Atrial septal defect (ASD) is a congenital heart condition that can remain unnoticed for long periods, especially when early symptoms are mild or absent. Over time, this defect may affect the heart’s efficiency if it is not accurately diagnosed and monitored. Medical advancements have introduced modern treatment options, most notably catheter closure, which allows many cases to be treated in a less invasive and safer manner, leading to growing demand for this procedure in Turkey.
What is an atrial septal defect?
Atrial septal defect (ASD) is a congenital heart defect in which a person is born with an abnormal opening in the wall that separates the two upper chambers of the heart, the atria. This defect leads to abnormal blood flow, in which a portion of oxygen-rich blood flows from the left atrium to the right atrium rather than to the rest of the body. As a result, blood flow to the lungs increases, which may affect the function of the heart and lungs over time.
This defect may be small and cause no significant issues, and may be discovered accidentally or arise spontaneously in the early stages of life; alternatively, it may be large and persist for a long time, requiring evaluation and treatment to avoid complications.
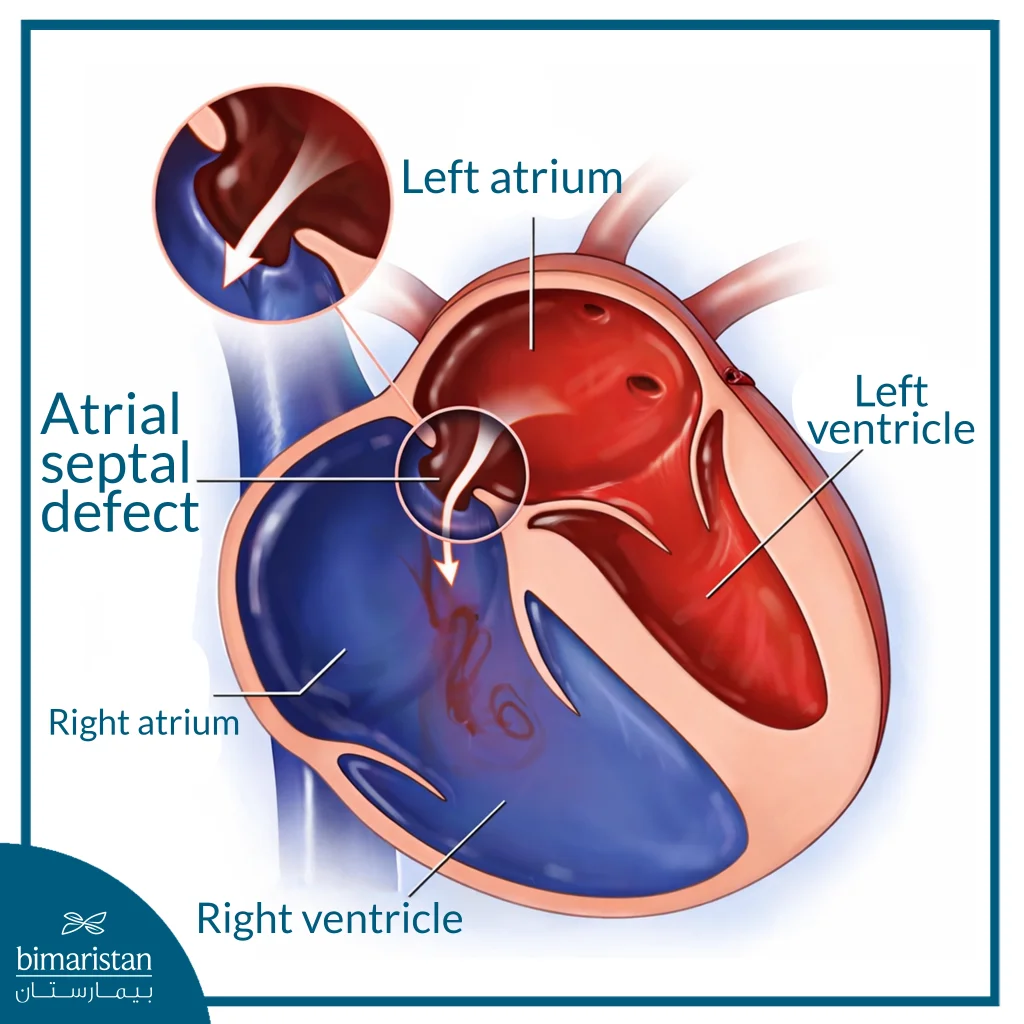
Types of atrial septal defect
Depending on the location of the opening in the atrial septum and the nature of the accompanying structural changes, the types of atrial septal defect differ. This categorization helps determine the appropriate follow-up and treatment options for each case.
Secundum atrial septal defect (Secundum ASD)
This is the most common type of atrial septal defect, located in the middle part of the atrial septum that separates the atria. It accounts for the majority of cases and is often amenable to non-surgical treatment in many patients.
Primary atrial septal defect (Primum ASD)
This type occurs at the bottom of the atrial septum, near the valves that separate the atria and ventricles. It may be associated with other congenital heart defects, such as valve abnormalities or additional cardiac structural abnormalities.
Sinus venosus atrial septal defect (Sinus Venosus ASD)
This is a rare type, typically located at the top or back of the atrial septum, and is often associated with other congenital changes in the heart’s structure or in the large blood vessels that return blood to the heart.
Coronary sinus atrial septal defect (Coronary Sinus ASD)
This is the rarest type of atrial septal defect and is caused by the absence or incomplete development of the wall between the coronary sinus and the left atrium. The coronary sinus is part of the venous system that drains blood from the heart muscle and is often associated with more complex congenital heart defects.
Atrial septal defect symptoms
A child with an atrial septal defect (ASD) may be born without any obvious symptoms, and signs of the condition might not emerge until later in life. Symptoms depend primarily on the size and location of the defect and on its effects on the heart and lungs; small defects may not cause significant issues, whereas symptoms are more pronounced in larger or untreated defects.
Symptoms in children
Most children with atrial septal defect (ASD), especially in mild cases, appear healthy and develop normally. However, some children may have symptoms that include:
- poor appetite
- Delayed growth or underweight for age
- Extreme fatigue or unusual exhaustion
- Difficulty or shortness of breath
- Frequent respiratory infections or pulmonary infections
Symptoms in adults
Adults with atrial septal defect may not experience symptoms until later in life, often after the defect has begun to affect cardiac and pulmonary function. Possible symptoms include:
- Feeling tired and fatigued
- Shortness of breath during physical activity
- Heart palpitations or the sensation of a fast or irregular heartbeat
- Swollen limbs or abdominal area
- Blue discoloration of the skin in advanced cases
Why might symptoms be mild or delayed in onset?
Symptoms are often mild or absent when the atrial septal defect is small and does not place excessive pressure on the heart or lungs. Over time, as abnormal blood flow persists, the effects of the defect may gradually become apparent, which explains why some patients do not present with symptoms until adulthood.
When does an atrial septal defect become dangerous?
A small atrial septal defect usually does not cause a major impact on the body, but larger or untreated defects can become serious over time. Excessive blood flow strains the right side of the heart, as it must pump more blood to the lungs, which can cause the right heart to enlarge and gradually decrease its efficiency. In the long term, this can lead to heart failure.
A large atrial septal defect also increases the risk of heart rhythm disorders, especially in adults, such as atrial fibrillation or atrial flutter. As individuals age, the risk of forming blood clots that can travel to the brain and lead to stroke may increase. In addition, constant pressure on the pulmonary blood vessels can lead to pulmonary artery hypertension, a serious complication that affects both the heart and the lungs. In advanced cases, you may develop what is known as Eisenmenger’s syndrome, a condition caused by severely elevated pulmonary blood pressure and altered blood flow within the heart.
How is an atrial septal defect diagnosed?
An atrial septal defect may be detected before birth or in early childhood, but smaller defects may not be detected until later in life. In some cases, the doctor may suspect the defect during clinical examination when an abnormal heart murmur is heard on auscultation, but the absence of this sign does not rule out the defect. Diagnosis is primarily based on a series of tests that evaluate the structure and function of the heart.
Tests used to diagnose atrial septal defect include the following:
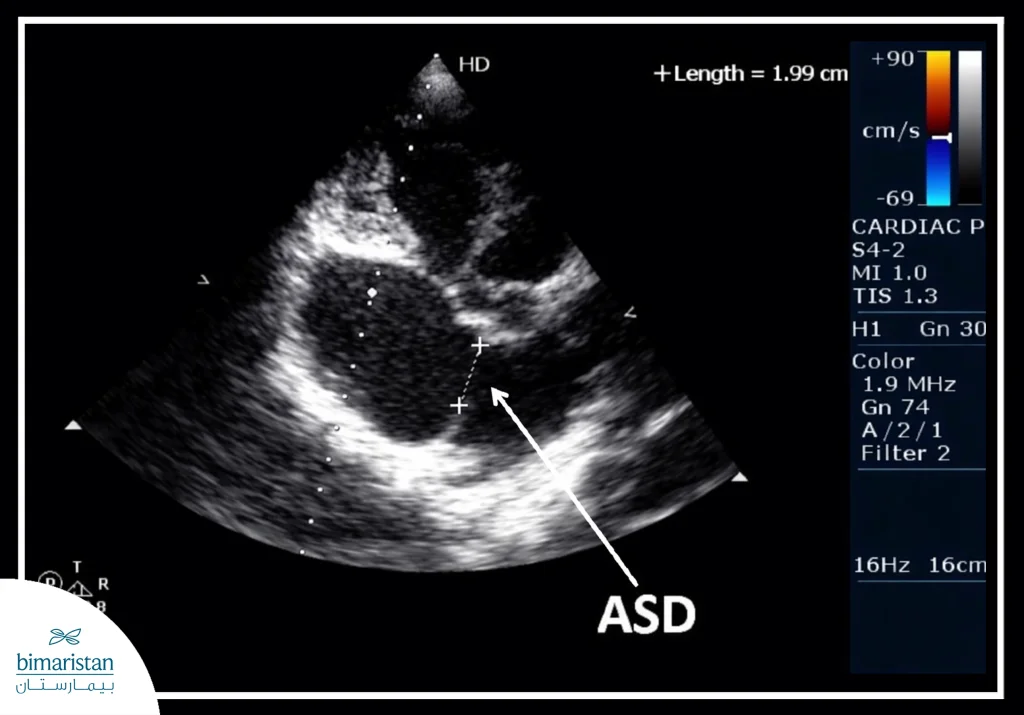
- Echocardiography: It shows the chambers and valves of the heart, assesses blood flow within the heart, and detects abnormal shunting between the atria.
- Transthoracic echocardiography (TTE): Used to evaluate the effect of the defect on the heart and lungs, including left-to-right atrial shunting.
- Transesophageal echocardiography (TEE): Helps to more accurately determine the size, shape, and location of the defect, as well as evaluate the heart valves.
- Electrocardiogram (ECG): Records the electrical activity of the heart and may reveal abnormal heart rhythms.
- Chest X-ray: May show enlargement of the right side of the heart or changes in the pulmonary vasculature.
- Cardiac magnetic resonance imaging (MRI) or computed tomography (CT): Used in cases where other tests do not give enough information, especially in uncommon types or when there are concomitant heart defects.
When does an atrial septal defect need treatment?
Not all cases require immediate therapeutic intervention, as the decision to treat is based on a thorough medical evaluation that balances the characteristics of the defect with the patient’s overall condition. The size of the hole and its functional impact on the heart are considered, as is evidence of increased cardiac load or changes in the function of the heart chambers. Additionally, the patient’s age, overall health status, and ability to tolerate the procedure are significant factors in this decision. In cases where the cardiac evaluation indicates that the defect may affect future cardiac function or increase the risk of complications, timely therapeutic intervention is recommended, even if symptoms are limited or absent.
Atrial septal defect treatment methods
Not all cases of atrial septal defects need direct treatment. Some small defects may only require regular medical check-ups without any intervention, particularly if they are asymptomatic and do not impact heart function. However, when the defect is moderate or large, or when it affects the cardiac function or poses a risk of future complications, therapeutic intervention is necessary.
Drug therapy
Medications are not used to close the atrial septal defect, but may be prescribed to help control some symptoms or reduce the risk of complications. These may include treatments to regulate the heartbeat, reduce fluid retention, or lower the risk of blood clots, depending on each patient’s clinical assessment.
Surgical treatment (open heart surgery)
Surgical treatment is the primary option for certain cases of atrial septal defect, particularly when the defect is large or cannot be closed via catheterization. This includes some primary defects, venous sinus defects, and coronary sinus defects. In these cases, open-heart surgery is performed, in which the heart is accessed through a chest incision to directly repair the defect using sutures or a specialized patch attached to the atrial septum.
This type of surgery is performed under general anesthesia and requires the use of an artificial heart and lung machine during the procedure. Although surgery is more invasive than catheterization, it is an effective and definitive treatment for cases unsuitable for non-surgical therapy. After the procedure, the patient requires a longer recovery period and several days of hospitalization, with regular medical follow-up to ensure that the heart has healed and cardiac function is stabilized.
Catheter closure of atrial septal defect
Catheter closure is a modern and minimally invasive treatment option, particularly suitable for certain types of defects. The procedure is characterized by a quick recovery and short hospital stay, making it a preferred option for many patients when the proper medical conditions are met.
How to close an atrial septal defect with catheterization
Catheter closure of an atrial septal defect is a modern, minimally invasive treatment option suitable for certain defect types. The procedure is performed in Turkey at specialized cardiology centers, resulting in less pain and faster recovery than open surgery.
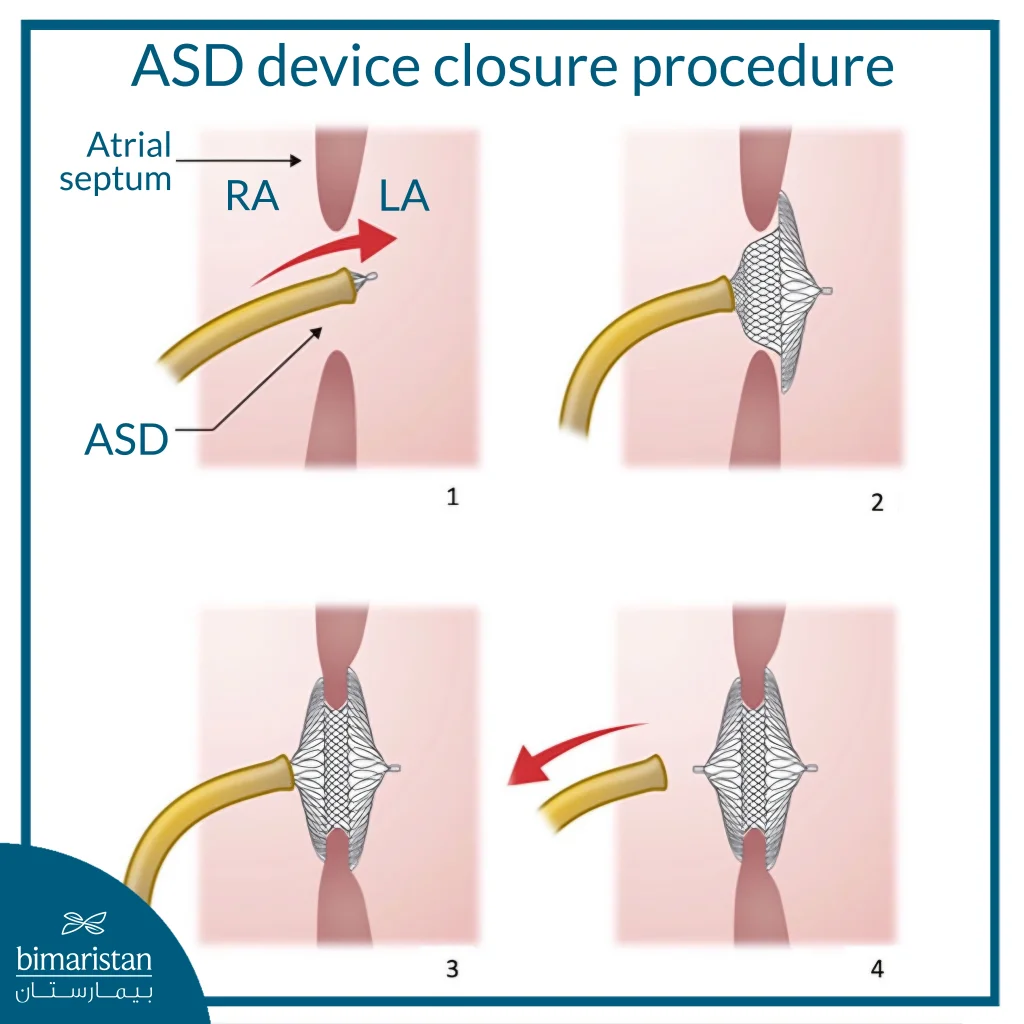
The process of closing an atrial septal defect with a catheter goes through several key steps, including:
- Preparation and anesthesia: The procedure is usually performed under general anesthesia or with sedation, depending on the patient’s condition and the medical team’s assessment.
- Catheter insertion: A thin, flexible tube is inserted through a blood vessel, often in the groin area, and then precisely guided to the heart using advanced imaging techniques.
- Accessing the site of the defect: The catheter is advanced to the atrial septal defect site, and its size and location are assessed during the procedure.
- Installing the closure device: A customized device is placed within the atrial septum and secured to close the defect.
- Finalization of the procedure and initial follow-up: After confirming that the closure device is stable, the catheter is removed, and the patient is monitored for a short period of time in the hospital.
The procedure often takes a short time and requires only a limited hospital stay, often as little as one day in many cases, with a gradual return to daily activities within a short period of time.
Catheter atrial septal defect closure results and post-treatment follow-up
The recovery period after closure of an atrial septal defect varies with the treatment method used, but most patients experience a smooth recovery with adherence to medical instructions and regular follow-up. However, catheter closure is faster compared to open surgery, with the possibility of returning to daily activities within a short period.
Recovery and return to activity
After catheter closure, most patients can resume normal activity in about one week, avoiding heavy physical exertion for the first few days. In the case of open surgical closure, the recovery period may take longer, and physical activity may be restricted for several weeks.
Medications after the procedure
After catheter closure, you may be required to take anticoagulants to prevent blood clot formation for up to six months. Antibiotics, especially before medical or dental procedures, may also be prescribed during the first few months after the procedure to prevent heart infections.
Medical follow-up after treatment
Regular follow-up is an essential part of successful treatment. Your doctor will conduct regular check-ups to ensure the procedure is effective and your heart is healthy, which may include:
- Echocardiography
- Electrocardiogram (ECG)
- Mobile heart rhythm monitors
- Exertion tests, when needed
Post-procedure follow-up in children
After closing a pediatric atrial septal defect with a catheter, the child stays in an observation room for several hours, where vital signs such as heart rate and breathing are monitored. The child may be asked to lie flat without bending the legs for a few hours to reduce the risk of bleeding. Hospitalization is usually required for at least one day, with follow‑up checks performed before discharge.
At home, it is recommended to temporarily avoid strenuous activities, follow prescribed medications, and attend scheduled medical visits. If abnormal symptoms appear, such as increased swelling, bleeding, or fever, the doctor should be contacted immediately. In the short term, the child needs regular follow‑up with the cardiologist, and later these visits become less frequent.
Atrial septal defect is a heart condition that can be effectively managed when diagnosed early, particularly due to advancements in catheter closure techniques. These improvements have led to better treatment outcomes and shorter recovery times for suitable patients. Bimaristan Medical Center helps individuals access specialized evaluations and treatment options through advanced cardiac centers.
Sources:
- British Heart Foundation. (2023, December 14). Atrial septal defect. British Heart Foundation.
- Johns Hopkins Medicine. (n.d.). Atrial septal defect transcatheter repair for children. Johns Hopkins Medicine.