Ankylosing spondylitis is a chronic inflammatory condition that targets the spine and sacroiliac joints, gradually causing stiffness and reduced flexibility of the vertebrae, which limits back movement over time. The disease typically presents with persistent back pain that worsens in the morning and improves with activity, and may also affect other major joints, such as the hips and shoulders.
This condition is among the most common forms of inflammatory arthritis in young adults, often emerging in the third and fourth decades of life, making it a significant cause of reduced work capacity and productivity, as well as a notable economic and health burden at the community level. Although ankylosing spondylitis has no complete cure, early diagnosis and consistent treatment under medical supervision play a crucial role in controlling inflammation, easing pain, and greatly enhancing quality of life, allowing patients to carry out daily activities more normally.
What is ankylosing spondylitis?
Ankylosing spondylitis is a chronic autoimmune disease that primarily affects the spine and the joints connecting the lower back to the pelvic bones, causing persistent inflammation that, over time, leads to stiffness and fusion of the vertebrae, reducing the spine’s natural flexibility and causing back curvature and difficulty with movement.
The disease arises from an abnormal immune response against joint and ligament tissues, and studies indicate a strong genetic predisposition, especially in those who carry the HLA-B27 gene. Symptoms usually begin with pain and stiffness in the lower back or hips that gradually spread upward, often increasing in intensity early in the morning or after periods of inactivity and improving with activity and movement. Over time, the inflammation can involve other areas of the body, such as the eyes, heart, or lungs.
What are the causes of ankylosing spondylitis?
The causes of ankylosing spondylitis result from a complex interplay of genetic, immunologic, and environmental factors, each of which contributes to the onset or progression of the disease:
- Genetic factors: Having the HLA-B27 gene significantly increases the risk, as it promotes abnormal immune responses in the joints.
- Immune dysfunction: A disorder that causes the immune system to attack the joint and ligament tissues instead of protecting them, leading to chronic inflammation.
- Hormonal and sexual factors: The disease is more common in men, suggesting that male hormones may play a role in its development.
- Environmental factors: Certain intestinal or urinary infections may trigger the disease in genetically predisposed people.
- Family factors: The risk increases with a family history of rheumatic diseases or ankylosing spondylitis.
Ankylosing spondylitis symptoms
The bony symptoms of ankylosing spondylitis develop gradually and result from chronic inflammation of the joints and ligaments surrounding the spine, leading to increasing pain and stiffness over time. Symptoms often worsen in the morning or after periods of inactivity and improve with physical activity:
- Chronic lower back pain that radiates to the buttocks or thighs
- Stiffness in the spine, especially when waking up in the morning
- Limited back mobility and difficulty bending or turning
- Pain in the hip and shoulder joints occurs as the inflammation spreads to those areas
- Curvature in the upper back over time
- Sometimes pain or swelling in peripheral joints, such as the knees or heels

Extra-articular complications of ankylosing spondylitis
The extra-articular symptoms of ankylosing spondylitis affect multiple body systems due to the disease’s autoimmune nature; the inflammation is not confined to the joints but also extends to other tissues and organs, thereby increasing the clinical complexity of the condition. These symptoms vary in severity among patients and may worsen during periods of active disease. The most significant extra-articular symptoms include:
- Inflammation of the eye (uveitis), causing redness, pain, and blurred vision
- Inflammation of tendons, especially where they attach to bones, such as the Achilles tendon behind the heel
- Heart disorders such as aortitis or arrhythmias
- Injury to the lungs due to hardening of the chest wall and impaired breathing
- General fatigue, loss of appetite, and weight loss as the disease progresses
- In some rare cases, inflammation of the kidneys or gastrointestinal tract may occur
Diagnosis of ankylosing spondylitis
The diagnosis of ankylosing spondylitis is based on a combination of clinical symptoms, laboratory tests, and radiographs that reveal inflammatory and structural changes in the spine and sacroiliac joints. Early diagnosis aims to initiate timely treatment to relieve inflammation and prevent permanent stiffness in the vertebrae:
- History and clinical examination: The doctor begins by assessing the nature, location, and duration of pain, morning stiffness, and difficulty moving, and checking the flexibility of the spine and joints.
- Laboratory tests: These are used to detect inflammatory markers, such as elevated erythrocyte sedimentation rate or C-reactive protein (CRP), and to perform HLA-B27 testing to assess genetic predisposition.
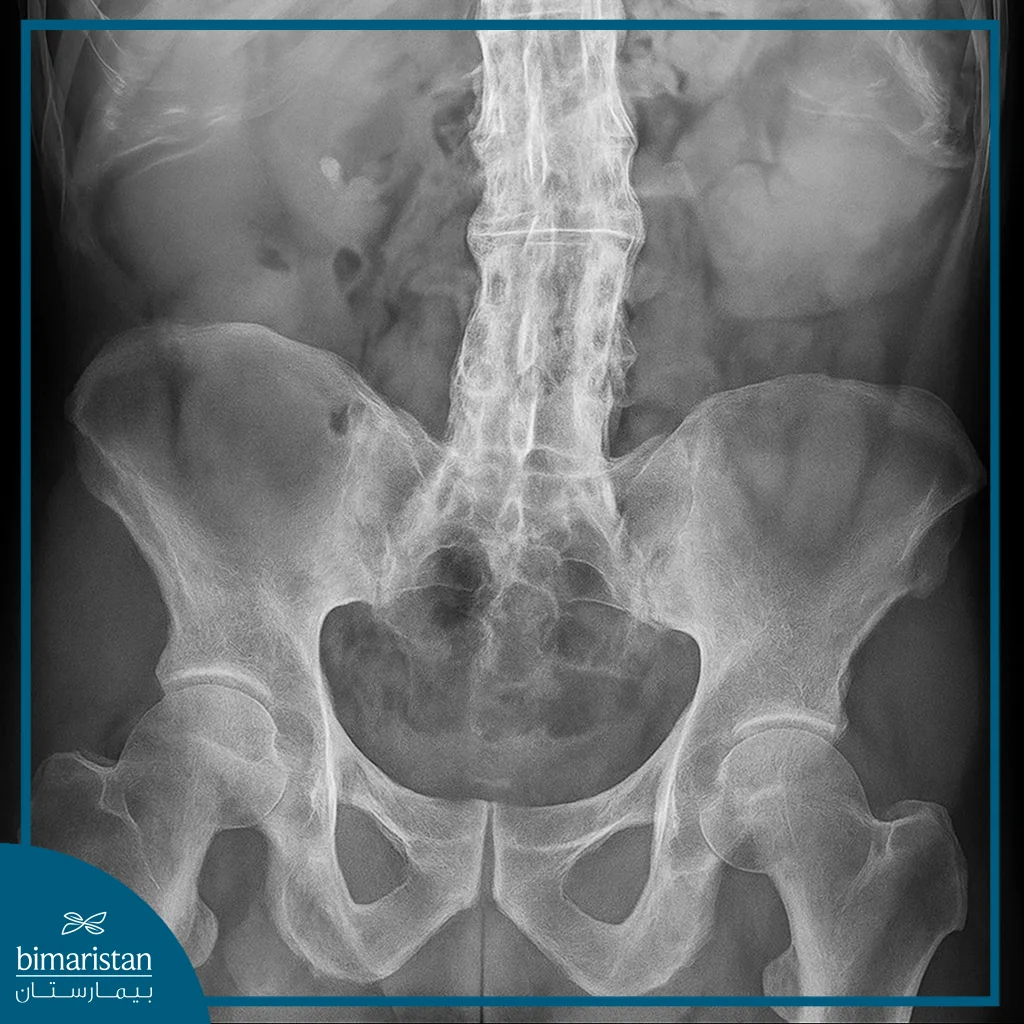
- Radiography: X-rays show changes in the sacroiliac joints and spine in the advanced stages, while MRIs help detect inflammation in its early stages before bony changes appear.
- Joint function and mobility tests: Used to measure the curvature and flexibility of the spine and assess the impact of the disease on daily movement.
Ankylosing spondylitis treatment in Turkey
Ankylosing spondylitis is managed by a rheumatologist, a specialist in autoimmune and joint diseases. The rheumatologist evaluates the patient’s condition and prescribes a tailored treatment plan. This plan may include medication, physical therapy, and in some cases, surgical intervention. These treatments can significantly improve the patient’s condition and help slow, or potentially halt, the progression of the disease. However, it is important to note that there is no definitive cure for ankylosing spondylitis.
Drug therapy for ankylosing spondylitis
The drug combinations prescribed by a rheumatologist to treat rheumatic diseases affecting the spine, such as ankylosing spondylitis, vary depending on the treatment line. If one treatment is not successful, we move on to the next, which is typically stronger, until the disease is contained and controlled. It’s important to note that the more powerful the medication used, the greater the potential side effects. Therefore, we do not start with strong drugs at the beginning of treatment; instead, we aim to use the most effective medication for the patient while minimizing cost and side effects. These medications include:
Painkillers and NSAIDs
Paracetamol and ibuprofen are the primary medications for managing ankylosing spondylitis; if they are not effective in relieving the patient’s pain, stronger medications are used.
Disease-modifying antirheumatic drugs (DMARDs)
These medications help reduce inflammation in the body and improve symptoms, especially in the hands and feet, and protect the joints from destruction, but they are considered less effective for symptoms related to the spine. The most important of these medications is methotrexate and sulfasalazine. When using these medications to treat ankylosing spondylitis, the patient must be monitored continuously to avoid side effects, and they are excellent for controlling pain and stiffness in the patient’s joints.
Biological therapy for ankylosing spondylitis
This category is the newest class of drugs for the treatment of ankylosing spondylitis, but their use should be cautious and under the supervision of a specialized doctor. These drugs aim to halt the autoimmune process responsible for the disease by targeting key components of this process, such as tumor necrosis factor (TNF) and interleukin 17. Among these, the most important drugs include:
- Etanercept
- Golemomab
- Adalimumab
- Secukinumab
- Citrolizumab pegol
Ankylosing spondylitis treatment with steroids
Steroid medications (such as corticosteroids) are medications used to treat attacks of ankylosing spondylitis, either injected into the inflamed joint or intramuscularly. There are also oral tablets and eye drops. We use steroid drops for ocular inflammation associated with rheumatoid spondylitis. Do not use this drug class for a long period of time due to its side effects, and like any other medication, contact your doctor immediately if you notice any side effects from treating ankylosing spondylitis.
Physical therapy for ankylosing spondylitis in Turkey
Physical therapy plays a pivotal role in the management of ankylosing spondylitis, aiming to relieve pain, maintain flexibility of the spine and joints, and improve the ability to perform daily activities. Along with medication under the supervision of a doctor, this type of therapy is an essential part of a comprehensive treatment plan:
- Training on correct posture: Teaching the patient how to sit, stand, and sleep in a way that minimizes pressure on the spine and affected joints.
- Daily stretches: Helps keep your spine and ligaments flexible and reduces joint stiffness, especially when you wake up in the morning.
- Muscular strengthening exercises: Targets the back, abdominal, and hip muscles to support the spine, improve posture, and reduce pain during movement.
- Hydrotherapy: Exercises in water help reduce joint load, facilitate movement, and significantly reduce pain.
- Heat and cold therapy: Applying warm compresses relieves pain and increases muscle flexibility, while cold compresses reduce inflammation and swelling, and are used for acute pain.

Ankylosing spondylitis treatment with surgery in Turkey
Most patients with ankylosing spondylitis do not require surgery, as most symptoms can be controlled with medication. Surgery is very useful for ankylosing spondylitis patients if one of the joints is damaged and requires replacement; the most important of which are hip joint replacement and knee joint replacement. Usually, we do not resort to spinal surgery except in special cases where intervention is essential to the patient’s life and improves their condition. Performing spinal surgery requires great expertise. Here, at Bimaristan Medical Center, the most skilled orthopedic surgeons in Turkey perform such specialized procedures.
In conclusion, ankylosing spondylitis is a chronic disease that mainly affects the spine and joints and needs continuous follow-up and a comprehensive treatment plan that combines medication, physical therapy, and lifestyle modifications. Early and regular treatment relieves pain, maintains spinal flexibility, and minimizes the development of curvatures or complications, enabling the patient to regain mobility, perform daily activities more efficiently, and significantly improve their quality of life.
Sources:
- VERSUS AVersus Arthritis. (n.d.). Ankylosing spondylitis. Versus Arthritis. Retrieved October 18, 2025
- National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS). (2023, May). Ankylosing spondylitis. National Institutes of Health.
- National Health Service (NHS). (2023, January 5). Ankylosing spondylitis.