Carotid artery stenosis is a major cause of ischemic stroke, resulting from the buildup of atherosclerotic plaque within the carotid artery wall that restricts blood flow to the brain. With advances in vascular interventional techniques, carotid angioplasty and stenting has become an effective, minimally invasive treatment used to widen the narrowed segment and restore cerebral perfusion. For patients at higher risk from conventional surgery, this procedure offers a safer alternative that enhances quality of life and lowers the likelihood of recurrent strokes when performed at the appropriate time and in carefully selected individuals.
The pathogenesis of carotid atherosclerosis
Carotid artery disease is caused by the accumulation of cholesterol in the arterial walls, especially at bifurcations such as the origins of the internal and external carotid arteries. Over time, this buildup leads to the formation of atheromatous (hardened) plaques within the arterial wall, composed of fatty substances and muscle fibers. As these plaques grow larger, they may narrow the arterial lumen and impede blood flow to the brain, and their surfaces may become rough or irregular, increasing the likelihood of blood clot formation. If the plaque ruptures, it can release a thrombus (clot) that can block a cerebral artery and lead to a stroke or transient ischemic attack, even if the narrowing isn’t too severe.
When cerebral perfusion is impaired, the brain relies on collateral circulation, an alternative blood flow through branching vessels such as the arterial circle of Willis. However, the body’s ability to compensate is influenced by several factors, including the size and shape of the plaque, the duration of ischemia, the nature of the clot (embolus), as well as the efficiency of cerebral vasodilation (vascular reserve).
All of these factors determine the severity of neurological symptoms, which can range from mild and temporary symptoms (such as blurred vision or temporary muscle weakness) to severe and permanent complications such as a major stroke.
The relationship between carotid artery stenosis and stroke
Stroke is the third leading cause of death in Western countries and can cause permanent disability. Carotid artery atherosclerosis is directly associated with 20-30% of stroke cases, so thromboembolism of cerebral vessels caused by carotid atherosclerosis (which causes stenosis) is an important health issue.
The incidence of stroke increases with age. In 2014, about 2.8% of the general population over the age of 18 had a history of stroke, and about 795,000 people had a new or recurrent stroke in each subsequent year. There were 6.5 million stroke deaths worldwide, and 3% of males and 2% of females were disabled by stroke in 2014.
Several risk factors are clearly associated with both carotid atherosclerosis and stroke, and it is very important to keep these factors in mind as a way to reduce the risk of recurrent stroke after carotid atherosclerotic plaque removal.
Common risk factors associated with carotid atherosclerosis and stroke
- Modifiable factors: High blood pressure, hyperlipidemia, smoking, diabetes, and obesity.
- Non-modifiable factors: Age >80 years, males, presence of coronary artery disease, presence of congestive heart failure, presence of family history.
Detecting and diagnosing carotid artery stenosis
Carotid artery stenosis may present with symptoms such as a transient ischemic attack (TIA) or stroke, or it may be asymptomatic. A TIA is a temporary neurological event that lasts from seconds to 24 hours with no lasting effect, but it may be a precursor to a subsequent stroke.
Stenosis can be detected during a routine examination by hearing a murmur or by an ultrasound scan, especially in high-risk patients such as those with coronary artery disease and hypertension. The presence of a murmur requires additional tests for an accurate diagnosis, and not all plaques carry the same risk of cerebral embolism, so it is important to accurately identify the cause to ensure proper treatment.
Symptoms and clinical signs of carotid artery stenosis
The main symptoms of carotid artery stenosis include:
- Weak facial and limb muscles
- Vision disorders and headaches
- Speech disorders
Signs suggestive of carotid artery stenosis include a very severe murmur at the origin of the internal carotid artery, an increase in the size and pulsation of the corresponding superficial temporal artery, and changes on retinal examination.
When is carotid artery stenosis treated?
Patients with carotid artery stenosis of more than 60% have a risk of ischemic stroke of more than 10% per year, so it is recommended to treat this stenosis by reopening the stenosis (revascularization) to reduce the risk of cerebral embolism. The effect of revascularization is limited in severe asymptomatic carotid artery stenosis because the stroke recurrence rate is only about 2% per year, so medical treatment and follow-up with minimally invasive surgery are preferred in patients with carotid artery stenosis greater than 80% with no symptoms.
In addition, revascularization therapy provides maximal benefits for newly symptomatic patients if performed within 14 days, but carotid revascularization therapy may be considered even in asymptomatic patients with less severe stenosis in the following cases: Presence of occlusion in the contralateral carotid artery, rapid progression of stenosis during clinical follow-up, presence of cerebral infarction on brain imaging that was not symptomatic, and presence of vulnerable plaques on ultrasound imaging.
Things to consider when choosing a treatment for carotid artery stenosis
Carotid angioplasty and stenting is preferred in patients who would have difficulty undergoing carotid endarterectomy or are at high risk of complications during surgery. Conversely, carotid endarterectomy is preferred if the lesion site is difficult to access via catheter-based endovascular access. It is advantageous to choose carotid endarterectomy when stent implantation is difficult or significant complications are expected, including type III aortic arch, bovine arch, severe proximal curvature, severe lesion calcification, femoral arterial occlusion, or severe aortic curvature with calcification.
Carotid angioplasty and stenting
Carotid angioplasty and stenting techniques have continued to evolve into an effective alternative treatment for carotid artery stenosis, especially for patients with high surgical risk. Newer devices that protect brain tissue from emboli have improved treatment safety, and studies have shown that carotid angioplasty and stenting may be an equivalent or better alternative to endarterectomy in some cases.
The timing of the intervention depends on the patient’s condition. It is advisable to delay the procedure for at least 4 weeks after a stroke to avoid bleeding, except in emergency cases. Carotid angioplasty and stenting is often performed when carotid endarterectomy is technically difficult, as in patients with difficult neck anatomy, recurrent stenosis after carotid endarterectomy, or a history of radiation therapy in the neck region. Stenoses that are either high (above the level of the mandible) or low (below the clavicle) are more amenable to carotid angioplasty and stenting than carotid endarterectomy.
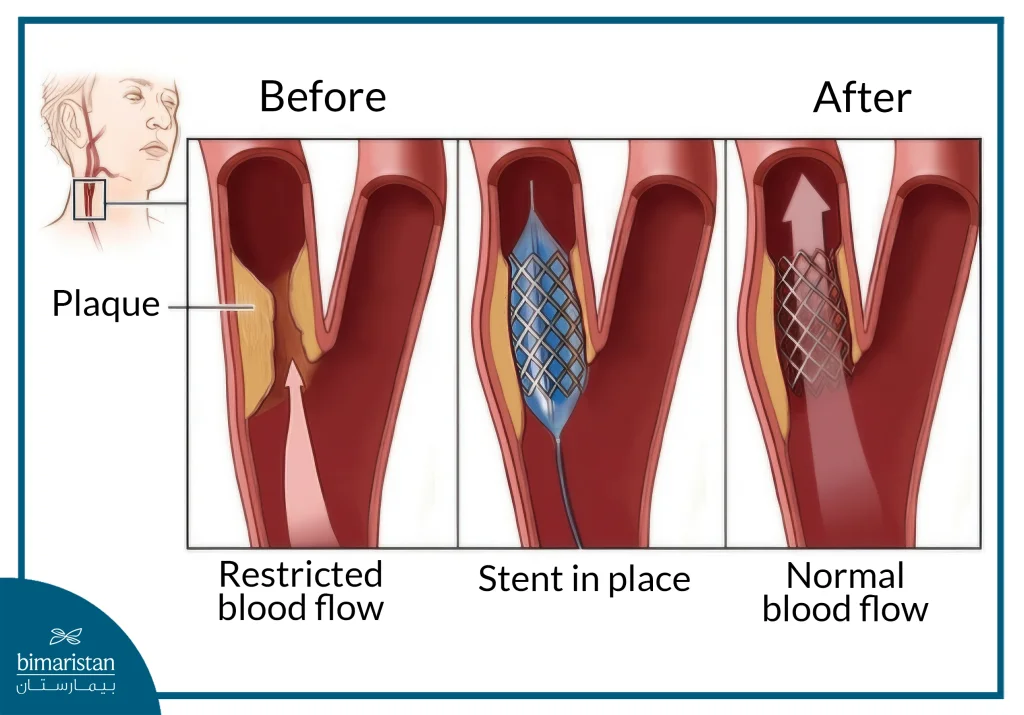
How does carotid angioplasty and stenting work?
Preparation for carotid angioplasty and stenting begins with pharmacologic therapy (such as aspirin and clopidogrel), which may vary based on the treating physician’s judgment and the patient’s clinical condition.
The patient is taken to the catheter angiography department, where the femoral artery is accessed. A guiding catheter is then advanced to the affected carotid artery. The procedure is performed under either conscious sedation or general anesthesia. Following this, contrast angiography is used to evaluate the degree of stenosis in the carotid artery.
To prevent embolic stroke, one of the main procedural complications of carotid angioplasty and stenting, three approaches are used for deploying an embolic protection device. These include distal embolic protection, proximal embolic protection, and distal filtration, which is the most commonly used method.
A brain protection device (usually a filter) is passed across the stenosis and positioned distal to it to capture any particles that may come out of the stenosis area during the procedure, after which a self-expanding stent is placed in the area of the carotid artery stenosis. Your doctor may perform balloon dilation before and after the stent is placed. At the end of the procedure, the filter is removed. The efficiency of blood flow through the stent and the absence of intracerebral embolization are confirmed by contrast angiography. The duration of the carotid artery angioplasty and stenting procedure is usually 30-60 minutes.
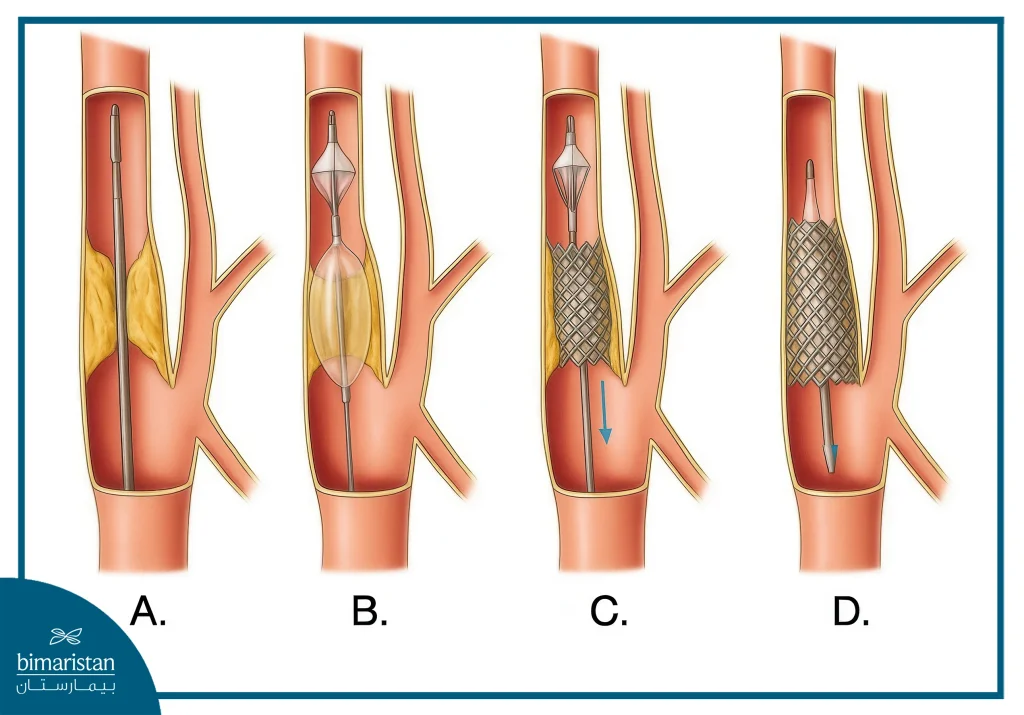
Heart rate and blood pressure are carefully monitored during carotid angioplasty and stenting, atropine is administered to avoid or relieve bradycardia, and severe hypotension is treated with intravenous infusions and small doses of vasoconstrictors (dopamine or noradrenaline).
All patients after carotid angioplasty and stenting are monitored neurologically and hemodynamically in the ICU for at least 12 hours to check their neurological status and maintain a normal heart rate and blood pressure. The patient is discharged after 48 hours, and all patients follow dual antiplatelet therapy, lipid-lowering therapy, and hypertension prophylaxis.
In cases of severe carotid artery stenosis (80%), pre‑dilation with a balloon (3–5 mm) is performed. After dilation, a self‑expanding stent is placed at the site of stenosis, followed by contrast angiography. If a residual stenosis of about 30% is observed, post‑dilation with a larger balloon (5–7 mm) is carried out.
Surgeons can use various types of stents during carotid angioplasty and stenting. In cases of stenosis involving the proximal segment of the common carotid artery, a balloon‑expandable stent is preferred to ensure accurate placement. These stents are also useful for lesions at the skull base or within the petrous segment of the carotid artery. On the other hand, self‑expanding stents are recommended over balloon‑expandable ones for the more common lesion sites at the carotid bifurcation or the proximal internal carotid artery.
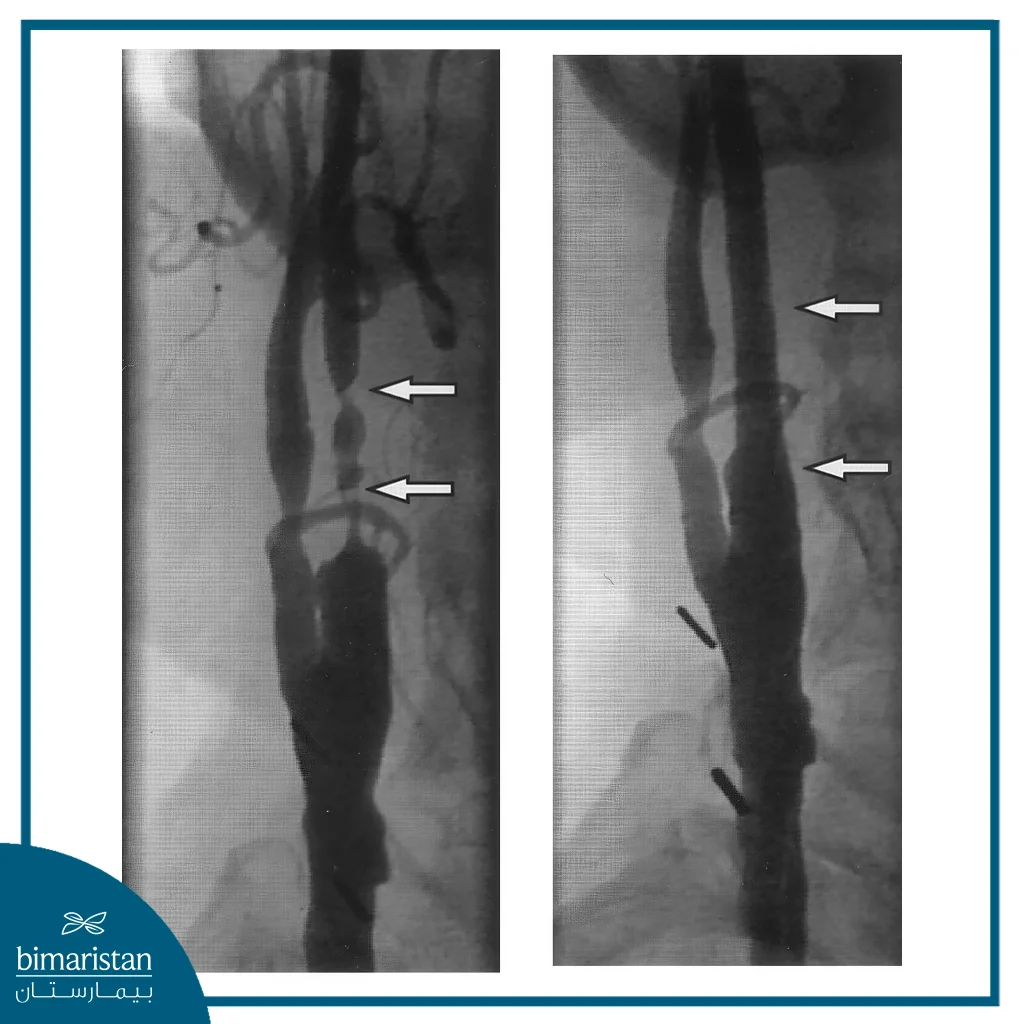
Patient care during carotid artery angioplasty and stenting
Carotid artery disease is not only a risk factor for stroke, but is also indicative of systemic vascular disease, especially ischemic heart disease. Therefore, evaluation prior to angioplasty and stenting includes an electrocardiogram and functional clinical assessment to detect any associated cardiac issues.
During the procedure, activated clotting time should be maintained above 250 seconds with heparin administration, and coronary angiography is recommended, as more than half of patients have underlying coronary artery disease. A sudden drop in blood pressure or heart rate after carotid sinus stimulation is usually transient and does not require specific treatment unless hypotension persists for a prolonged period or systolic blood pressure falls below 80 mmHg and is accompanied by symptoms.
Carotid angioplasty and stenting complications
Although carotid angioplasty and stenting is an advanced minimally invasive treatment option unrelated to open surgery, it can also have complications, some of which can occur during the procedure and some of which can occur a week later. Evaluating these complications is important to prevent worsening of the injury, and patients and their families should be educated about the signs and symptoms of these complications.
The incidence of medical complications after carotid angioplasty and stenting is less than 10%, and complications are associated with the presence of hypertension, coronary artery disease, diabetes mellitus, and renal insufficiency. Preoperative evaluation should focus on identifying these comorbidities and optimizing modifiable risk factors when possible.
Complications associated with carotid angioplasty and stenting include: Cerebral infarction, cerebral hemorrhage, or hyperperfusion syndrome, stent insertion site-related complications, embolic prophylactic device-related complications, systemic complications, and localized complications at the femoral puncture site.
In conclusion, carotid angioplasty and stenting is an effective and safe option for stroke prevention in patients with carotid artery stenosis who are not suitable for conventional surgical intervention. With advances in technology and medical expertise, the procedure offers encouraging results with fewer complications and faster recovery.
Sources:
- Erickson K.M., Cole D.J. Carotid artery disease: stenting vs endarterectomy. British Journal of Anaesthesia 2010;105: 34-49.
- Oran N.T, Oran I. Carotid Angioplasty and Stenting in Carotid Artery Stenosis: Neuroscience Nursing Implications. 2010; 42(1): 3-11.
- Park J.H, Lee J.H. Carotid Artery Stenting. Korean Circulation Journal 2018;48(2):1-17.