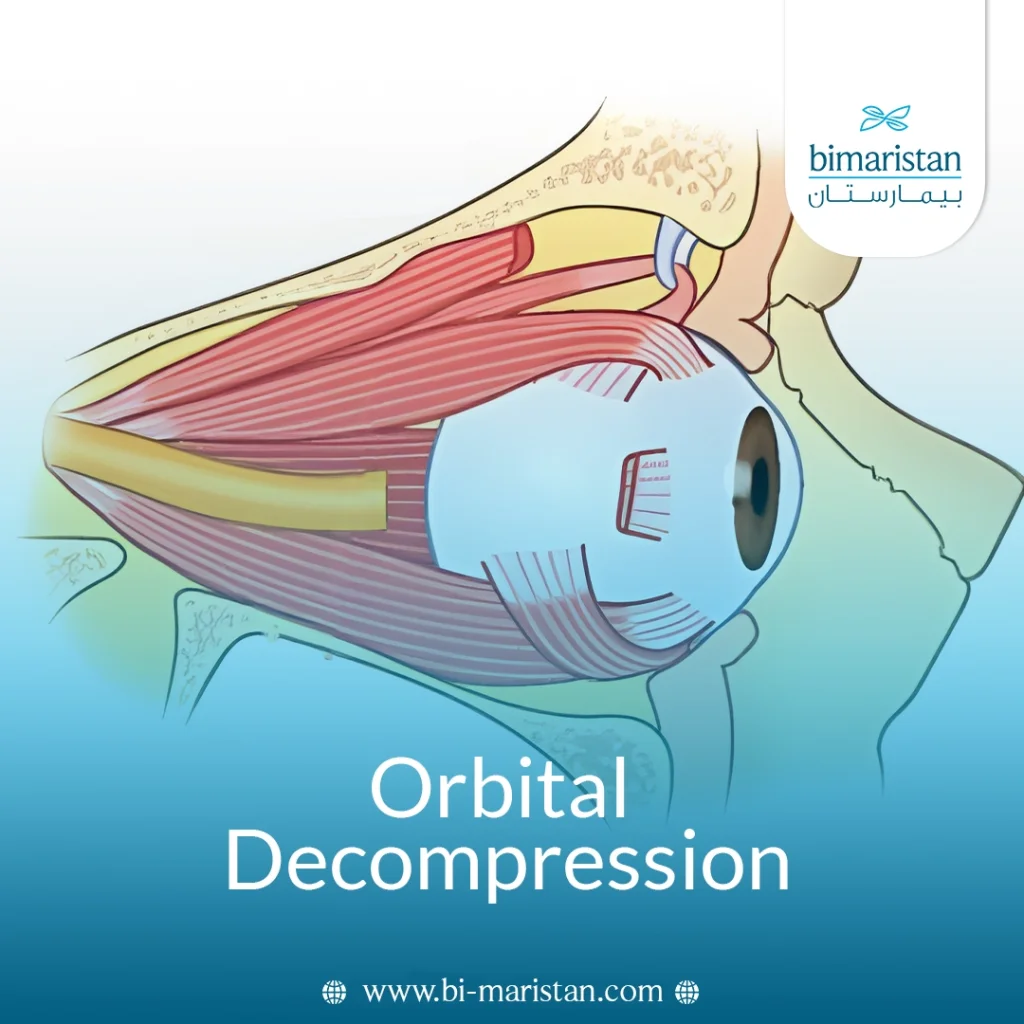
The eye socket is a bony space that houses the eye, motor muscles, nerves, blood vessels, and supporting tissues. Any increase in the size of these components or swelling within this confined space can raise intraorbital pressure, which can directly affect vision and eye function. In some cases, this elevation is mild and manageable, while in others it can become a serious issue that threatens the integrity of the optic nerve and requires careful therapeutic intervention.
The importance of early recognition of orbital pressure, understanding its causes and symptoms, and working towards orbital decompression, as timely intervention may prevent permanent complications to vision or eye movement. Hence, the importance of highlighting the concept of orbital pressure and its role in making the appropriate treatment decision.
What is Orbital compression?
Orbital compression is a condition in which there is increased pressure within the eye socket due to congestion or enlargement of one of its components, such as the orbital muscle or fat, or a pathological mass such as inflammation, hemorrhage, or tumor. Due to the closed bony nature of the orbit, any increase in volume has no room to expand, pushing the eye forward or putting pressure on the optic nerve and other sensitive structures.
Depending on the cause, orbital hypertension can be gradual or severe and may be accompanied by eye protrusion, pain, difficulty moving the eye, or decreased visual ability. The severity of the condition varies from patient to patient, which subsequently determines the nature of the treatment, whether it is conservative, pharmaceutical, or surgical, by relieving orbital pressure.
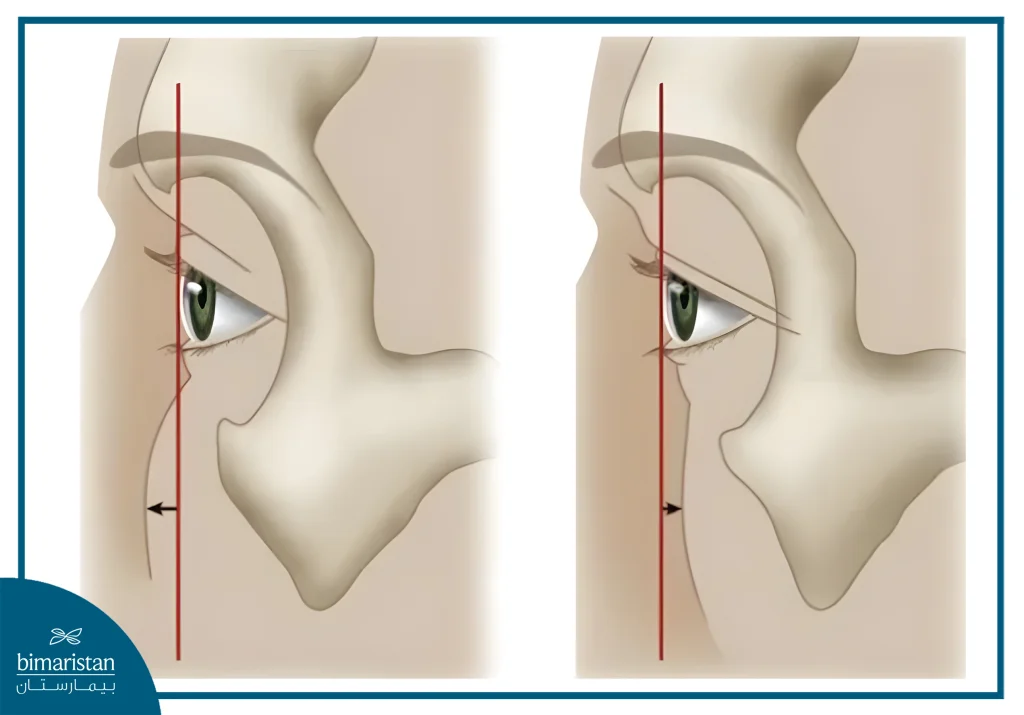
Causes of High orbital Pressure
High orbital pressure is caused by a combination of causes that increase the volume of contents within the eye socket or impede the drainage of blood and fluids from it. These causes vary in severity and speed of progression, which is reflected in the symptoms and treatment options.
Thyroid ophthalmopathy
Thyroid-related ophthalmopathy is one of the most common causes of high orbital pressure. In this condition, the eye muscles and adipose tissue become enlarged as a result of an immune reaction, leading to intraorbital congestion and protrusion of the eye, which may be accompanied by dry eye, double vision or, in advanced cases, pressure on the optic nerve.
Intra-orbital tumors
Benign or malignant tumors within the eye socket can cause a gradual increase in pressure, especially if they grow slowly without obvious symptoms at first. As the tumor expands, it begins to press on the eye or nearby nerves, resulting in a protruding eye or decreased vision.
Inflammation and hemorrhages
Acute intraorbital infections, such as bacterial orbital inflammation, can lead to rapid swelling and a sharp rise in pressure, which are medical emergencies that require immediate intervention. Intraorbital bleeding after trauma or surgery can also cause a sudden increase in pressure with severe pain and blurred vision.
Other, less common causes
Other causes include vascular malformations, fluid retention, or certain systemic diseases that affect the orbital tissue. Although rare, if not diagnosed and treated in time, it can have a severe impact.
Symptoms of orbital pressure
Symptoms of orbital pressure vary depending on the cause and the speed of progression of the condition, and may appear gradually or suddenly.
- Visual symptoms: Blurred vision, double vision, or a gradual decrease in visual acuity.
- Functional symptoms: Difficulty or pain when moving the eye or a sensation of pressure or fullness within the eye socket.
- External symptoms: Eye protruding forward, difficulty closing the eyelids, redness or swelling around the eye.
The onset of these symptoms, especially if they are aggravated or sudden, requires a thorough medical evaluation to determine the cause and the appropriate treatment plan.
When does orbital decompression become necessary?
Not all cases of orbital hypertension require direct surgical intervention. In some mild or early cases, symptoms can be controlled with drug therapy and careful monitoring. However, orbital decompression becomes necessary when the pressure poses a real threat to vision or when conservative treatments fail to stop the progression of the condition. Surgical intervention is recommended in the following cases:
- Pressure on the optic nerve with decreased visual acuity
- Severe eye protrusion that causes difficulty closing the eyelids or damage to the cornea
- Persistent pain or rapid worsening of symptoms despite drug therapy
- A visible effect on eye movement or the appearance of troublesome double vision
- Advanced thyroid ophthalmopathy cases after disease activity has stabilized
In these circumstances, the primary goal of surgery is to protect vision and prevent permanent damage to the eye.
What is Orbital Decompression?
Orbital decompression is a surgical procedure that aims to reduce the pressure inside the eye socket by increasing the space available for its contents. This is achieved by removing part of the bony orbital walls, removing part of the orbital fat, or a combination of both, depending on the nature and severity of the condition.
This procedure helps to allow the enlarged tissue to expand into the neighboring spaces, reducing pressure on the eye and optic nerve and improving the intraorbital position of the eye. The exact type of surgical intervention is determined after a thorough clinical and radiographic evaluation.
Types and techniques of orbital decompression
Orbital decompression techniques vary depending on the cause and degree of hypertension, and the surgeon chooses the most appropriate method for each individual patient.
Bone decompression
In this type, specific parts of the bony orbital walls, such as the medial or inferior wall, are removed, allowing tissue to move into neighboring sinuses. This technique is often used in moderate to severe cases.
Lipid Decompression
This procedure is based on removing a portion of the orbital fat without affecting the bone and is preferred in cases where fat hypertrophy is the main cause of high blood pressure.
Compound dilution
This technique combines both bone and fat removal and is used in advanced cases or when a significant reduction in pressure and a marked improvement in eye prominence is needed.
Surgical methods
The procedure can be performed through incisions inside the eyelid through the nose or using modern techniques that aim to minimize scarring and speed recovery, while preserving the natural function of the eye as much as possible.
Orbital decompression steps
The orbital decompression process goes through several structured stages to ensure the best possible outcome while minimizing risk.
Preoperative preparation
Before making a surgical decision, the patient undergoes a comprehensive evaluation that includes an eye examination, visual acuity assessment, eye movement, and radiographic imaging such as CT or MRI to determine the cause and severity of the pressure. The patient’s general condition is also stabilized, especially in cases associated with thyroid disorders.
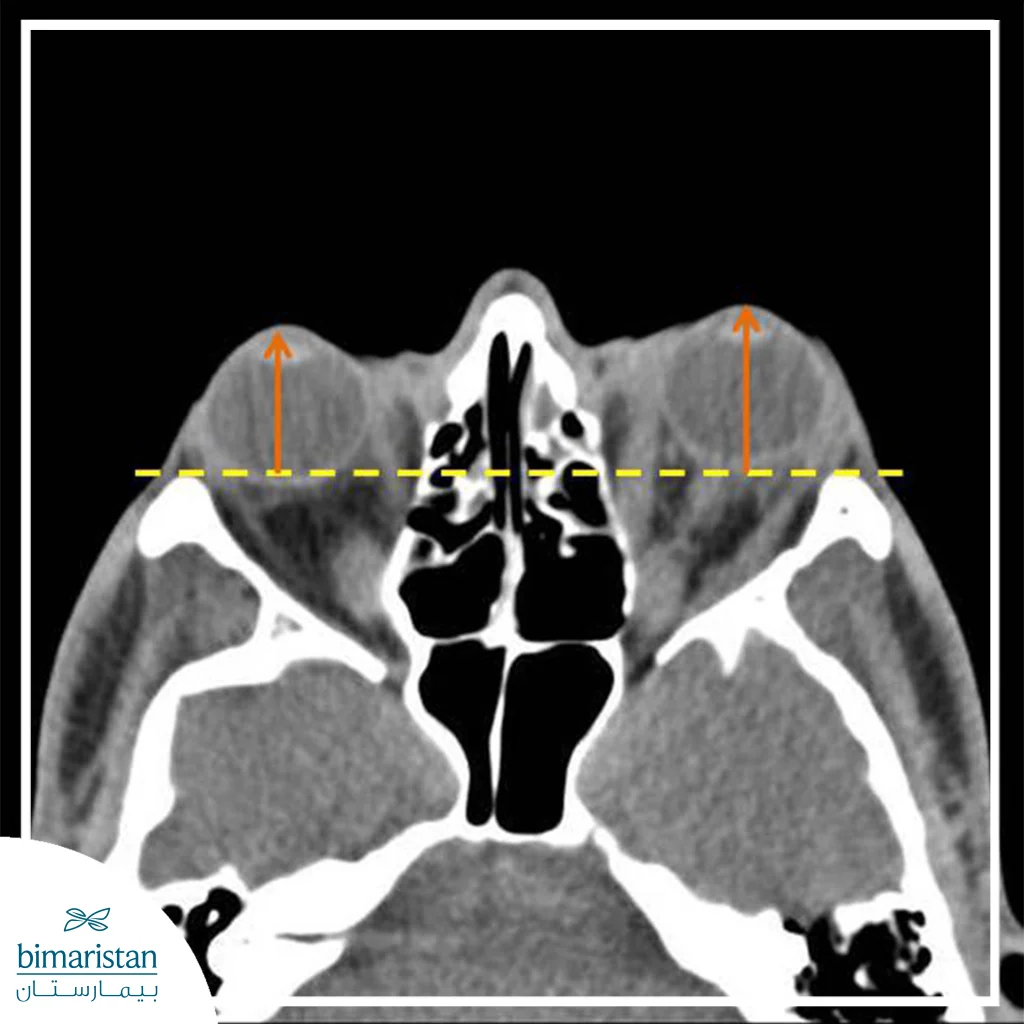
Procedure steps
The procedure is usually performed under general anesthesia. The surgeon makes tiny incisions, often on the inside of the eyelid or through the nose, to access the orbit without leaving visible external scars. A portion of the orbital bone or fat, or both, is then removed according to a predetermined surgical plan, allowing for a gradual and controlled decompression of the eye socket.
Duration of the procedure and anesthesia
The procedure usually lasts between one and two hours, but can be longer in complex cases. After completion, the patient is transferred to observation for a short period of time before returning to the room or discharged from the hospital, depending on their general condition.
Benefits and results of orbital decompression
This procedure aims to achieve a range of important functional and visual outcomes, which often reflect positively on the patient’s quality of life.
Functional results
Reducing intraorbital pressure helps reduce pain and pressure, improves the ability to move the eye more comfortably, and reduces difficulty closing the eyelids and associated ocular surface issues.
Visual results
In cases where the optic nerve is threatened, surgical intervention may preserve vision and prevent deterioration, and may even see a gradual improvement in vision after the pressure and swelling subsides.
Cosmetic results
Orbital decompression reduces eye prominence and improves facial symmetry, which has a positive effect on the appearance and self-confidence of many patients, even if the primary goal of the procedure is not cosmetic.
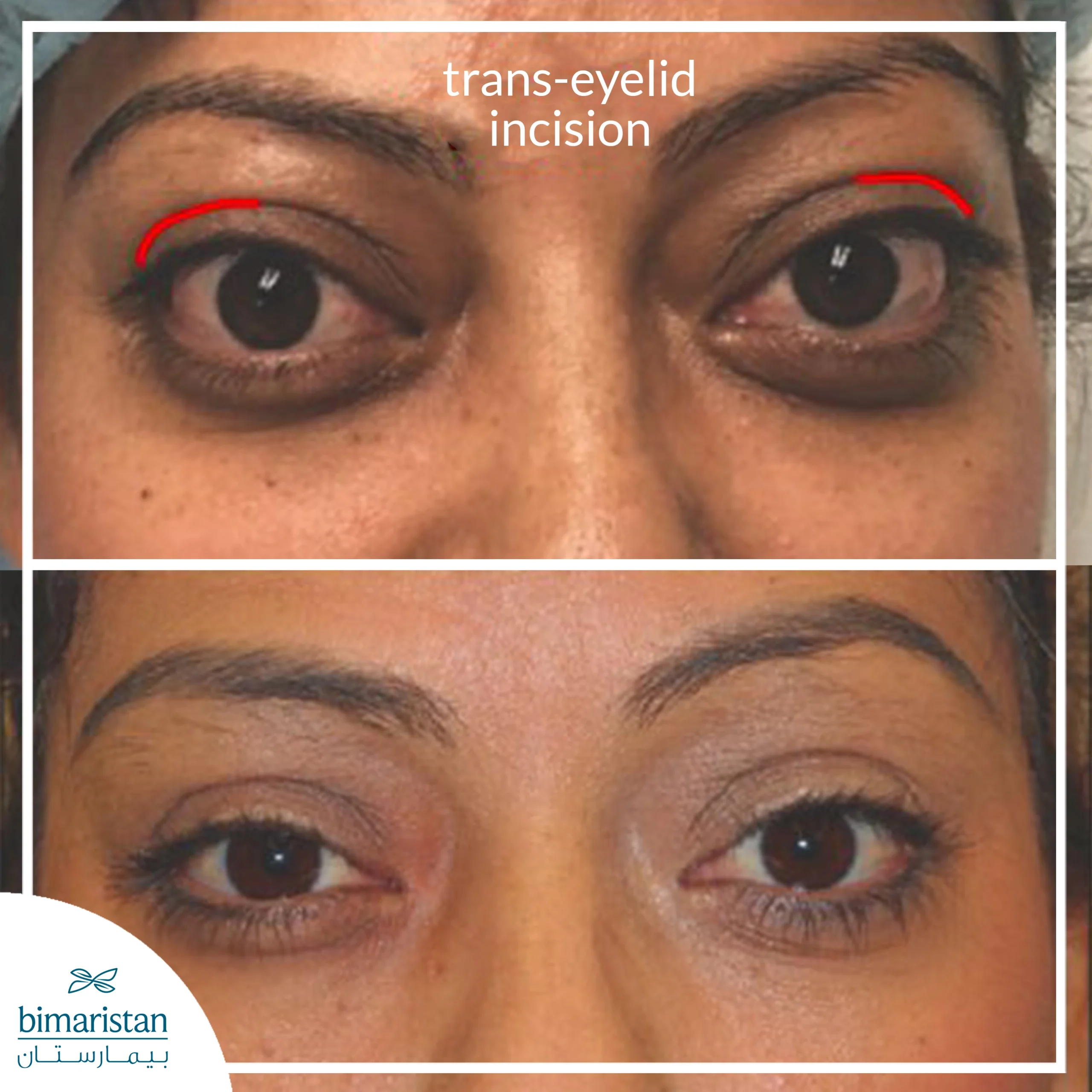
Recovery after orbital decompression surgery
The recovery period varies from person to person, but most patients notice a gradual improvement during the first few weeks after surgery. During the first few days, there may be swelling or bluishness around the eye, which is normal and will gradually subside. The patient is advised to adhere to the prescribed medications, use cold compresses when needed, and avoid physical exertion or extreme bending for a specific period of time.
Regular follow-up with an ophthalmologist to assess eye position, muscle movement, and vision improvement is usually done and the final results may take several weeks to months to fully stabilize.
Success rate of orbital decompression surgery and factors affecting it
Orbital decompression surgery has a high success rate, especially when performed at the right time and before permanent damage to the optic nerve occurs. The earlier the diagnosis is made and the more appropriate the treatment plan, the better the outcome. Factors that affect the success of the procedure include:
- Patient adherence to instructions and follow-up after surgery
- Cause of high orbital pressure
- Severity of the condition before intervention
- Surgical team experience
Can orbital decompression be repeated?
In some cases, it may be possible to repeat the surgical procedure if the pressure persists or the improvement from the first operation does not materialize. This decision is made after careful evaluation of symptoms, imaging results, and the impact of the condition on vision. On the other hand, a repeat procedure may not be recommended if the risks are higher than the expected benefit or if the symptoms are stable and do not pose a functional threat to the eye.
In conclusion, orbital decompression is an important therapeutic procedure in cases where high intraorbital pressure threatens vision or affects ocular function and quality of life. With an accurate diagnosis and the right timing and technique, positive functional and visual outcomes can be achieved, with a marked improvement in symptoms and ocular appearance.
Sources:
- American Academy of Ophthalmology. (2022). Orbital decompression surgery. In Basic and Clinical Science Course (BCSC): Oculofacial Plastic and Orbital Surgery. San Francisco, CA: AAO.
- American Academy of Ophthalmology. (2023). Orbital decompression. EyeWiki.
- Imperial College Healthcare NHS Trust. (2021). Orbital decompression surgery: Information for patients, relatives and carers.