Arrhythmia occurs when the heart no longer maintains a normal rhythm, becoming faster, slower, or irregular, and its severity can range from mild, symptom‑free episodes to dangerous conditions such as ventricular fibrillation. In more serious cases, advanced interventions are needed to manage these rhythm disorders and reduce the risk of complications, including the use of an implantable cardioverter‑defibrillator.
What is an Implantable Cardioverter‑Defibrillator (ICD)?
An Implantable Cardioverter-Defibrillator (ICD) is a small device implanted under the skin that continuously monitors the heartbeat and intervenes when a serious rhythm disturbance occurs. It differs from a conventional pacemaker in its ability to treat both bradycardia and tachycardia, making it an effective lifesaver in situations where there is a risk of sudden cardiac arrest.
Causes of arrhythmias
Normally, the heart’s electrical activity begins in a small node in the right atrium called the sinus node, which generates electrical signals that travel through the atrial walls, causing the atria to contract and pump blood into the ventricles. These signals then travel to the atrioventricular node, then through the His bundle and the Purkinje fibers, causing the ventricles to contract and pump blood to the body and lungs. This delicate process keeps the heart rhythm regular, often between 60 and 100 beats per minute in adults.
When there is an abnormality in the formation or transmission of this signal or in the heart muscle’s response to it, an irregular heart rhythm (arrhythmia) occurs, which may arise from multiple causes, including those related to the heart itself, such as:
- Heart valve disease, especially with high blood pressure
- Narrowed or blocked coronary arteries (coronary artery disease)
- Previous heart attacks
- Inflammation or weakness of the heart muscle
The cause can also be external, such as:
- Too much caffeine, alcohol, or nicotine
- Severe emotional reactions can affect your pulse rate
- The effect of certain medications or drugs
- Hyperthyroidism
These factors can lead to excessive bradycardia or tachycardia, and in some cases can cause serious disorders that require urgent intervention.
Arrhythmias symptoms
Symptoms vary depending on the type of disorder:
- Bradycardia: It is characterized by a heart rate below normal, which reduces blood flow to the body, especially the brain. The patient may feel dizzy or faint, experience general fatigue and weakness, and notice blurred vision due to low perfusion.
- Ventricular tachycardia: In this condition, the heart beats too fast and irregularly, reducing pumping efficiency. The patient experiences rapid palpitations, shortness of breath, and, sometimes, chest pain or pressure. Dizziness or even loss of consciousness may accompany this condition if blood flow is significantly reduced.
- Ventricular fibrillation: One of the most serious arrhythmias, this condition disrupts the heart’s ability to pump blood effectively by producing rapid, uncoordinated beats. This leads to rapid loss of consciousness, and without immediate defibrillation intervention, death can occur within minutes.
Diagnosing an arrhythmia
Sometimes, the patient’s symptoms, history, and clinical examination already raise suspicion for an arrhythmia. An electrocardiogram (ECG) is performed, which shows typical changes in each case. Long-term (24-hour) electrocardiograms are also recommended, as well as cardiac echocardiograms to assess the structure and function of the heart. Sometimes other screening methods are used, such as a stress test or an Electrophysiological study of the heart.
Arrhythmia treatment
The treatment plan depends on the type and severity of the arrhythmia, as well as the patient’s overall health status. Treatment options include the following:
- Drug therapy: Commonly used for mild to moderate arrhythmias, it includes antiarrhythmic medications that work to regulate the heart rate and improve its electrical stability, and the type of medication varies depending on the type and severity of the disorder.
- Catheter ablation: This is an interventional procedure that aims to identify and damage specific areas of the heart that cause irregular electrical signals, using electrical energy, heat, or cold. This treatment is especially used in cases of tachycardia that do not respond to medication.
- External defibrillation: Used in emergencies such as ventricular fibrillation or life-threatening ventricular tachycardia, electric shocks are delivered through the patient’s chest to quickly and effectively return the heart to its normal rhythm.
- Implantable cardioverter-defibrillator (ICD): This is a therapeutic and preventive option for cases that do not respond to previous treatments or carry a high risk of life-threatening arrhythmias.
How implantable cardioverter defibrillator (ICD) works and its types
An implantable cardioverter-defibrillator continuously monitors the heartbeat and automatically intervenes when serious rhythm disturbances occur. In case of bradycardia, the device delivers small electrical impulses to stimulate the heart muscle and ensure a regular beat. In the event of an excessively rapid or irregular rhythm, the device delivers stronger electrical shocks that quickly return the heart to a normal rhythm. The device can be programmed according to the patient’s specific condition and needs, and is powered by a long-life battery that ensures it lasts for years.
There are several types of ICDs, depending on how many chambers of the heart the device covers:
- Single-chamber: Contains a single electrode implanted in the right ventricle, suitable for some cases where only ventricular pacing is required.
- Bi-chamber: Contains two electrodes, one in the right atrium and the other in the right ventricle, which allows the synchronized contraction of the atria and ventricles to be regulated to improve the efficiency of blood pumping.
- Subcutaneous implantable cardioverter defibrillator (S-ICD): Implanted under the skin without the need to insert electrodes into the heart, this is a less invasive option for some patients who don’t need internal pacing.
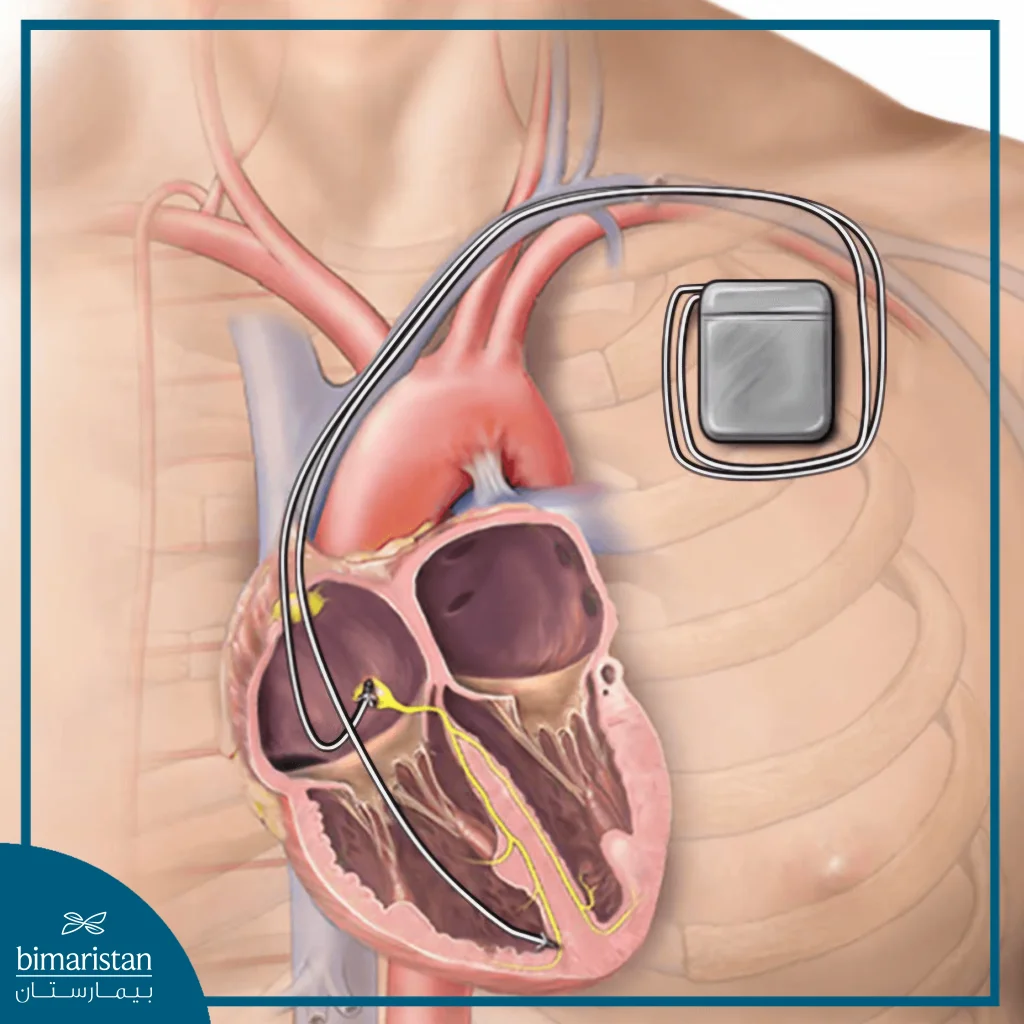
Implantable cardioverter‑defibrillator surgery
The process of implanting an ICD (implantable cardioverter-defibrillator) typically begins with a thorough evaluation of the patient’s overall condition. The medical team reviews the patient’s medications, particularly those that affect blood clotting, such as aspirin or warfarin. Patients may be asked to temporarily stop taking these medications to reduce the risk of bleeding during the surgery. Additionally, laboratory tests are conducted to ensure the patient is safe and fully prepared for the operation.
Local anesthesia is often used in the area under the clavicle, with intravenous sedatives to help the patient relax and reduce anxiety. In rare cases, general anesthesia may be used, especially when warranted.
The surgeon makes a small incision in the skin under the clavicle and then creates a pocket to place the device, protecting it and securely anchoring it under the skin. The electrodes are then inserted through the subclavian vein using a catheterization technique and carefully guided towards the heart under X-ray (fluoroscopy) guidance. An electrode is placed in the right ventricle, and if the device is a dual-chamber type, another electrode is added in the right atrium to ensure effective monitoring and regulation of the heartbeat.
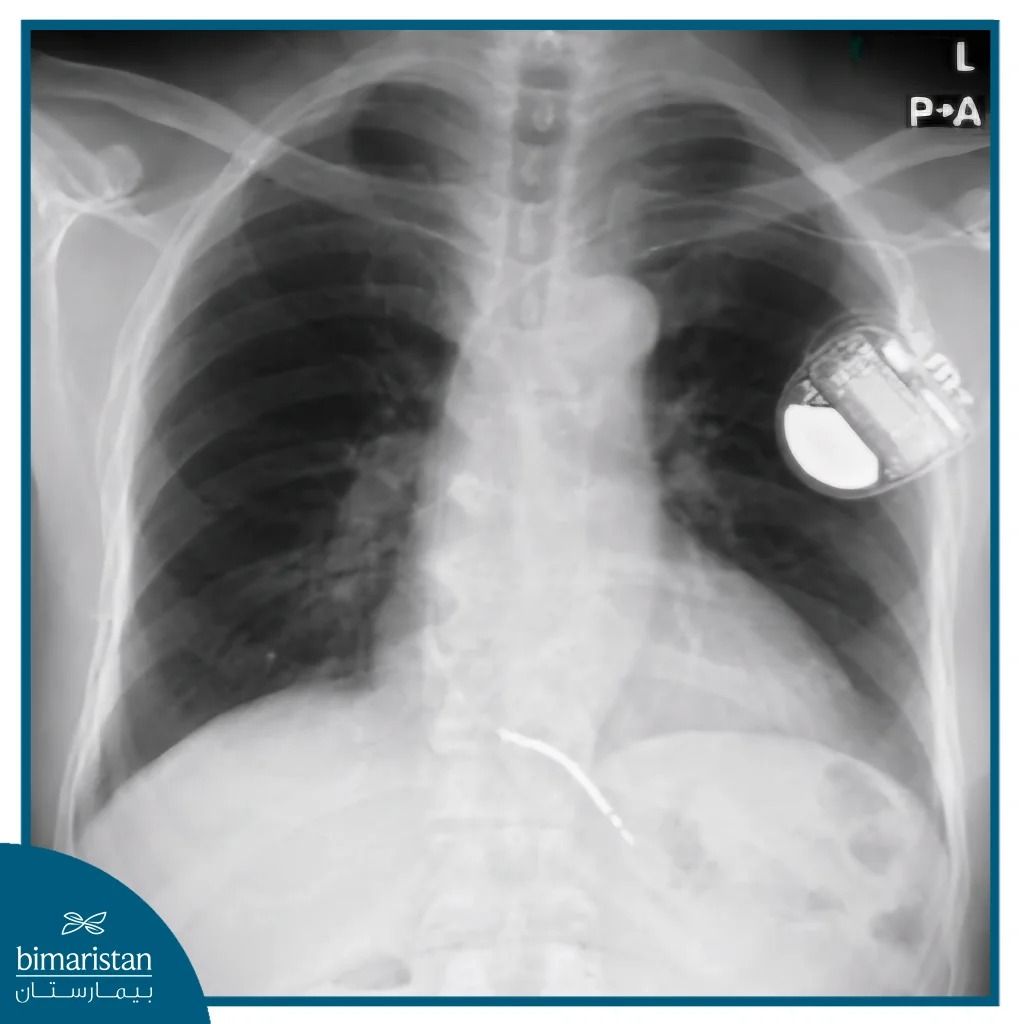
Once the electrodes are in place, they are connected to the defibrillator located inside the skin pocket. The medical team then tests the device’s functionality by triggering a temporary heart rhythm disturbance to ensure it can detect abnormal electrical signals and deliver the necessary electrical shocks to restore a normal rhythm. After verifying the device’s proper functioning, the incision is closed with fine sutures, and the device is programmed to the patient’s specific needs, allowing it to automatically monitor heart rhythm and intervene appropriately and effectively when needed.
Implantable cardioverter‑defibrillator complications
Although implantable cardioverter defibrillator (ICD) implantation is considered safe in most cases, it can be associated with some complications. There may be bleeding or swelling at the implantation site, or injury to nearby nerves that may cause temporary numbness or weakness. There is also a risk of injury to the heart muscle or blood vessels during electrode insertion. Additionally, complications may include air entering the space around the lung (pneumothorax) and fluid accumulation around the heart (pericardial effusion), both of which can temporarily affect heart function
Other complications may include infection at the device site or around the electrodes, which could require antibiotics or, in rare cases, removal of the device. Additionally, there is a possibility of blood clots forming in the veins where the electrodes were inserted, as well as technical issues such as electrode displacement or device malfunction. Despite these risks, the advantages of the device in preventing life-threatening arrhythmias significantly outweigh the potential for these complications.
Instructions after the implantation
On the first day after the implantable defibrillator is placed, the patient remains under close observation in the hospital to ensure the device is functioning properly and to monitor heart recovery. During this period, the pulse and activity of the device are monitored, and the wound area is cared for to prevent any infection. The patient is advised to rest, avoid violent movements, especially in the arm on the same side as the device, and avoid lifting weights or performing strenuous physical activity.
As the initial days unfold, the device evaluation is completed, and its settings are adjusted to suit the patient’s condition, and clear instructions are given before discharge from the hospital about activities that are allowed and temporarily prohibited, such as refraining from driving a car, being careful when swimming, or doing activities that may cause danger in the event of sudden fainting.
Life with an implantable cardioverter-defibrillator
After the initial recovery period, the patient can return to their daily life with some precautions. Stay away from sources of strong magnetic or electric fields, such as high-voltage systems, large electric motors, and electrical stimulation devices, unless the device is designed to withstand them. MRI may also be unsafe unless the device is compatible with it.
It is important to perform regular checks of the device and heart function, as settings may require adjustments, or the battery might need replacement after five to ten years. If you experience any unusual symptoms such as severe dizziness, frequent shocks from the device, or a change in its position, please consult your doctor immediately. Adhering to these instructions will help the patient adapt to the device and enjoy a normal and active life.
In conclusion, implantable cardioverter‑defibrillator are an important medical solution for those suffering from serious heart rhythm disorders, as they help regulate the heartbeat and preserve life. Successful use of this device depends on adherence to the doctor’s instructions and regular follow-up, as well as adapting to any changes that may occur after implantation. With the necessary care, the patient can lead a normal, active life, taking advantage of modern technology to improve their quality of life.
Sources:
- American Heart Association. (n.d.). Implantable cardioverter defibrillator (ICD).
- British Heart Foundation. (2025, May 6). Implantable cardioverter defibrillator (ICD).