Atrial fibrillation (AF) is one of the most common heart rhythm disorders, caused by an imbalance in the electrical signals that regulate the heartbeat, resulting in a rapid or irregular heartbeat. With advances in therapeutic techniques, atrial fibrillation catheter ablation has become an effective treatment option, as it targets the electrical foci responsible for the disorder and aims to restore a regular rhythm.
What is atrial fibrillation?
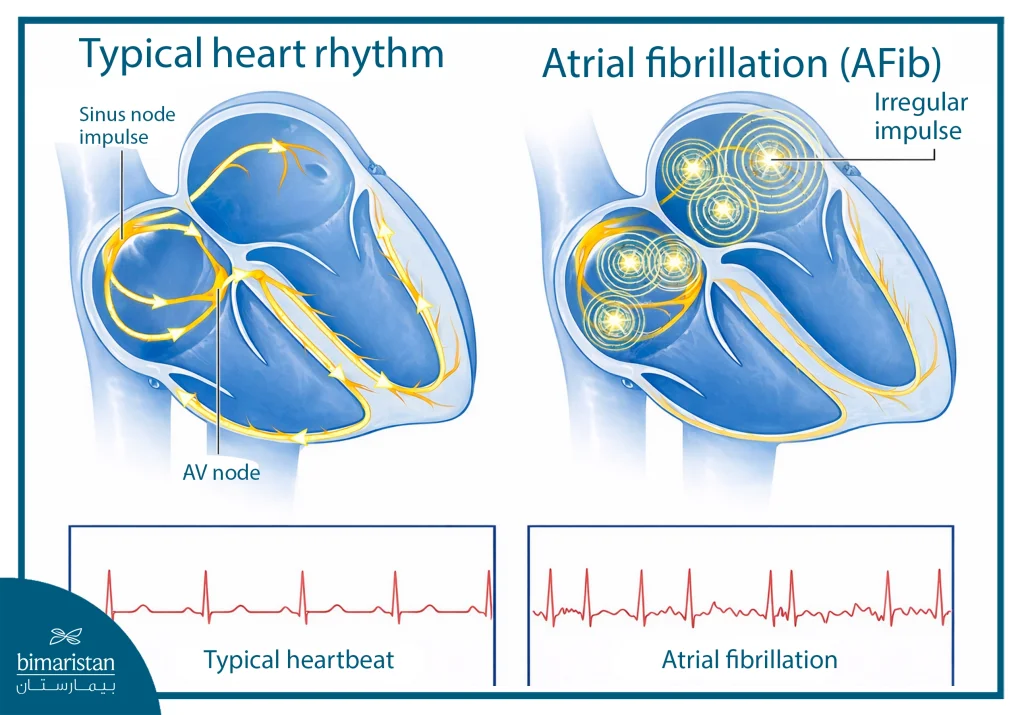
Atrial fibrillation, one of the most common heart rhythm disorders, occurs when the electrical signals in the atria are disrupted and lose their normal rhythm. Instead of the signal traveling in a coordinated fashion, multiple signals fire simultaneously, resulting in a rapid, chaotic contraction of the heart’s upper chambers that is not synchronized with the ventricles.
As a result, blood is not pumped efficiently, and the patient may experience rapid or irregular palpitations, shortness of breath, or dizziness, while some people may not notice any symptoms. Atrial fibrillation episodes can be intermittent or continuous, and while not life-threatening in itself, they increase the risk of clot formation, stroke, or heart failure, requiring proper evaluation and treatment.
With these potential risks, it is important to understand the treatment options available to control atrial fibrillation and minimize its complications.
Types of atrial fibrillation and their impact on the ablation decision
Atrial fibrillation is classified into several types based on the duration and progression of the episode, and this classification is important when assessing the appropriateness of catheter ablation for each patient. Types include:
- Paroxysmal atrial fibrillation: Occurs as intermittent episodes that stop spontaneously over a short period of time without permanent intervention.
- Persistent atrial fibrillation: Lasts longer and requires medical intervention to normalize the rhythm.
- Long-term or chronic atrial fibrillation: It lasts for extended periods of time and may have been present for years.
Identifying the type of AF helps guide the treatment decision, as paroxysmal and new-onset cases tend to respond better to the procedure than prolonged or chronic cases, making categorization an essential step in treatment planning.
What is atrial fibrillation catheter ablation?
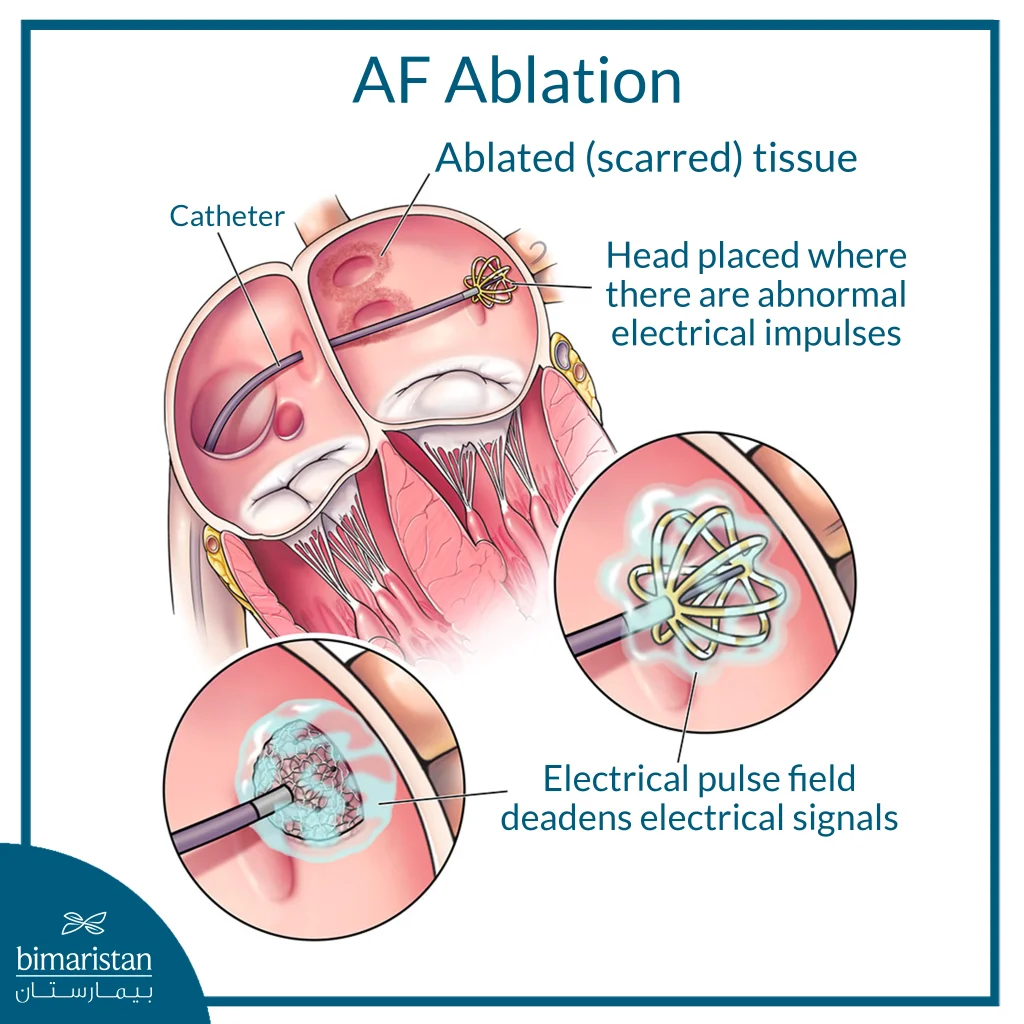
Catheter ablation of atrial fibrillation is a therapeutic procedure used to control the arrhythmia by stopping the abnormal electrical signals that cause it. This treatment involves creating small areas of scar tissue within the heart using heat (thermal) or cold (cryogenic) energy, thereby blocking the transmission of abnormal signals and restoring the heart’s rhythm. This procedure is minimally invasive compared to surgery, and is often used when medications are not enough, and in some cases may be chosen as an early treatment option.
Which patients are suitable for catheter ablation of atrial fibrillation?
Catheter ablation of atrial fibrillation is primarily considered in patients with troublesome symptoms such as palpitations or shortness of breath, or in those whose medications have not achieved adequate rhythm control, and may be used to maintain a normal rhythm and reduce the risk of long-term complications such as heart failure and stroke, although it may not eliminate the need for blood thinners.
The procedure is usually more effective in patients with relatively recent paroxysmal atrial fibrillation, especially if there are no obvious structural heart abnormalities. Older age, longer duration of atrial fibrillation, left atrial enlargement, impaired left ventricular function, and comorbidities such as obesity, hypertension, and sleep apnea may be associated with an increased risk of arrhythmia recurrence after the procedure, but are not absolute contraindications.
The presence of a thrombus in the left atrium is a contraindication to ablation; each case should be evaluated individually to weigh the expected benefit against the potential risks, and treatment options should be discussed with your physician.
Preparation before atrial fibrillation catheter ablation
Catheter ablation of atrial fibrillation is performed in the hospital and requires advanced preparation to ensure the safety of the procedure. Fasting instructions are explained to the patient by the doctor, and the patient is often asked to abstain from food and drink for several hours before the procedure, usually after midnight. It is also important to follow the doctor’s instructions regarding medications, especially blood thinners, and not to discontinue any medication except under direct guidance.
Some pre-operative tests may be required to assess the condition of the heart, such as an electrocardiogram, echocardiogram to assess structure and function, and sometimes additional tests such as a stress test, CT scan, or MRI to determine the exact anatomy of the heart, along with necessary blood tests.
On the day of the procedure, an intravenous line is placed to administer medications. The patient is given sedatives or anesthesia, depending on their health condition and the type of disorder; anesthesia may be light or general as needed. It is also advisable to arrange transportation home after the procedure and to wear comfortable clothes.
Catheter-based atrial fibrillation cauterization procedure
Catheter-based atrial fibrillation cauterization is performed in the hospital by a doctor who specializes in arrhythmias and involves inserting thin catheters into the heart to locate the source of the abnormal electrical signals and then isolating them with a guided scar. The procedure usually takes between two and six hours, depending on the complexity:
- Preparing the entry site: The area, usually in the groin, is shaved, cleaned, and sterilized, then anesthetized locally, and the patient is given sedatives or general anesthesia, depending on their condition, to remain relaxed or asleep during the procedure.
- Insertion of catheters: The doctor inserts a small sheath into a blood vessel and passes thin electrode catheters through it, which are guided to the heart using X-rays.
- Electrocardiography: Advanced mapping systems are used to map cardiac signals and accurately identify the areas responsible for the disorder.
- Ablation procedure: After localizing the abnormality, RF thermal energy or cryogenic energy is used to create small scars that isolate the tissue causing the fibrillation and prevent the transmission of abnormal signals.
- Termination of the procedure: After completion, the catheters are withdrawn, and the entry site is closed with pressure or special closures to prevent bleeding.
In some special cases, the treatment plan may require additional procedures depending on the type of ablation used.
What is the difference between thermal ablation and cryoablation?
There are two main types of catheter ablation of atrial fibrillation, depending on the energy source used to create scar tissue within the heart:
- Radiofrequency ablation: Uses thermal energy to heat the target tissue and create scars that prevent the transmission of abnormal electrical signals.
- Cryoablation: Uses cold energy to freeze the tissue causing the disorder, creating similar scars at the electrode site.
Both methods achieve the common goal of stopping the abnormal signals and restoring a regular pulse, and studies show that their effectiveness and safety are comparable in many cases. Some of the technical details may differ. Thermofrequency is performed pointwise by heating the targeted areas, whereas freezing can produce more uniform scar formation around the lung veins in some cases, which may minimize the need for multiple adjustments.
The choice between these two types often depends on the doctor’s assessment of the patient’s condition, the location of the heart defect, and the medical team’s experience, with the understanding that each method has potential advantages that can be discussed with the caregiver.
Risks and complications of catheter-based atrial fibrillation cauterization
Catheter ablation of atrial fibrillation is a relatively safe procedure, with complications uncommon, especially when performed in experienced centers. However, there are potential risks that should be discussed in advance with your doctor. Possible complications include
- Bleeding, inflammation, or pain at the catheter insertion site, or damage to blood vessels
- Damage to heart tissue or valves may rarely require a permanent pacemaker
- Forming clots that can lead to stroke or bleeding around the heart
- Pulmonary vein stenosis or new rhythm disturbances after the procedure
- Rare complications such as esophageal or nerve damage, or effects associated with the use of radiation or contrast material
Some serious risks are estimated to be low: the risk of stroke is about 1 in 500, the risk of bleeding around the heart is about 1 in 200, and the risk of death is rare at about 1 in 1000.
Complications are more likely to occur in the elderly or those with heart disease or comorbid conditions, and some patients may have a recurrence of fibrillation episodes months or years later, sometimes requiring a repeat procedure.
Catheter ablation of atrial fibrillation and follow-up
After the procedure is completed, the patient is taken to a recovery room where vital signs are monitored for several hours. Some patients may leave the hospital the same day, while others may need to stay overnight depending on their condition.
The patient may experience mild pain, chest tightness, or a slight bruise at the insertion site, which often resolves within days. Most patients are able to return to their daily activities within a few days, avoiding heavy physical exertion, short-term lifting, and driving for the first 48 hours. Medications will be reviewed by the doctor after the procedure, and blood thinners may continue to be used to prevent clots, depending on individual assessment, as ablation has not been shown to completely eliminate the risk of stroke. Follow-up appointments and instructions regarding catheter site care and physical activity should be adhered to.
It is important to know that the final results may take several weeks to fully appear, and during the first few months, temporary arrhythmias may occur as the heart tissue heals, which may be normal at this stage.
Catheter ablation of atrial fibrillation: cost and influencing factors
The approximate cost of catheter ablation of atrial fibrillation in Turkey ranges from $4,000 to $8,000 and may vary depending on the case and the technique used. The cost is usually influenced by the following factors:
- Type of ablation used (thermal or cryoablation)
- Type of atrial fibrillation and complexity of the procedure
- Duration of the procedure and the need for advanced EEG techniques
- Experience of the medical team and the hospital where the procedure is performed
- Length of hospitalization and ancillary services
- Pre-operative diagnostic tests, medications, and post-operative follow-up
It is advisable to get an individualized assessment from the medical center to get an accurate quote for each patient’s health condition.
In conclusion, catheter ablation of atrial fibrillation is an advanced treatment option for arrhythmia control in patients who do not respond adequately to medications or have symptoms that affect their quality of life. The success of the procedure depends on careful evaluation of each case and appropriate patient selection, recognizing that ongoing follow-up may still be necessary and that some patients may need to repeat the procedure to achieve the best possible outcome. The decision to treat should be made after a thorough discussion with your physician to weigh the benefits and risks and develop an individualized treatment plan.
Sources:
- Johns Hopkins Medicine. (n.d.). Atrial fibrillation ablation.
- European Society of Cardiology. (n.d.). Catheter ablation for the management of atrial fibrillation: A treatment strategy.